What Is Homocysteine and Why It Matters for Brain Health
What is homocysteine?
Homocysteine is a naturally occurring amino acid produced as part of the body’s methylation process. The level of it in the plasma is increasingly being recognised as a risk factor for disease. It is also seen as a predictor of potential health problems such as cardiovascular disease and Alzheimer’s. You can learn more about homocysteine, testing, and what healthy levels mean in our main guide on understanding homocysteine.
The complex metabolism of homocysteine within the body is highly dependent on vitamin derived cofactors. Deficiencies in vitamin B12, folic acid and vitamin B6 are associated with raised homocysteine levels. Other factors thought to raise levels are poor diet and poor lifestyle. These include smoking and high coffee and alcohol intake, some prescription drugs (such as proton pump inhibitors), diabetes, rheumatoid arthritis as well as poor thyroid function.
There is no consensus about the upper reference limits for plasma homocysteine concentrations. The ‘normal’ range for healthy individuals is considered to be between 5 and 15 µmol/L. However, levels as low as 6.3 µmol/L are thought to confer an increased risk. Each 5 µmol/L can increase the risk of coronary heart disease events by approximately 20%.
Why testing matters
The good news is that homocysteine levels can be tested. High levels can, in many cases, be normalised through diet and vitamin supplementation. The most important nutrients that help lower homocysteine levels are folate, the vitamins B12, B6 and B2, zinc and trimethylglycine (TMG).
This article explains the causes and impacts of high homocysteine levels and emphasises the importance of measuring them. It also highlights the limitations involved in sample handling and homocysteine testing, and it outlines how vitamin supplementation can help normalise homocysteine levels.
Measurement of Homocysteine
written by Dr Gillian Hart BSc (Hons), PhD, Cert Mgmt (Open), MIBMS
Background
The importance of homocysteine as a risk factor is becoming much more familiar as evidence grows. An increasing number of studies now show that homocysteine predicts potential health problems. It is clear now that raised plasma homocysteine concentrations both predict and precede the development of cardiovascular disease including stroke. A study (published in the British Medical Journal) showed homocysteine level in blood plasma predicts risk of death from cardiovascular disease in older people even better than any conventional measure of risk including cholesterol, blood pressure or smoking.
Raised levels of homocysteine are also linked to Alzheimer’s, dementia, declining memory, poor concentration and judgment and lowered mood. Women with high homocysteine levels find it harder to conceive and are at risk from repeated early miscarriage. High homocysteine has also been linked to migraines. Those with conditions such as diabetes and osteoporosis are at increased risk of raised homocysteine levels. Finally,homocysteine has been shown to play a crucial role as a key marker for disease development. It can even determine longevity and health throughout a person’s lifespan.
Why is homocysteine harmful?
Homocysteine is a naturally occurring amino acid that the body produces during the methylation process. It has the formula C4H9NO2S and appears in blood plasma as a protein derivative when body chemistry is out of balance. A homologue of the amino acid cysteine, differing by an additional methylene (-CH2-) group, it is not obtained from the diet. Instead, it is biosynthesized from methionine via a multi-step process that probably occurs in every cell of the body (Figure 1).
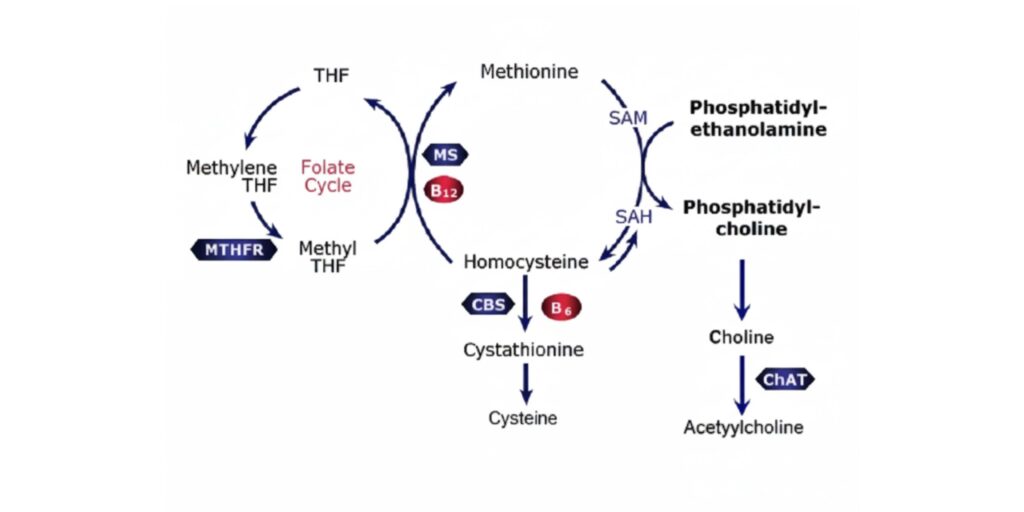
Figure 1: Methionine Metabolism
Methionine is an amino acid, ingested as a component of food protein. It is found primarily in meats, eggs, dairy products, fish, chicken, seeds, nuts and some vegetables. Methionine is activated to S-adenosylmethionine (SAM) by the enzyme methionine adenosyltransferase. Circulating levels of homocysteine are usually low due to its rapid metabolism via one of two pathways:
- a cobalamin (vitamin B12) and folate dependent re-methylation pathway that regenerates methionine
- a pyridoxal 5’ phosphate (PLP, vitamin B6) dependent trans-sulphuration pathway that converts homocysteine into cysteine.
