Snacks: Brain Boost or Brain Drain?

—
In fact, snacking is one of the easiest ways to sabotage your long-term brain health and memory. Most people wouldn’t eat a plate of sugar at mealtimes (unless they start the day with shop-bought cereal or sweetened yoghurt), yet it’s common to reach for a bar, a biscuit, or something from a petrol station or coffee shop without a second thought.
These everyday choices are a silent driver of brain fog, low mood, memory problems – even dementia. It’s time to upgrade your brain by upgrading your snacks. Below, we share a free Brain Boost Bites recipe and some other smart snack ideas – perfect for long drives, picnics, or busy days on the go.
The Problem with Typical Snacks
The modern snack aisle is a minefield of ultra-processed foods: cereal bars, crisps, flavoured yoghurts, granola bites, and biscuits – many of them marketed as “healthy”. But beneath the surface, they’re often:
- High in sugar or refined carbs – causing a rapid blood glucose spike followed by a crash. Many so-called healthy bars contain over 15g of sugar with little fibre, protein, or healthy fat to balance them.
- Low in brain-essential nutrients – such as omega-3s, magnesium, or phospholipids.
- Full of artificial additives – emulsifiers, preservatives, and even excitotoxins like MSG.
- Designed for instant gratification – often with addictive properties rather than sustained energy.
As explained in our Four Horsemen of the Mental Health Apocalypse series (read Part 1 here and Part 2 here), poor glucose control is a key driver of accelerated brain ageing and cognitive decline. A high-sugar snack spikes blood sugar, then causes a crash that reduces brain energy and impairs mental performance. Over time, this rollercoaster leads to insulin resistance, which is strongly linked to cognitive decline and Alzheimer’s disease.
The Smart Snacking Solution
The answer isn’t to stop snacking altogether – it’s to snack smart.
Our in-house chef and lecturer in culinary nutrition and functional health, Kim Close, shares a free recipe below from the Upgrade Your Brain Cook App. It’s packed with brain-supportive nutrients and perfect for keeping your energy and focus steady.
And if you’re not sure what to eat for better brain health, the Cook App includes 120+ recipes (and growing) to guide you meal by meal.
Brain Boost Bites
Refined sugar-free | Fibre-rich | Brain-fat fuelled | Brain Boosting

Ingredients:
- 100g (3½ oz) almonds
- 30g (1 oz) walnuts
- 50g (1¾ oz) goji berries
- 2 tbsp ground flaxseed
- 2 tbsp almond butter
- 1 tbsp raw cacao powder
- 1 tbsp water (if needed for blending)
Method:
- Blend all ingredients in a food processor until the mixture becomes sticky and holds together.
- Roll into small balls.
- Chill in the fridge for at least 30 minutes.
Servings: Makes 10-12 balls
Cook’s Tips: Store in an airtight container in the fridge for up to a week. Add orange zest or vanilla extract for flavour variation.
Other Smart Snack Ideas:
- Oatcakes with almond butter or smoked mackerel pâté
- Olives
- Square of Dark Chocolate Bar (Recipe in Cook App)
- Hummus or nut butter with raw veggie sticks
- A boiled egg with cherry tomatoes
- A handful of walnuts or pumpkin seeds
- A small cup of full-fat Greek yoghurt with blueberries
- Chia pudding made with coconut milk (recipe in the app)
- 2 squares of 85%+ dark chocolate
Snacking wisely is one of the easiest daily upgrades you can make for your brain. And with the right ingredients, it can be delicious too.
New Study: higher choline intake lowers the risk of dementia, Alzheimer’s, & cognitive decline
by Patrick Holford

—
Choline is an often-overlooked but vital nutrient for brain health.
A new study suggests the optimal intake is 400mg, yet there is no Recommended Daily Allowance or widespread promotion of this crucial nutrient. It is also notably low in vegetarian and especially vegan diets.
(We discuss this and more in our COGNITION 6-month brain upgrade programme – available when you become a FRIEND of Food for the Brain.)
