Boosting GABA: Natural Support for Anxiety and Low Mood This Winter
Boosting GABA: Natural Support for Anxiety and Low Mood This Winter
By Patrick Holford

Boost gaba naturally this winter. For many people, the darker months are when anxiety creeps up and mood dips. Shorter days, colder weather and more indoor time often leave the nervous system running on empty. Yet winter does not have to feel this way. Once you understand what is happening in your brain, you can support it with simple, effective tools that help you stay calm, steady and more resilient.
Why alcohol and cannabis feel calming: the GABA effect
How these substances create short term calm
When anxiety builds, many people instinctively reach for something to take the edge off. In one ordinary week in the UK, around 10 million tranquilliser pills are taken, 10 million cannabis joints are smoked and 120 million alcoholic drinks are consumed.
These substances all act on the same calming messenger in the brain: GABA, short for gamma aminobutyric acid. GABA is your neurological dimmer switch. It helps turn down adrenaline, settles the nervous system and makes you feel relaxed and more sociable. A drink or a joint can temporarily boost GABA and give you that familiar sense of relief.
Why the calming effect backfires
The problem comes shortly afterwards. GABA rises, then dips. Once levels fall, irritability, low mood and cravings follow, pushing people towards another drink or smoke. Alcohol also disrupts dreaming sleep which is essential for mental rejuvenation. The result is that you wake tired, flat and anxious with GABA still suppressed and the body working hard to detoxify last night’s alcohol.
Over time, alcohol raises anxiety rather than reducing it. Cannabis, used habitually, tends to lower drive and motivation while offering the same short-lived GABA response.
The good news is that you can support your GABA system in ways that build resilience rather than deplete it.
Natural ways to boost GABA and restore calm
GABA and taurine supplements
GABA is both a neurotransmitter and an amino acid. Supplementing it can help support healthy GABA activity in the brain, offering a gentle, natural way to unwind. In the UK it is regulated as a medicine so you cannot purchase it, though it remains easily available online in other countries. Several natural calming formulas include taurine and glutamine which help the body boost GABA production.
If using GABA directly, most people benefit from 250 to 500 mg once or twice a day. It is not addictive. Higher doses can cause nausea, vomiting or a rise in blood pressure, especially above 3 g a day. Taken in the evening it can also support sleep.
Taurine is structurally and functionally similar to GABA and helps settle the stress response. Despite its inclusion in energy drinks, taurine is not a stimulant. Research shows taurine supplementation slows key markers of ageing (2). It is richest in animal foods, so vegetarians may be more prone to low levels. A typical supportive dose is 500 to 1,000 mg twice daily.
B vitamins and vitamin C for steadier mood
Several B vitamins, especially vitamin B6, are tightly linked to how efficiently your body produces GABA. A recent trial found that 100 mg of B6 reduced self-reported anxiety (3). A large-scale study found women with higher vitamin B6 intake had lower depression and anxiety risk (4). Combined B vitamins also correlate with lower levels of both stress and mood disorders (5).
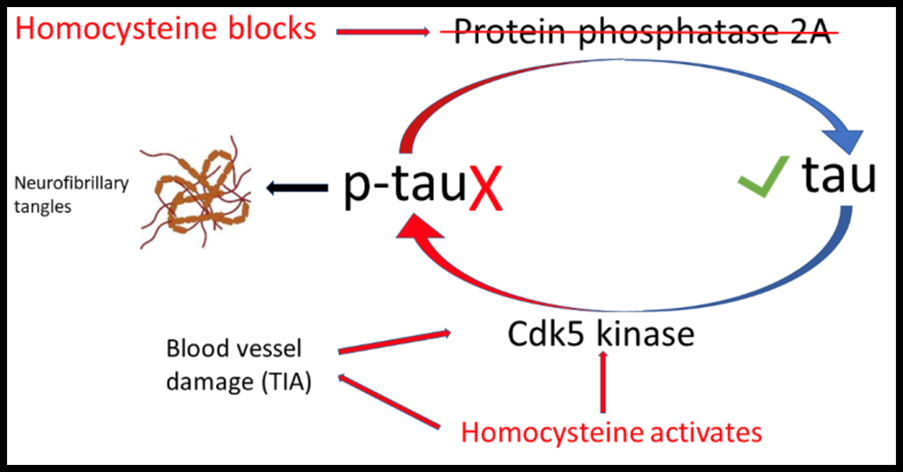
B6 is part of the same biochemical pathway that keeps homocysteine in check. When homocysteine rises, methylation slows and the brain becomes more vulnerable to low mood and anxiety. Keeping this pathway supported can make a meaningful difference. If you are curious about your levels, homocysteine is included in the DRIfT test.
Another review concluded that B6, magnesium and essential fatty acids can reduce anxiety and blood pressure responses to stress, particularly in women (6).