Metabolism
The body relies heavily on vitamin derived cofactors to metabolise homocysteine. When levels of vitamin B12, folic acid or vitamin B6 are low, homocysteine levels rise and hyperhomocysteinaemia can develop. Homocysteine can accumulate in the body causing cell damage and the onset of major disease. The reason is because the biochemical transformation process is not working properly, usually due to lack of these needed vitamins. If these pathways are lacking the required vitamins and minerals, dangerous homocysteine levels and potential ill health can result.
The proposed mechanisms by which hyperhomocysteinaemia can cause harm are common to several conditions. For example, vascular damage, cognitive impairment, neurological complications, congenital defects and pregnancy complications
A detailed review of these mechanisms is outside the scope of this article. However, raised homocysteine is associated with damage to the arteries. One mechanism involves homocysteine interfering with how cells use oxygen, which results in a build up of damaging free radicals. Oxidation triggers many diseases including heart disease, strokes, cancers and autoimmune diseases.
Reactive chemical forms, such as free radicals, can oxidize low-density lipoproteins producing oxy-cholesterols and oxidized fats and proteins within developing arterial plaques. This oxidation injury, along with changes in nitric oxide metabolism, appears to contribute to the damage caused. Researchers suggest that methylation defects and impaired DNA repair caused by disturbed folate metabolism contribute to carcinogenesis.
Nitric oxide is an important regulator and mediator of numerous processes in the nervous, immune and cardiovascular systems, and decreased methylation.
Effects on Arteries and Disease Risk
Homocysteine also stimulates the growth of smooth muscle cells, causing deposition of extracellular matrix and collagen. In turn this causes a thickening and hardening of artery walls. Overall though, the exact mechanisms involved in the increased risk of ill health with raised homocysteine, still remain a mystery in many respects. More studies are needed to elucidate the exact associations.
What causes raised levels?
Many factors are thought to raise levels of homocysteine. Among these are poor diet, poor lifestyle especially smoking and high coffee and alcohol intake.
Additional factors include some prescription drugs, diabetes, rheumatoid arthritis and poor thyroid function as well as with chronic inflammatory diseases in general, and some intestinal disorders such as coeliac and Crohn’s diseases.
Levels increase with age and higher levels are more common in men than women. Levels can also increase with oestrogen deficiency and with some long term medications, including corticosteroids. Strict vegetarians and vegans may also be at risk as well as people who suffer from stress.
As with cholesterol, family history and genetic make-up can play a part in causing raised levels, as can obesity and lack of exercise. Even people with an active, healthy lifestyle may still be at risk, if there is a family history of high levels of homocysteine or disease.
Researchers have identified a rapidly increasing number of variations in the genes that regulate the enzymes involved in methionine metabolism. Reduction in the activity of genes such as the one that regulates the enzyme methyl-enetetrahydrofolate reductase (MTHFR) increases mean homocysteine levels. This gene is present in its homozygous form in about 10% of most European populations. However, the frequency varies widely geographically and between different ethnic populations.
Testing for homocysteine
The measurement of total homocysteine which includes the sum of the concentrations of free and bound homocysteine in the blood plasma, is technologically difficult. After blood sampling, the blood cells produce and release homocysteine. This results in an increase in measured levels of about 10 percent per hour at room temperature. Thus it is vital to follow a specific process within 30 minutes of collection:
Collect blood plasma (using EDTA or heparin to prevent coagulation) and then centrifuge the sample to remove the blood cells from the plasma. Even the most efficient transport from clinic or GP practice to laboratory centrifuge rarely renders this feasible. Collection of blood serum is not appropriate due to the relatively long clotting time required. Once separated from the blood cells the homocysteine is stable in plasma for at least 4 days at room temperature, and much longer refrigerated or frozen.