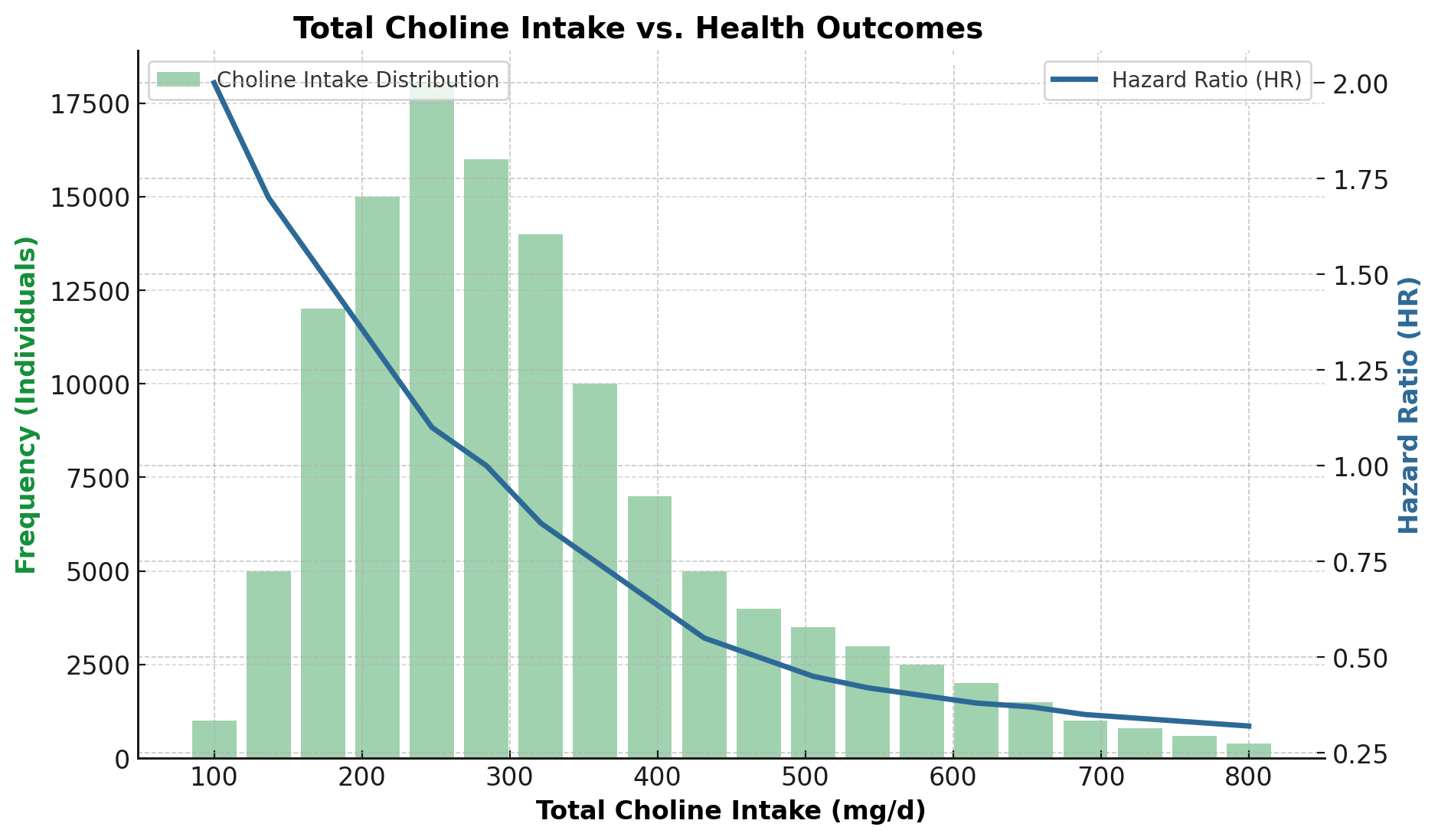
A major study published this year found that higher choline intake lowers the risk of dementia, Alzheimer’s, and cognitive decline.
