
The vagus nerve is a fundamental part of the autonomic nervous system, which is composed of two key branches; the parasympathetic – the branch that allows us to rest, relax, digest and recharge, and the sympathetic – the branch that is responsible for our stress response and survival by controlling functions such as the heart rate, blood sugar and cortisol, which help us get away from a threat quickly and efficiently. The vagus nerve is the parasympathetic nervous system’s primary nerve, which travels from our brain stem down into a large number of organs and tissues such as the gut, the lungs and the heart. This is why this nerve was coined ‘vagus’, which is latin for ‘wandering’, due to its far-reaching effects on so many parts of the body.
A healthy parasympathetic nerve response, which is governed by the vagus nerve, is essential for our mental wellbeing and physical health. This is because when we are functioning from a parasympathetic ‘point of view’, we are able to repair, digest and assimilate nutrients in our food properly and regenerate. We have evolved to be in this state the majority of the time, however, due to the pressures of modern life and chronic stress, many of us are continuously in a sympathetic state, where we are constantly in a physiological ‘fight or flight’ mode. Stress is a major risk factor for all health conditions and emerging research is showing that it is also a fundamental driver of many of today’s chronic diseases, such as heart disease, diabetes and irritable bowel disease.
Poor mental health such as depression, anxiety, panic attacks and insomnia, are symptoms of a dysregulated nervous system, where our response to environmental stressors have, in essence, become either excessive, causing panic, anxiety, hypervigilance and aggression, or downregulated to the point where we experience symptoms of apathy, depression and sometimes even catatonia. These are all symptoms of poor vagus nerve function, which are often a result of environmental factors such as stressful situations and trauma.
We know that the vagus nerve is connected to the gut and plays a crucial role in modulating the enteric nervous system, which is a complex network of nerves that are located in the wall of the upper intestinal tract. This is a nervous system that is able to function entirely on its own, away from the central nervous system, which is composed of the spinal cord and the brain. Scientists have labelled it the ‘second brain’ due to its independent nature and its ability to communicate with the brain, which is where the vagus nerve comes into play. The vagus nerve is essentially the ‘bridge’ between the brain and the gut, facilitating a bi-directional communication between the two organs.
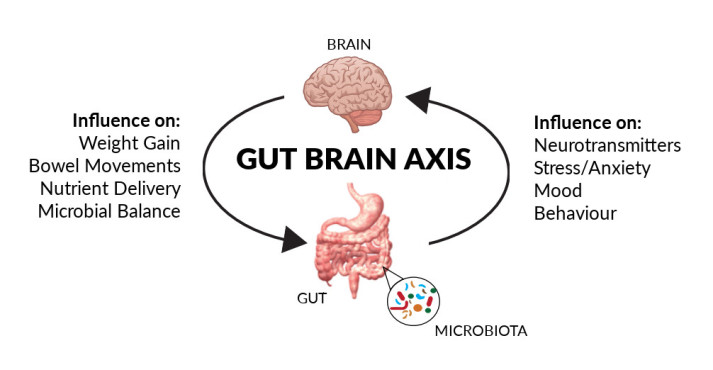
ref: https://lifeverchanging.com/2018/01/25/is-ibs-a-gut-brain-microbiome-axis-disorder/
As you can see in the diagram above, this two-way communication has a variety of functions, which not only influences the emotional wellbeing of a person, but also key physical processes such as digestion and metabolism. A crucial part of facilitating this communication and maintaining a healthy vagus nerve is the microbiome – the bacteria that live in the digestive system. In the past decade, research has exploded in this area, where scientists have begun to unearth how microorganisms such as bacteria, yeast and fungi impact the production and functioning of neurotransmitters and inflammatory processes, which modulate brain activity.
Research shows that eighty percent of the information transmitted by the vagus nerve flows from the body to the brain (afferent nerve fibres). Whereas twenty percent of the vagus nerve is efferent, which means the signals are transmitted from the brain to the body. A clear example of this two-way communication is seen in animal studies, where researchers have found how stress inhibits the signals sent through the vagus nerve and causes gastrointestinal problems. Symptoms such as the suppression of stomach acid and digestive enzyme production, as well as increased gut permeability (leaky gut), slower bowel transit time and nutrient malabsorption are often experienced when under chronic stress. On the other hand, we also see how ‘gut instincts’ or visceral sensations, influenced by external factors such as stressful environments, alert the brain by triggering an emotional response such as fear and anxiety.
