The Midlife Biomarker Proven to Drive Alzheimer’s – And How to Bring It Down
The Midlife Biomarker Proven to Drive Alzheimer’s – And How to Bring It Down

It is the only measurable Alzheimer’s risk factor where lowering it has been shown to slow the disease process itself. When homocysteine rises, the brain shrinks faster. When it is lowered with the right nutritional support, shrinkage slows and thinking skills stabilise [1][3][4].
Yet despite decades of evidence, most people have never been told to test it. Most health systems never mention it at all.
This matters because homocysteine begins to rise years before symptoms develop. It gives us a glimpse into the future health of the brain long before memory changes appear. And midlife is the moment where this shift becomes easiest to detect and easiest to change. Far from being the start of inevitable decline, it is a powerful opportunity for prevention.
What Is Homocysteine and Why Does the Brain Care?
Homocysteine is a natural amino acid produced during methylation, the process the body uses to build and repair cells, process toxins, create neurotransmitters and maintain healthy brain tissue. When methylation runs smoothly, homocysteine stays low. When the system struggles, homocysteine rises.
Elevated homocysteine affects the brain in several ways:
• It accelerates shrinkage of the hippocampus, the brain’s memory centre [3].
• It increases oxidative stress and inflammation [1].
• It injures small blood vessels, increasing microvascular damage seventeen-fold [2].
• It disrupts the formation of neuronal membranes [1].
These are not abstract processes. They are part of the biology that leads to cognitive decline.
Homocysteine is therefore both a predictor and a causal contributor to these mechanisms. Scientists use the word causal when lowering a factor has been shown to change the underlying disease process. Homocysteine meets this definition because reducing it slows brain shrinkage and slows cognitive decline, which no amyloid-targeting drug has yet achieved [1][3][4].
Why Homocysteine Is a Causal Alzheimer’s Risk Factor
A causal relationship in medicine is established when different kinds of evidence all point in the same direction. Homocysteine fulfils these criteria in a way no other Alzheimer’s biomarker has been shown to do in human intervention trials
Large population studies show that higher homocysteine levels predict faster cognitive decline and a greater risk of dementia [6][10]. These relationships are consistent, and they follow a clear pattern: the higher the level, the faster the decline.
Researchers also understand why this happens. Homocysteine places strain on the brain in multiple ways. It injures the lining of small blood vessels, increases oxidative stress, disrupts methylation and accelerates the atrophy characteristic of Alzheimer’s disease [1][2].
But the strongest evidence comes from intervention. In the Oxford trials, people with raised homocysteine who were given vitamin B6, B12 and folate experienced a remarkable slowing of brain shrinkage. In those with sufficient omega 3, the reduction in atrophy reached up to 73 per cent [3]. Cognitive decline slowed or even stopped for many participants [4]. When changing a factor changes the outcome, that factor can be considered causal.
This makes homocysteine fundamentally different from more widely discussed markers such as amyloid or p-tau.
Why Homocysteine Rises in Midlife
Homocysteine does not increase because the brain is failing. It rises slowly and quietly in midlife for many reasons that are understandable and often reversible.
During these decades, the body begins to handle nutrients slightly differently, and small shifts in lifestyle or physiology can place more demand on the pathways that keep homocysteine under control.
One of the earliest changes is a gradual reduction in stomach acid that happens in many, which makes it harder for the body to absorb vitamin B12. Many people also take acid-suppressing medication long term, which compounds the issue. At the same time, daily stress tends to increase during these years. Stress uses up B vitamins more quickly, increasing the strain on methylation.
Blood sugar regulation also plays a role. Diets higher in sugar and refined carbohydrates push the body towards insulin resistance, and this metabolic pressure can lift homocysteine levels [8]. Women often face an additional shift: the natural decline in oestrogen during perimenopause. Oestrogen normally supports methylation and antioxidant capacity, so its fall makes the brain more sensitive to nutritional gaps.
There is also the modern reality that many midlife adults eat less oily fish or plant-based omega 3 sources. Without enough DHA, the brain cannot use B vitamins as effectively for repair [5][11]. And for some, medications such as metformin or certain anticonvulsants further deplete essential vitamins.