Researchers tracked 125,000 people from the UK Biobank for 12 years and the study was published in the American Journal of Clinical Nutrition. It showed that higher choline intake reduced risk, with the most benefit around 400mg per day.
__
—
Why does it matter?
Brain cells are made of a membrane containing choline (and other phospholipids) attached to the omega-3 fat DHA. Without choline the omega-3 doesn’t work. The attaching of the two depends on methylation, a process that is dependent on B vitamins, especially B12, folate and B6. Choline helps methylation and healthy methylation, indicated by low homocysteine, helps synthesise choline.
__
–
Also previous studies (2) have found remarkable effects supplementing 480-900mg of choline in pregnancy on promoting ‘smart’ babies with faster reflexes and cognitive processes. It’s important for all ages and a key topic in our Smart Kids & Teens Programme.
What should you do or eat?
Choline is essential for the body, especially the brain, yet it has no Recommended Daily Allowance.
Choline is abundant in eggs, fish, and meat. An egg provides about 120mg, while a 50g serving of beef or salmon contains around 50mg. Beef liver is the richest source, but eggs are the best overall because they contain phosphatidylcholine which is more easily absorbed by the body. Plant-based sources include soy, quinoa, nuts, seeds, beans, and broccoli. A 50g serving of almonds or broccoli provides about 25mg. Phosphatidylcholine, found in lecithin capsules and granules, is an easy supplement option for vegans and vegetarians.
We recommend eating two eggs most days, with a minimum of six per week. Include fish and some meat if you eat it, or soy, quinoa, broccoli, nuts, and seeds if you don’t. Supplementing is likely beneficial, especially for vegetarians. Taking two high-PC lecithin 1,200mg capsules daily provides 250mg of phosphatidylcholine (PC), the form used by the body. These supplements are available at your local health food store.
Remember, your brain is built from what you feed it – and how you use it (as covered in COGNITION). What choline-rich foods can you add to your diet this week?
If you’re unsure what to eat to support your brain or need inspiration, the Cook App is here to help! With over 100 recipes at your fingertips, eating delicious, brain-boosting foods has never been easier—all for just £30 a year.
Actions:
- Take the Cognitive Function Test today – our validated online assessment – to find out exactly what you need to focus on.
- Become a FRIEND and get access to your 6-month COGNITION programme so you know how to upgrade your brain.
–
Food for the Brain is a not-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
—Reference list
Reference
- Niu YY, Yan HY, Zhong JF, Diao ZQ, Li J, Li CP, Chen LH, Huang WQ, Xu M, Xu ZT, Liang XF, Li ZH, Liu D. Association of dietary choline intake with incidence of dementia, Alzheimer disease, and mild cognitive impairment: a large population-based prospective cohort study. Am J Clin Nutr. 2025 Jan;121(1):5-13. doi: 10.1016/j.ajcnut.2024.11.001. Epub 2024 Nov 7. PMID: 39521435.
- Caudill, M. et al, ‘Maternal choline supplementation during the third trimester of pregnancy improves infant information processing speed: a randomized, double-blind, controlled feeding study’ FASEB Journal (Apr 2018); 32(4): 2172-80. doi: 10.1096/fj.201700692RR.
The Mood & Brain Boost: 7 Ways to Ditch the Seasonal Slump

How can we lift our mood and nourish our brain?
Depression, now the leading cause of disability globally, affects millions. According to the World Health Organization, it represents a significant disease burden, particularly in high-income countries (1). With a staggering 100 million antidepressant prescriptions issued annually—a 70% increase in five years—it’s clear that something is going wrong in our modern western world (1).
Thankfully, nutrition and lifestyle changes provide science-backed ways to boost our mood naturally.
(If you want to know more about how to overcome depression then make sure you watch our webinar ‘Finding your way out of depression’).