Some manufacturers now provide blood collection vacutainers, which contain a stabiliser solution that can help delay the urgent need for centrifugation.
Considerations
There are several other important factors to consider when blood sampling. As methionine, ingested as protein in the diet, is the only source of homocysteine, it would be expected that food intake would cause increased concentrations of homocysteine in plasma. A protein rich meal can significantly raise total homocysteine levels, so clinicians generally recommend that the person taking the test should be overnight fasted at the time of blood sampling.
Urine homocysteine measurement is not useful as renal excretion does not seem to be an important route of elimination. Only about 1% of the homocysteine filtered by the glomeruli is normally found in the urine. The rest is reabsorbed and metabolized. In saying that, some GPs do offer urine measurement, as it is easy to collect. However, you should interpret the results with caution because they are likely to detect only extreme hyperhomocysteinaemia.
Test methods
The increased need in clinical chemistry laboratories for methods of homocysteine determination, in correlation with cardiovascular diseases and nutritional deficient status, has led to the development of different analytical methods for measurement.
Methods include amino acid analysis, high performance liquid chromatography (HPLC), capillary electrophoresis, gas chromatography-mass spectrometry (GC-MS) and immunoassay. HPLC is the gold standard reference method. Different total homocysteine measurement methods do usually give comparable results. However, because methods and laboratories vary, you should use caution when comparing values obtained from different laboratories.Studies have shown that single measurements can classify persons with respect to their average plasma homocysteine level quite well. However, because inter-method and inter-laboratory variability can affect results, you should monitor homocysteine concentrations over time using the same method and the same laboratory. Choosing laboratory testing services is thus a critical process.
“Normal” reference ranges
There is no consensus about the upper reference limits for plasma homocysteine concentrations. Among apparently healthy individuals “normal” concentrations commonly range from 5 to 15µmol/L. However, studies on targeted segments of the population have shown that the upper limit of 15µmol/L is far too high in well-nourished populations without obvious vitamin deficiency. It is clear now that each increase of 5µmol/L in homocysteine level increases the risk of coronary heart disease events by approximately 20%, independently of traditional coronary heart disease risk factors. Risk for coronary artery disease increases across a continuum of homocysteine concentrations, with substantial risk appearing between 10 and 15 µmol/L.Some report that any homocysteine measurement over 6.3µmol/L represents an increased risk.
There is little doubt that homocysteine measurement will become a routine screening tool for risk assessment in the future, but that current reference limits will change from being based on values from a presumed normal healthy population towards a baseline where ‘normal’ is the optimum level. Experts recommend carefully monitoring homocysteine levels.
Recommendations
The good news is that many people can normalise high homocysteine levels. Evidence shows that diet and vitamin supplementation effectively reduce plasma homocysteine. It is clear though that vitamin supplementation can normalise levels even when serum vitamin levels are within the normal range, or even in the high range. Metabolic, environmental and genetic factors make it virtually impossible to determine individual nutritional requirements without first carrying out a homocysteine test; the test result can then define the diet and supplementation regime required. The most important nutrients that help lower homocysteine levels are folate, the vitamins B12, B6 and B2, zinc and trimethylglycine (TMG).
Conclusion
This article has provided an overview of the importance of homocysteine measurement, whilst highlighting some of the limitations associated with sample handling and testing. There will always be people who are at high risk of raised homocysteine, but the only way to find out definitively is to perform a validated homocysteine test, and then monitor levels regularly going forwards.
Dr Gill Hart is a Biochemist with over twenty-five years’ experience in the development and evaluation of hospital standard tests and testing services. Gill joined the YorkTest team in 2005, and has applied her scientific and regulatory knowledge to all YorkTest services.
References
1. de Ruijter, W. et al, “Use of Framingham risk score and new biomarkers to predict cardiovascular mortality in older people: population based observational cohort study”. British Medical Journal, 2009, 338: a3083.
2. Seshadri, S. et al, “Plasma homocysteine as a risk factor for dementia and Alzheimer’s disease”. New England Journal of Medicine, 2002, 346:476-483.
3. Rugolo, S. et al, “Hyperhomocysteinemia: associated with obstetric diabetes and fetal malformations”. Minerva Ginecologica, 2005, 57:619-25.