By themselves, these changes are small. But together (plus others not mentioned), they create a gentle upward drift in homocysteine that can continue for years without noticeable symptoms. The hopeful part is that every single one of these factors is modifiable. Midlife is not a point of no return. It is the moment where small corrections create the greatest long-term benefit.
How Rising Homocysteine Changes the Brain
As homocysteine increases, a series of changes begins to shape how the brain functions long before any formal diagnosis is made.
MRI studies show that higher homocysteine is linked with faster atrophy in regions most affected in Alzheimer’s disease, particularly the hippocampus [3]. This shrinkage is not sudden. It reflects long-term strain on neurons and on the methylation pathways the brain relies on to repair itself.
Homocysteine also affects the brain’s vascular system. It damages the delicate lining of small blood vessels, increasing the likelihood of microvascular injury and transient ischaemic events [2]. These events are often too small to be noticed clinically, yet they can gradually reduce mental clarity, processing speed and resilience.
Another important effect is its influence on neurotransmitters. Methylation is essential for producing dopamine, serotonin and acetylcholine, which underpin mood, motivation and memory. When methylation slows, people often describe feeling foggy, flat or less emotionally steady. Although this article focuses on Alzheimer’s processes, the effects of raised homocysteine reach far beyond memory alone.
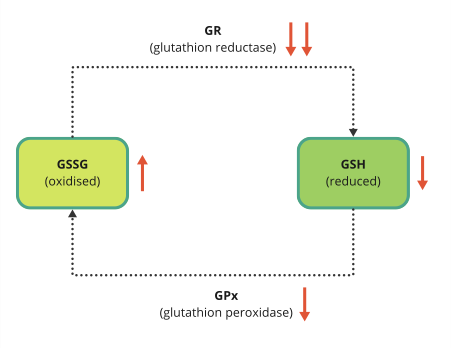
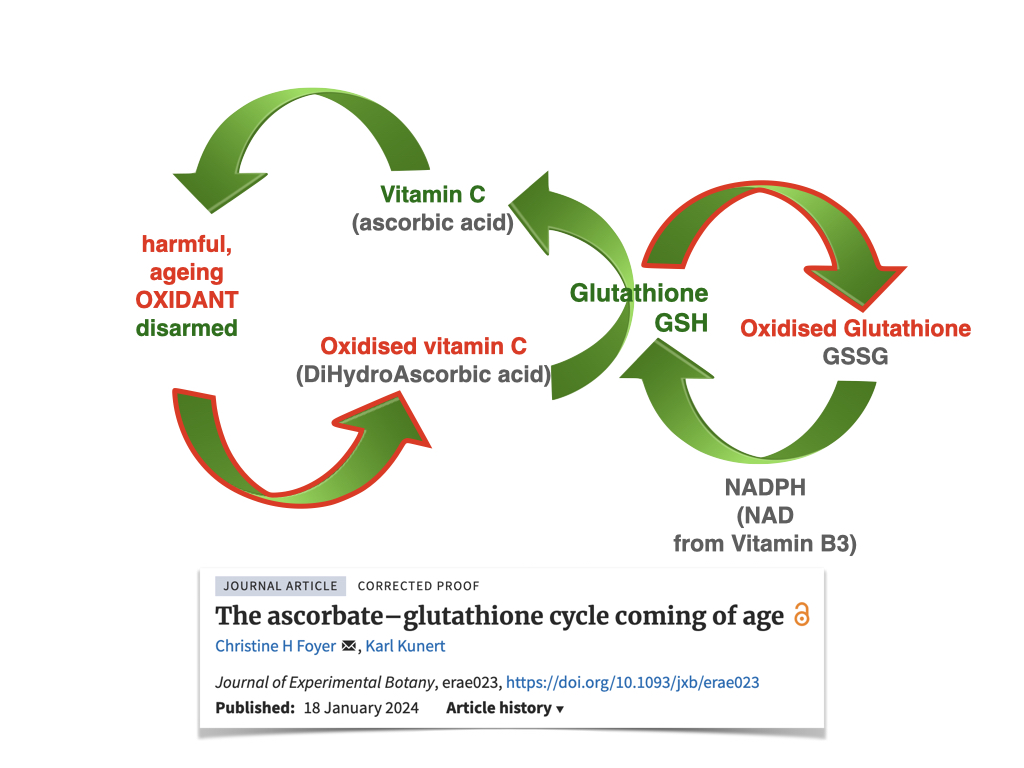
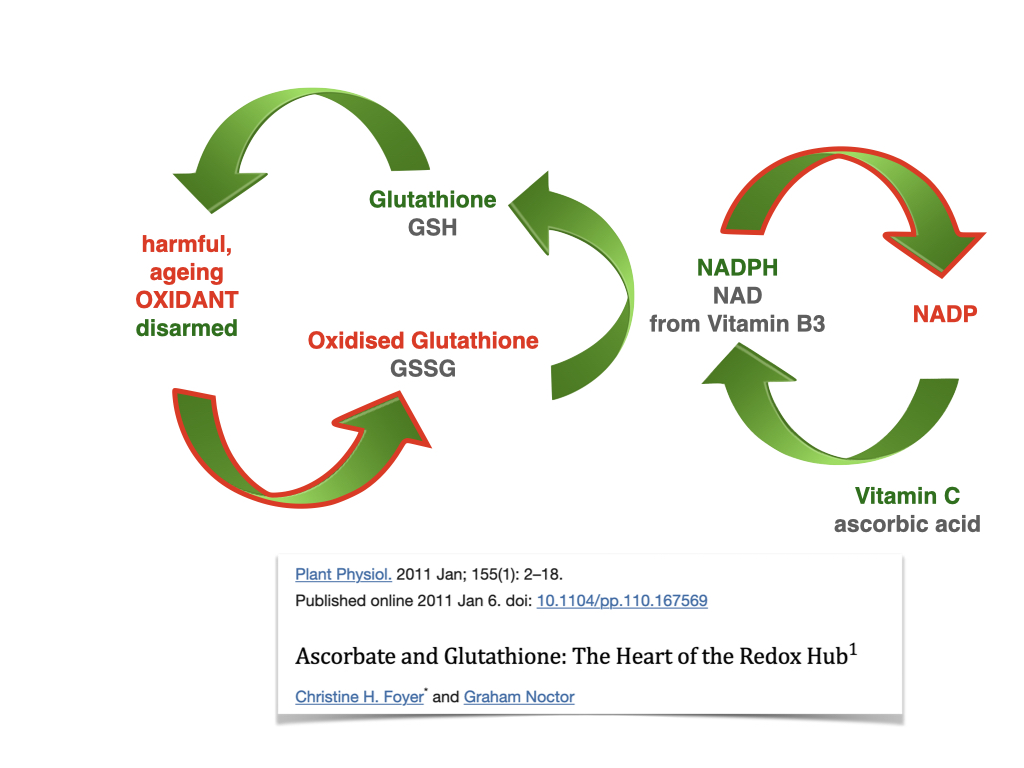
All of this is amplified by increased oxidative stress, which makes the brain more vulnerable to inflammation and everyday wear and tear. This combination of structural, vascular and chemical changes explains why midlife is often the first time people notice subtle shifts such as word-finding pauses, irritability, lower stress tolerance or difficulty multitasking. They are small clues that the brain’s repair systems are under pressure, long before disease takes hold.
Learn more about oxidative stress in the video below:
The Omega 3 Link: Why B Vitamins Work Better Together
One of the most striking discoveries in homocysteine research is how closely it interacts with omega 3 fatty acids. The brain is structurally rich in DHA, the omega 3 found in oily fish, and it depends on DHA to build and maintain healthy neuronal membranes. B vitamins play a crucial role here because they enable DHA to be incorporated into the phospholipids that make up these membranes.