—
Understanding Depression
Depression manifests through persistent feelings of hopelessness, low energy, disrupted sleep, and even physical changes such as weight loss or gain (2). The root causes can be multifactorial—psychological stress, biochemical imbalances, or nutritional deficiencies.
But here’s the good news: you can take simple, practical steps to nourish your brain, boost serotonin, and improve your mood naturally.
—
7 Ways to Boost Mood and Brain Function
—
1. Increase Your Omega-3 Fats
Your brain is 60% fat, and omega-3 DHA and EPA are critical for its structure and function. Countries with high fish consumption have lower depression rates. A study from Harvard Medical School found that EPA, specifically, has potent antidepressant effects.
A meta-analysis published in Psychopharmacology Bulletin found that higher omega-3 intake reduces depressive symptoms by 53%. Omega-3 helps build brain cell membranes and boosts serotonin receptor function, which improves mood and cognition.
- What to do: Eat oily fish like salmon, sardines, and mackerel at least twice a week or supplement with high-dose omega-3 fish oil. Aim for 1,000–2,000 mg of EPA and DHA combined daily (4, 5, 6).
—
2. Optimise Your B Vitamins and Lower Homocysteine
The little-known amino acid, homocysteine, may double your risk for depression if levels are elevated. This toxic by-product accumulates when you’re deficient in B6, B12, and folic acid, impairing brain chemistry.
Studies by Professor David Smith from Oxford show that lowering homocysteine can dramatically slow brain shrinkage and improve mood. Which is why we now offer at home homocysteine test kits so you can monitor your own level and prevent disease (7,8,9).
- What to do: Eat leafy greens, whole grains, and fortified foods. Test your homocysteine and aim for levels below 7 μmol/L. Supplement with a methylated B complex (20 mg B6, 500 μg B12, and 400 μg methylfolate).
—
“B vitamins are brain-makers; without them, key neurotransmitters like serotonin can’t be synthesised” – Patrick Holford, Upgrade Your Brain.
—
3. Fuel Your Brain with Serotonin Precursors
Serotonin, your “happy hormone”, is made from tryptophan, an amino acid found in protein-rich foods like fish, poultry, beans, and eggs. For some, tryptophan conversion to serotonin is impaired due to poor digestion or low stomach acid, common with age and stress.
Supplementing with 5-HTP can bypass these barriers. Clinical studies show 5-HTP compares favourably with SSRIs in treating depression (10, 11, 12, 13).
- What to do: Include tryptophan-rich foods daily and consider a 5-HTP supplement (100–200 mg twice daily). Always consult your doctor if combining with antidepressants.



—
4. Balance Your Blood Sugar
Maintaining stable blood sugar levels is essential for mood regulation, as uneven glucose supply to the brain can lead to irritability, fatigue, and depressive symptoms. Diets high in refined carbohydrates and sugar contribute to these fluctuations and are linked to poor mood and an increased risk of depression. A study of 3,456 adults found that individuals consuming diets rich in processed foods had a 58% greater risk of depression, whereas those eating whole foods experienced a 26% reduced risk (14, 14, 16).
Refined sugars also deplete mood-enhancing nutrients like B vitamins, essential for energy production, and divert chromium, which is vital for glucose regulation. Adopting a low glycaemic load (GL) diet, avoiding caffeine and alcohol, and focusing on whole foods, fruits, and vegetables can help stabilise blood sugar levels and improve mood.
- What to do: Follow a Low-GL diet with whole foods, low-GL carbs, and protein at every meal. Avoid sugar, caffeine, and alcohol .
5. Boost Your Vitamin D Levels
The “sunshine vitamin,” vitamin D, is essential for mood regulation. Research shows a 40% lower incidence of depression in those with adequate vitamin D. Alarmingly, over 60% of the UK population is deficient during winter (17, 18, 19, 20).
- What to do: Get tested and aim for levels above 75 nmol/L. Supplement with 2,000–3,000 IU daily in winter months.