In order to support healthy vagus nerve function to optimise mental wellbeing, it is essential to not only practice lifestyle habits that stimulate vagus nerve tone, but also to take care of digestive function.
Here are a number of ways that have been shown to help stimulate the vagus nerve and parasympathetic nerve activity:
Healthy gut bacteria help to create signalling molecules, which are communicated via the vagus nerve to the brain and keep inflammation at bay. Bacteria are also capable of creating neurotransmitters such as serotonin and dopamine. Eating fermented foods such as sauerkraut and kimchi (both fermented vegetable mixes) that are rich in beneficial bacteria, help to maintain equilibrium in the gut. In addition, eating a wide variety of vegetables and fruits can help to provide prebiotic fibres for bacteria to break down, which provides them the essential fuel they need to maintain themselves and create the metabolites that positively influence brain function.
Whilst breathing is part of our autonomic nervous system (meaning that it is a process that happens automatically, without the need for us to think about it) it is also a process that we can control. Deep belly breathing, and in particular, the lengthening of the exhale, can have an immediate impact on the nervous system, stimulating the vagus nerve and therefore the parasympathetic response. One of the easiest and most accessible breathing techniques is the box breathing exercise, which can be followed below:
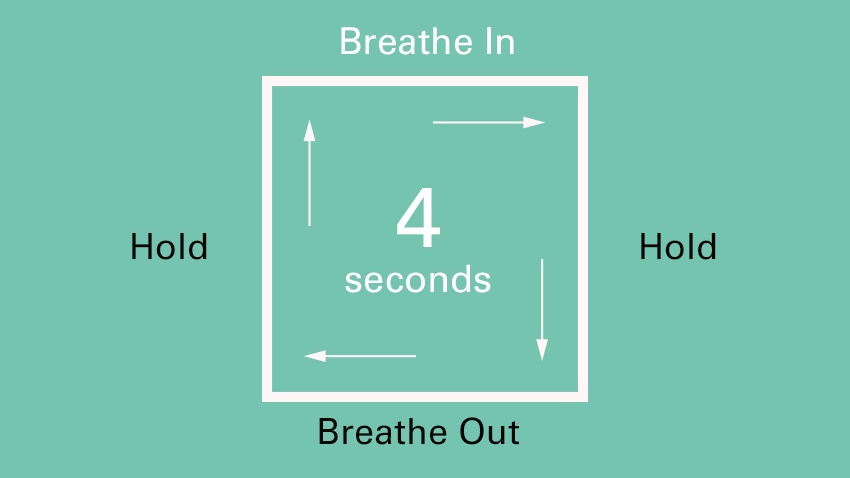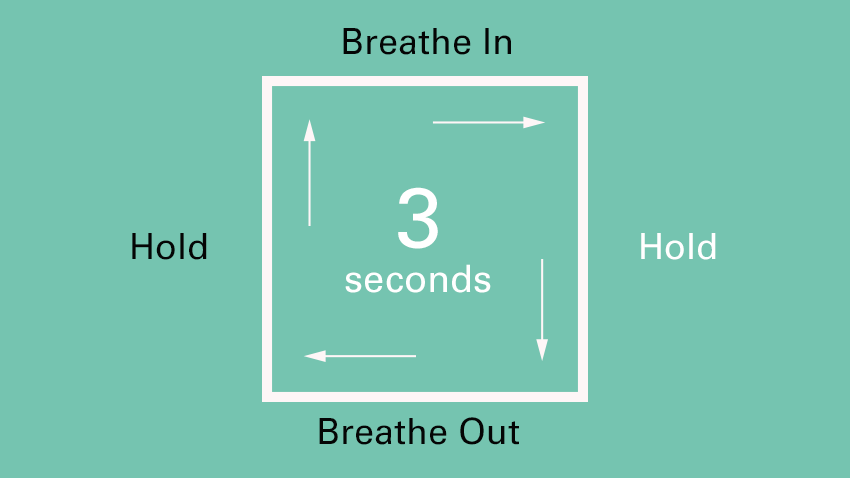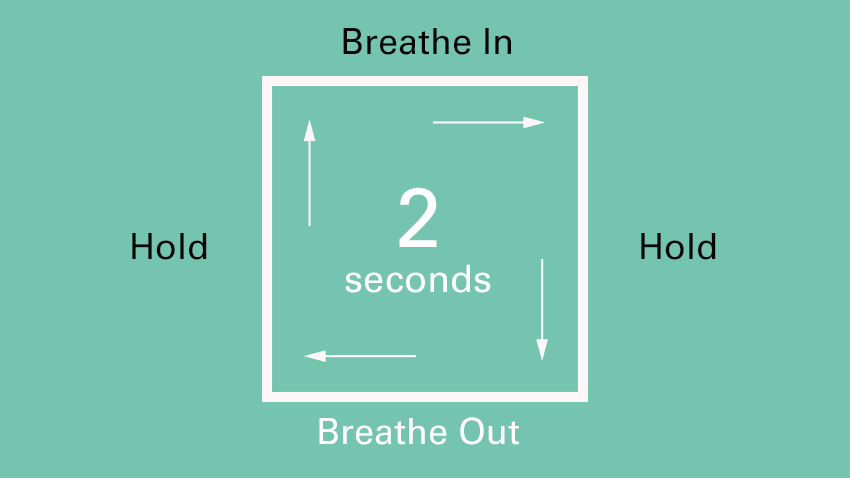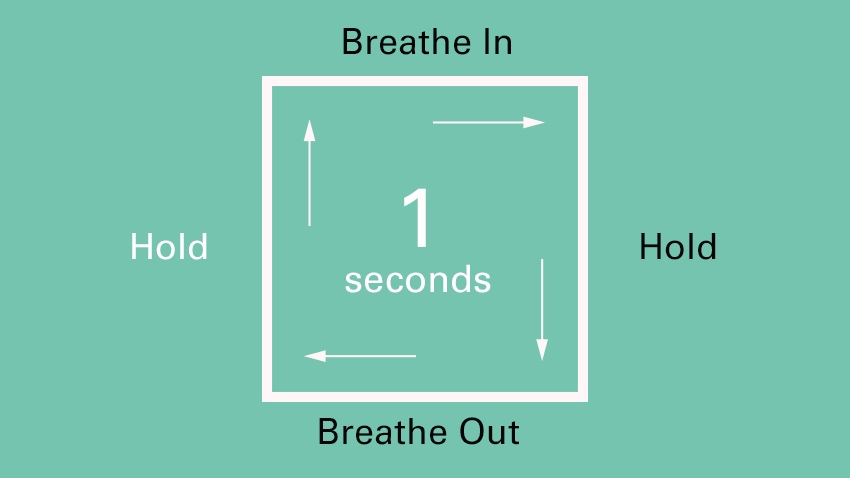