When DHA levels are low, the brain cannot carry out this repair process efficiently, which means B vitamins have far less impact on slowing cognitive decline. But when DHA is sufficient, the picture changes. In clinical studies, the combination of high DHA and adequate B vitamins produced the greatest reduction in brain shrinkage, particularly in areas vulnerable to Alzheimer’s pathology [5][11]. This synergy is one of the clearest examples of how nutrients work together, rather than in isolation, to support long-term brain health. This is why the Food for the Brain DRIfT test measures both homocysteine and the omega 3 index. These markers do more than signal different aspects of nutritional need. They interact in a way that shapes the brain’s ability to repair itself, making them essential parts of an effective prevention strategy.
What You Can Do: How to Lower Homocysteine Safely
The hopeful part of this story is that homocysteine is one of the simplest biomarkers to measure and improve.
1. Measure it
Optimal levels are generally between 6 and 8 micromoles per litre. Order your at home test here – available internationally.
2. Increase key nutrients
Homocysteine is lowered by vitamin B6, folate, vitamin B12 and choline [1][9]. These nutrients can be supplemented and are found in foods such as leafy greens, eggs, lentils, beef, salmon, chickpeas and nutritional yeast. Many people benefit from targeted supplementation: read more here.
3. Support omega-3 intake
DHA from oily fish or algae helps the brain use B vitamins effectively [11].
4. Reduce sugar and ultra-processed foods
This lowers metabolic stress and improves methylation [8].
5. Address underlying factors
Gut health, stomach acid, hormonal changes and medication use all play a role.
Together these simple changes create powerful momentum. Midlife becomes a decade of opportunity rather than ‘inevitable’ decline.
Homocysteine gives us one of the clearest signals of how the brain is ageing long before symptoms appear. It rises for understandable, reversible reasons and responds quickly to targeted support. More importantly, lowering it has been shown to slow the disease process itself.
This means midlife is not a waiting room for cognitive decline.
It is the moment when we can influence our long-term brain health most powerfully.
Checking homocysteine is one of the simplest and most effective ways to do that.
References:
- Smith AD, Refsum H. Homocysteine, B vitamins and cognitive impairment. Annu Rev Nutr. 2016;36:211-239.
- Smith AD, Refsum H, Bottiglieri T, et al. Homocysteine and dementia: an international consensus statement. J Alzheimers Dis. 2018;62(2):561–570.
- Douaud G, Refsum H, de Jager CA, et al. Preventing Alzheimer’s disease-related gray matter atrophy by B-vitamin treatment. Proc Natl Acad Sci USA. 2013;110(23):9523–9528.
- de Jager CA, Oulhaj A, Jacoby R, et al. Cognitive and clinical outcomes of homocysteine-lowering B-vitamin treatment in mild cognitive impairment. Int J Geriatr Psychiatry. 2012;27(6):592–600.
- Jernerén F, Elshorbagy AK, Oulhaj A, et al. Brain atrophy in cognitively impaired elders: the role of homocysteine and long-chain omega 3 fatty acids. Clin Chem Lab Med. 2015;53(3):435–443.
- Zhang X, Huang Y, Wang Y, et al. Elevated plasma homocysteine levels contribute to increased risk of dementia: a meta-analysis. J Alzheimers Dis. 2016;52(4):1227–1237.
- McCaddon A. Homocysteine and cognitive decline: a vitamin B story. Br J Nutr. 2014;111(2):279–280.
- Smith AD, Refsum H. Can nutrition prevent Alzheimer’s disease? Nutrients. 2021;13(1):1–33.
- Smith AD. B vitamins and the prevention of cognitive decline and dementia. Adv Nutr. 2021;12(5):1836–1844.
- Nurk E, Refsum H, Tell GS, et al. Plasma homocysteine and memory in the elderly. Am J Clin Nutr. 2005;82(3):493–498.
- Oulhaj A, Jernerén F, Refsum H, et al. Omega 3 fatty acids interact with B vitamins in slowing cognitive decline in mild cognitive impairment. Am J Clin Nutr. 2016;103(6):1041–1048.
- Ford AH, Almeida OP. Effect of homocysteine lowering treatment on cognitive outcomes. J Alzheimers Dis. 2019;69(2):443–456.