—
6. Include Chromium to Combat Atypical Depression
If you suffer from atypical depression—characterised by weight gain, fatigue, and carbohydrate cravings—you might benefit from chromium. Studies show chromium supplementation can improve mood scores by up to 83% (21, 22, 23).
- What to do: Include whole grains and vegetables or supplement with 600 mcg of chromium picolinate daily.
—
7. Bring on the Sunshine and Movement
Exercise and sunlight have a direct effect on serotonin levels and mood. Regular exercise boosts brain-derived neurotrophic factor (BDNF), which helps build new brain cells and connections】.
- What to do: Aim for 30 minutes of exercise daily and sun exposure for 15 minutes, when safe.
—
Key Action Plan
- Eat oily fish twice weekly or supplement omega-3s with at least 1,000 mg EPA and DHA.
- Test and lower homocysteine with B6, B12, and folic acid supplements.
- Try 5-HTP to boost serotonin naturally.
- Follow a Low-GL diet to stabilise blood sugar.
- Supplement vitamin D during winter. Find out more about dose here.
- Add chromium for atypical depression.
- Exercise regularly and get sensible sun exposure.
—
—
Food for the Brain is a not-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
- World Health Organization. Depression and Other Common Mental Disorders: Global Health Estimates. WHO; 2017.
- Brown G, et al. Social support, self-esteem and depression. Psychol Med. 1986;16(4):813-31.
- Hibbeln JR. ‘Fish consumption and major depression’. Lancet, vol 351(9110), pp. 1213 (1998)
- M. Peet and R, Stokes, Omega 3 Fatty Acids in the Treatment of Psychiatric Disorders Drugs, vol 65(8), pp. 1051-9 (2005)
- S Kraguljac NV, Montori VM, Pavuluri M, Chai HS, Wilson BS, Unal SS (2009) Efficacy of omega-3 Fatty acids in mood disorders – a systematic review and metaanalysis. Psychopharmacology Bulletin 42(3):39-54
- Hibbeln JR. Fish consumption and major depression. Lancet. 1998;351(9110):1213.
- Coppen A, Bailey J. Folic acid and affective disorders. J Affect Disord. 2000;60(2):121-30.
- Taylor MJ, Carney SM, Goodwin GM, Geddes JR. Folate for depressive disorders. Cochrane Database Syst Rev. 2003;(2):CD003390.
- Smith AD, Refsum H. Homocysteine, B vitamins, and cognitive impairment. Annu Rev Nutr. 2016;36:211-39.
- Poldinger W et al. A comparison of 5-hydroxytryptophan and fluvoxamine. Psychopathology. 1991;24(2):53-81.
- E. Turner, Serotoninalacarte: Supplementation with the serotonin precursor 5-hydroxytryptophan.’ Pharmacology&Therapeutics (2005) [article in press].
- W. Poldinger et al. A functional-dimensional approach to depression: serotonin deficiency and target syndrome in a comparison of 5-hydroxytryptophan and fluvoxamine, Psychopathology vol 24(2), pp. 53-81 (1991)
- Associate editor: K.A. Neve ‘Serotonin a la carte: Supplementation with the serotonin precursor 5-hydroxytryptophan’ ErickH. Turner a,c,d,*, Jennifer M. Loftis a,b,c, AaronD. Blackwell a,b,e Pharmacology & Therapeutics(2005) www.elsevier.com/locate/pharmthera
- Akbaraly TN, Brunner EJ, Ferrie JE, et al. Dietary pattern and depressive symptoms in middle age. Br J Psychiatry. 2009;195:408–13.
- Benton D, Owens DS, Parker PY. Blood glucose influences memory and mood in an everyday setting. Biol Psychol. 1982;14(1-2):129–35.
- Christensen L. Psychological distress and diet – effects of sucrose and caffeine. J Appl Nutr. 1988;40(1):44–50.
- Lansdowne AT, Provost SC (1998): Demonstrates that vitamin D3 supplementation enhances mood in healthy subjects during winter.
- C. Wilkins et al. (2006): Links vitamin D deficiency to low mood and poorer cognitive performance in older adults.