Vitamin C also plays an important role in stress resilience. It sits alongside cortisol in the adrenal cortex and rises in the bloodstream during stress. Since humans, unlike most animals, do not produce vitamin C internally, low intake can heighten vulnerability to stress. Several trials show vitamin C supplementation reduces anxiety and boosts mental vitality (7, 8). Earlier work from the 1970s showed that intakes above 400 mg reduced fatigue (9).
Calming herbs: valerian, hops and passionflower
Valerian (Valeriana officinalis) is a well-established natural relaxant used for restlessness, nervousness and insomnia. It enhances GABA receptor activity and can help boost GABA in a gentle way that supports deeper relaxation. Typical amounts are 50 to 100 mg twice daily, with double that amount before bed if sleeplessness is an issue. Valerian should not be combined with sedative medication or alcohol and not taken without medical guidance.
Hops (Humulus lupulus) has been used historically for sleep and nervous tension. It acts directly on the central nervous system and is most effective when combined with valerian or passionflower.
Passionflower (Passiflora incarnata) offers gentle calming support, promotes sleep and has no known side effects at normal doses. Around 100 to 200 mg a day is typical. It is also thought to be useful for children who struggle to settle. For those who want to avoid excessive drowsiness, hops and passionflower used without valerian may be preferable.
Magnesium to relax body and mind and to help boost GABA pathways
Magnesium supports muscle relaxation, nerve function and mood. Diets high in sugar, refined foods, calcium rich dairy, caffeine and alcohol may lead to depleted magnesium status. Too much calcium relative to magnesium can contribute to muscle tension, nervousness, insomnia and irregular heartbeat.
Magnesium also helps stabilise blood sugar and works alongside B6 and zinc in stress regulation. Several trials show that magnesium, especially combined with B6, reduces anxiety and depression within weeks (10, 11).
Most people would benefit from around 300 mg from supplements, alongside a diet rich in vegetables, nuts, seeds and whole foods. Seeds, nuts, beans and leafy greens provide very good levels.
Theanine: why tea feels calming
Tea delivers caffeine but never feels as jittery as coffee. That is because tea naturally contains L-theanine, an amino acid that increases alpha wave activity associated with relaxed alertness (13). Around 50 mg can noticeably shift the nervous system into a calmer state. Supplements that combine theanine with GABA can can boost gaba effects even further (14).
Balance blood sugar to reduce anxiety physiology
Alongside supporting neurotransmitters like GABA, keeping blood sugar steady is one of the simplest ways to reduce anxiety. When glucose drops, the body releases adrenaline and cortisol to raise it again, which can create sudden waves of anxiety, shakiness and irritability. Research shows that unstable glucose control increases stress reactivity and mood volatility, while balanced meals with protein, fibre and lower GL carbohydrates help stabilise both blood sugar and mood (15). This is particularly relevant in winter, when comfort eating, irregular routines and higher sugar intake are more common.
Support omega 3 levels for calmer mood and boost GABA function
Another key factor underpinning calmness is omega-3 status. EPA and DHA play an essential role in how flexible and responsive brain cell membranes are, which directly affects how well GABA and serotonin receptors function. Keeping omega three levels optimal helps the brain boost GABA signalling more effectively.
Several clinical studies show omega-3 supplementation can lower symptoms of anxiety and improve overall mood stability, especially in those with low baseline levels (16). Since omega-3 cannot be produced in meaningful amounts by the body, keeping levels optimal makes a measurable difference to stress resilience.
If you are unsure of your status, then order your DRIfT blood test to find out – available globally.
Top up vitamin D for winter mood resilience
Winter is also the time when vitamin D levels typically fall, and low vitamin D has repeatedly been linked with lower mood, poorer stress tolerance and greater anxiety. A large meta analysis found that adults with low vitamin D were significantly more likely to experience depression, and supplementation helped improve mood in those who were deficient (17). Vitamin D also influences serotonin production and inflammation, two pathways that strongly affect how the brain responds to stress. Checking levels during winter and supplementing if needed is a simple step with meaningful impact.
A notes on panic attacks, lactic acid and the breath
Panic attacks can be terrifying, with palpitations, rapid breathing and a sense of impending doom. While psychological factors play a role, there can be a biochemical layer too. High levels of lactic acid can drive symptoms. When breathing becomes fast and shallow, carbon dioxide drops and lactic acid rises, which can quickly trigger an anxiety surge.
Breathing slowly into a paper bag or through cupped hands can help restore balance by raising carbon dioxide and reducing lactic acid. Keeping blood sugar stable by eating regularly also helps prevent abrupt dips that can trigger hyperventilation.