4. Savage, D. et al “Sensistivity of serum methylmalonic acid and total homocysteine determinations for diagnosing cobalamin and folate deficiencies”. American Journal of Medicine, 1994, 96:239-46.
5. Klee, G. “Cobalamin and folate evaluation; measurement of methylmalonic acid and homocysteine vs vitamin B12 and folate”. Clinical Chemistry, 2000, 46:1277-83.
6. Bolander-Gouaille, C. In “Focus on homocysteine and the vitamins involved in its metabolism”. Published by Springer-Verlag, France, 2002, Chapter 3, p33.
7. Upchurch, G. et al, “Homocysteine, EDRF and endothelial function”. Journal of Nutrition, 1996, 126:1290S-1294S.
.
8. Cortelezzi, A. et al, “Hyperhomocysteinemia in myelodysplastic syndromes: specific association with autoimmunity and cardiovascular disease”. Leukemia & Lymphoma, 2001, 41:147-50.
9. Mutus, B et al, “Homocysteine-induced inhibition of nitric oxide production in platelets: a study on healthy and diabetic subjects”. Diabetologia, 2001, 44: 979-82.
10. Duthie, S. “Folic acid deficiency and cancer: mechanisms of DNA instability”. British Medical Bulletin, 1999, 55:578-92.
11. Robertson, K. “DNA methylation, methyltransferases, and cancer”. Oncogene, 2001, 20:3139-55
12. Carmody, B. et al, “”Folic acid inhibits homocysteine-induced proliferation of human arterial smooth muscle cells”. Journal of Vascular Surgery, 1999, 30: 1121-8.
.
13. Majors, A. et al, “Homocysteine as a risk factor for vascular disease. Enhanced collagen production and accumulation by smooth muscle cells”. Arteriosclerosis Thrombosis and Vascular Biology, 1997, 17:2074-81.
14. Bolander-Gouaille, C. and Bottiglieri, T. In “Homocysteine related vitamins and neuropsychiatric disorders”. Published by Springer-Verlag, France, 2003, pp58-108.
15. Rozen, R. “Genetic modulation of homocysteinemia”. Seminars in Thrombosis and Hemostasis, 2000, 26: 255-61.
16. Wilcken, B. et al, “Geographical and ethnic variation of the 677C>T allele of 5,10 methylenetetrahydrofolate reductase (MTHFR): findings from over 7000 newborns from 16 areas world wide”. Journal of Medical Genetics, 2003;40:619-625.
17. European Patent EP1518118
.
18. Rasmussen, K. and Møller, J. “Total homocysteine measurement in clinical practice”. Annals of Clinical Biochemistry, 2000, 37: 627-648.
19. Refsum, H. et al, “Facts and Recommendations about total homocysteine determination: an expert opinion”. Clinical Chemistry, 2004, 50: 3–32.
20. Garg, U. et al, “Short-term and long-term variability of plasma homocysteine measurement”. Clinical Chemistry, 1997, 43: 141-145.
21. Hart, G. “Fundamentals to look for when choosing laboratory testing services”. Nutrition Practitioner, 2008, Spring/Summer.
22. Bolander-Gouaille, C. In “Focus on homocysteine and the vitamins involved in its metabolism”. Published by Springer-Verlag, France, 2002, Chapter 8, p206.
23. Nygard, O. et al, “Major lifestyle determinants of plasma total homocysteine distribution: the Hordaland Homocysteine Study”. American Journal of Clinical Nutrition, 1998, 67:263-70.
.
24. Ubbink, J. et al, “Results of B-vitamin supplementation study used in a prediction model to define a reference range for plasma homocysteine”. Clinical Chemistry, 1995,41:1033-7.
25. Humphrey, L. et al, “Homocysteine level and coronary heart disease incidence: a systematic review and meta-analysis”. Mayo Clinic Proceedings, 2008, 83:1203-12.
26. Robinson, K. et al, “Hyperhomocysteinemia and low pyridoxal phosphate: common and independent reversible risk factors for coronary artery disease”. Journal of Circulation, 1995, 92:2825-30.
27. Holford, P. and Braly, J. (2003) “The H Factor”. Published by Piatkus, UK.
28. Nilsson, K. et al, “Plasma homocysteine in relation to serum cobalamin and blood folate in a psychogeriatric population”. European Journal of Clinical Investigation, 1994, 24:600-6.
29. Faurshou, M. et al, “High prevalence of hyper-homocysteinemia due to marginal deficiency of cobalamin or folate in chronic myeloproliferative disorders”. American Journal of Hematology, 2000, 65: 136-40.

