Dry January for Your Brain: A Lighter, Clearer Start to the Year
Dry January for Your Brain: A Lighter, Clearer Start to the Year

Dry January arrives with its usual mix of good intentions and side-eye, but beneath the trend is a surprising truth: your brain loves this month more than you think.
That’s because January quietly offers something modern brains rarely get the rest of the year: a drop in oxidative stress and a chance for your natural repair systems to catch up. It’s a pause that lowers the background “noise” created by alcohol and allows your natural calming chemistry to rise back to the surface.
Many people start Dry January thinking about their liver or their waistline. But the strongest benefits often happen behind the scenes, in the place that governs mood, memory, sleep, and stress resilience.
That’s where the real benefits begin to show.
Dry January for Your Brain: Why the Benefits Show Up So Fast
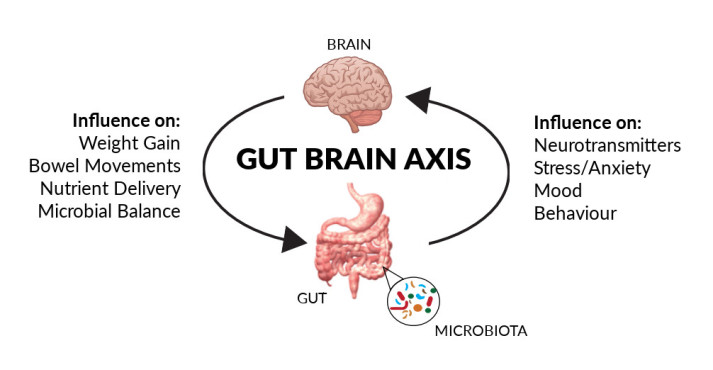
Alcohol works on the same calming pathway your brain uses to wind down naturally. It boosts GABA, the neurotransmitter that quietens the nervous system. That lovely “first sip exhale” comes from this temporary GABA boost. You can learn more about GABA here.
But your brain is clever. To compensate, it gradually nudges up adrenaline and turns the GABA dial down. This is why the glass that once relaxed you, can start to make you feel restless or wakeful later in the night.
And there’s more happening beneath the surface:
- Alcohol increases oxidative stress inside neurons, largely because its metabolism produces acetaldehyde. This compound generates reactive oxygen species and increases neuronal damage (1).
- It also places extra pressure on glutathione, the molecule the brain relies on for detoxification and repair. Chronic alcohol exposure is associated with reduced glutathione levels and impaired antioxidant capacity in the brain (2).
- The hippocampus is particularly affected. This memory and mood hub is vulnerable to long term strain, and higher alcohol intake is linked to reduced hippocampal volume even at moderate levels (3).
- Alcohol also disrupts sleep quality, especially REM cycles, which are crucial for cognitive repair. While alcohol initially sedates, it later fragments sleep architecture through a rebound in adrenaline and cortisol.
Read more about how alcohol impacts your brain here.
These are some of the core drivers of long term cognitive ageing. When they ease up, even for a short period, the brain begins to function more cleanly and calmly.
For this reason, so many people report that a couple of no or low alcohol weeks in January give them clearer thinking, steadier mood, and deeper sleep.
Two Brain Friendly Drinks for Your January Wind Down
With that in mind, here are two great recipe options to help you reduce your alcohol intake while still enjoying a wind down ritual. If you want more brain friendly recipes this year, make sure you subscribe to the Upgrade Your Brain Cook App.
The Classic Gin Rickey
Zero alcohol, zero sugar, 100 percent January friendly
Pomegranate–Basil Spritz
Bright, Uplifting and Polyphenol-Rich

Serves: 1
Prep time: 2 minutes
GL per portion: 0 to 1 (negligible, no added sugar)
Ingredients
• 1 measure of alcohol free gin
• Soda water
• Ice
• 6 frozen cranberries
• Mint and or a sprig of rosemary
• Juice of half a lime, plus a slice for garnish
• Optional: a few drops of orange bitters
Instructions
1. Fill a tall glass with ice and scatter in the frozen cranberries.
2. Add the alcohol free gin.
3. Top with soda water.
4. Add the lime juice, a lime slice, and fresh herbs.
5. Swirl gently and enjoy.
It takes 60 seconds to make and tastes like a fresh start.

Serves: 2
Prep time: 5 minutes
GL per portion: 6
Ingredients
• 125 ml pomegranate juice (100 percent, unsweetened)
• 250 ml sparkling water
• Juice of half a lime
• 4 fresh basil leaves
• 2 cucumber ribbons
• Ice
Instructions
1. Add the basil and lime juice to a jug and gently muddle to release the oils.
2. Pour in the pomegranate juice and sparkling water.
3. Stir, add the cucumber ribbons, and serve over ice.
Nutritional highlights
• A natural source of vitamin C, polyphenols, and plant nitrates to support circulation.
• Offers a gentle lift through dopamine supporting compounds found in pomegranate and fresh herbs.
Cook’s notes
Diluting the juice keeps sugars moderate without losing impact. Mint works beautifully in place of basil if you prefer a cooler, sharper flavour.
Want to go deeper?
If you want deeper support for your brain this year, there are three simple steps you can take.
- First, measure the things that matter. The DRIfT 5 in 1 at home blood test gives you a clear picture of the nutritional and metabolic factors that influence long term brain health. It is one of the most effective ways to understand your personal risk and what to do next.
- Second, stay connected to what keeps your brain healthy. Becoming a FRIEND of Food for the Brain gives you ongoing support, events, and guidance grounded in evidence and prevention.
- Third, take the free Cognitive Function Test. It provides an objective snapshot of how your brain is performing right now and helps you track your progress over time.
Food for the Brain is a not for profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index. This allows them to advise you on how to dementia proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References:
- Zakhari S. Overview: how is alcohol metabolized by the body? Alcohol Res Health. 2006;29(4):245-54. PMID: 17718403.
- Das SK, Vasudevan DM. Alcohol-induced oxidative stress. Life Sci. 2007;81(3):177-87. PMID: 17570440.
- Topiwala A, et al. Moderate alcohol consumption as risk factor for adverse brain outcomes and cognitive decline. BMJ. 2017;357:j2353. PMID: 28588063.