A systems based approach to boost GABA and reduce anxiety
Anxiety rarely comes from one place. Biology, psychology, sleep, nutrients, hormones, blood sugar and daily habits all interact, which is why a systems based approach often works best. Supporting several of these pathways at once helps the nervous system become steadier and more resilient, especially in winter when stress loads tend to rise. When you strengthen blood sugar balance, reduce stimulants, restore nutrient status, improve sleep and use targeted herbs, you naturally boost GABA and shift the whole stress response.
Next steps:
- Read more about sugar and brain health here.
- Take the free Cognitive Function Test to understand your personal profile.
- Explore the DRIfT test to join our research and check key nutritional and metabolic markers linked to mood and cognitive health.
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
3 Field DT, Cracknell RO, Eastwood JR, Scarfe P, Williams CM, Zheng Y, Tavassoli T. High-dose Vitamin B6 supplementation reduces anxiety and strengthens visual surround suppression. Hum Psychopharmacol. 2022 Nov;37(6):e2852. doi: 10.1002/hup.2852. Epub 2022 Jul 19. PMID: 35851507; PMCID: PMC9787829.
4 Kafeshani M, Feizi A, Esmaillzadeh A, Keshteli AH, Afshar H, Roohafza H, Adibi P. Higher vitamin B6 intake is associated with lower depression and anxiety risk in women but not in men: A large cross-sectional study. Int J Vitam Nutr Res. 2020 Oct;90(5-6):484-492. doi: 10.1024/0300-9831/a000589. Epub 2019 Jun 11. PMID: 31188081.
5 Mahdavifar B, Hosseinzadeh M, Salehi-Abargouei A, Mirzaei M, Vafa M. Dietary intake of B vitamins and their association with depression, anxiety, and stress symptoms: A cross-sectional, population-based survey. J Affect Disord. 2021 Jun 1;288:92-98. doi: 10.1016/j.jad.2021.03.055. Epub 2021 Mar 26. PMID: 33848753.
6 McCabe D, Lisy K, Lockwood C, Colbeck M. The impact of essential fatty acid, B vitamins, vitamin C, magnesium and zinc supplementation on stress levels in women: a systematic review. JBI Database System Rev Implement Rep. 2017 Feb;15(2):402-453. doi: 10.11124/JBISRIR-2016-002965. PMID: 28178022.
7 de Oliveira IJ, de Souza VV, Motta V, Da-Silva SL. Effects of Oral Vitamin C Supplementation on Anxiety in Students: A Double-Blind, Randomized, Placebo-Controlled Trial. Pak J Biol Sci. 2015 Jan;18(1):11-8. doi: 10.3923/pjbs.2015.11.18. PMID: 26353411.
8 Sim M, Hong S, Jung S, Kim JS, Goo YT, Chun WY, Shin DM. Vitamin C supplementation promotes mental vitality in healthy young adults: results from a cross-sectional analysis and a randomized, double-blind, placebo-controlled trial. Eur J Nutr. 2022 Feb;61(1):447-459. doi: 10.1007/s00394-021-02656-3. Epub 2021 Sep 2. PMID: 34476568; PMCID: PMC8783887.
9 E. Cheraskin et al., ‘Daily vitamin consumption and fatigability’, Journal of the American Geriatrics Society (1976), vol 24(3), pp. 136–137.
10 Noah L, Dye L, Bois De Fer B, Mazur A, Pickering G, Pouteau E. Effect of magnesium and vitamin B6 supplementation on mental health and quality of life in stressed healthy adults: Post-hoc analysis of a randomised controlled trial. Stress Health. 2021 Dec;37(5):1000-1009. doi: 10.1002/smi.3051. Epub 2021 May 6. PMID: 33864354; PMCID: PMC9292249.
11 Tarleton EK, Littenberg B, MacLean CD, Kennedy AG, Daley C. Role of magnesium supplementation in the treatment of depression: A randomized clinical trial. PLoS One. 2017 Jun 27;12(6):e0180067. doi: 10.1371/journal.pone.0180067. PMID: 28654669; PMCID: PMC5487054.
12 Hindmarch I et al, Psychopharmacology, 1998; see also Hindmarch I et al, Psychopharmacology, 2000
13 Nobre AC et al., a report to Unilever by the Department of Experimental Psychology, University of Oxford, 2003; see also Unno K et al, Pharmacol Biochem Behav, 2013
14 Lyon et al, Altern Med Rev, 2011
15 Benton D, Donohoe RT. The effects of nutrients on mood. Public Health Nutr. 1999 Dec;2(3A):403–9.
16 Su KP, Matsuoka Y, Pae CU. Omega 3 fatty acids in mood disorders. J Clin Psychiatry. 2003;64 Suppl 2:32–7.
17 Anglin RE, Samaan Z, Walter SD, McDonald SD. Vitamin D deficiency and depression in adults: systematic review and meta analysis. Br J Psychiatry. 2013 Feb;202:100–7.