Both gargling and singing mechanically stimulate the vagus nerve by vibrating the muscle fibres at the back of the mouth in the throat area. Due to part of the vagus nerve being located in this area, activities such as gargling can directly stimulate and fire the nerve fibres in the vagus. Practicing these activities on a daily basis can help to improve vagus nerve tone, which may have been lost due to chronic stress and trauma.
Craniosacral therapy directly addresses the cranial nerves (the vagus nerve is the 10th cranial nerve) and helps to shift the body out of a fight or flight state. Over time this can help to ‘rewire’ the nervous system by increasing vagal tone and allowing the balance between sympathetic and parasympathetic to reach a healthy equilibrium.
We know that meditation and mindfulness can be great health tools, especially due to the positive effect they can have on the nervous system. However, loving kindness meditation goes a step further by encouraging visualisation that generates ‘warm and fuzzy’ feelings of compassion and gratitude. This type of meditation is rooted in Buddhist tradition and seeks to promote four key experiences of friendliness, compassion, gratitude and equanimity. Studies have shown that practicing this type of meditation not only improves vagus nerve tone, but also significantly reduces symptoms of depression in those with PTSD and helps to increase social connection.
Here is a great guided loving kindness meditation, which you can try out:
Sign up to our mailing list
Receive educational articles and latest information on events, campaigns and research