- A. Nanri et al. (2009): Discusses the association between vitamin D levels and depressive symptoms across seasonal changes.
- R. Jorde et al. (2008): Shows that vitamin D supplementation alleviates depressive symptoms in overweight and obese individuals
- Lifting Depression – The Chromium Connection by Dr Malcolm McLeod (Basic Health Publications):
- J. R. Davidson et al, Effectiveness of chromium in atypical depression: a placebo-controlled trial, Biol Psychiatry, vol 53(3), pp. 261-4 (2003)
- Docherty, J et al, ‘A Double-Blind, Placebo-Controlled, Exploratory Trial of Chromium Picolinate in Atypical Depression’. Journal of Psychiatric Practice. Vol 11(5), pp. 302-314, (2005)
- Holford P. Upgrade Your Brain. HarperCollins; 2024.
Are You Being Fructed? Fructose, Dementia, Diabetes & Brain Fog
By Jerome Burke

Why too much fructose is driving dementia, diabetes and brain fog
—
The fruit sugar ‘fructose’ isn’t generally considered a food that’s best avoided. After all, it comes from fruit.
Yet a radical new theory, developed by Richard Johnson, Professor of Nephrology at the University of Colorado, explains how it can trigger various damaging changes in our metabolism that make us more likely to develop chronic conditions such as diabetes, obesity and Alzheimer’s. If doctors better understood this, it could transform the new emphasis on sickness prevention that the government is promising.
—
The science of being ‘fructed’
Professor Johnson has produced what is effectively a biochemical wiring diagram of the connections which fructose turns on and off, that are making an increasing number of people sick. Fructose makes up half of white sugar and most of fructose corn syrup which is the main sweetener in fizzy drinks and ultra-processed foods as well as being the main sugar in fruit, particularly fruit juice.
For instance, the amount of fat stored in the liver increases, driving fatty liver disease, while the cell’s mitochondria, which create the body and brain’s energy molecule ATP, become less productive and blood pressure goes up. The result is that you get fatter, with more brain fog and fatigue and feel less inclined to exercise. Fructose is also a major promoter of diabetes.
Meanwhile an anti-ageing process called autophagy, which would normally clear away used up and damaged mitochondria, the cell’s energy factories, to make room for new ones, is disabled. When fructose crosses the blood-brain barrier into the brain, it is one of the factors causing the brain to form the clumps of amyloid protein found in Alzheimer’s, which is the focus of new drug treatments.
Why on earth does fructose carry out such a blitz on our bodies? Why would the body run a programme that was potentially so lethal?
“It would be wrong to think of fructose as some sort of major toxin, although it becomes neurotoxic in excess,” says Professor Johnson. “Instead, its remarkable range of effects are part of an ancient set of biological programs, which we call the ‘Survival Switch’, that work to prepare animals for hibernation, storing supplies in preparation for times of famine.” This is why fat storage increases and energy drops off producing brain fog. The trouble is we never run out of food or fructose in our modern times.
—
Eat your fruit, don’t drink it.
None of this means that we should avoid fruits, which contain only a small amount of fructose that comes with beneficial fibre that feeds our vital gut bacteria, plus various nutrients. Not so for fruit juice, devoid of fibre. A glass of orange juice is the equivalent of three oranges in terms of fructose, but without the fibre. So, eat your fruit, don’t drink it.
But this does explain why too much blood glucose from regularly eating generous amounts of sugar-laden foods and carbohydrates, is so damaging? The liver turns the excess glucose into fructose with all its knock-on effects. Other substances that can accelerate fructose production are alcohol and salt.
This rise in fructose intake and its presence in processed food makes it all too easy to start piling on the pounds, regardless of how many calories you have cut or how much further you are running. It’s a connection that very few nutritionists or GPs are aware of.
A sign of the widespread damage the Survival Switch can cause is that there are low ATP levels in the brains of people with disorders such as obesity, diabetes, fatty liver disease and Alzheimer’s. Understanding this points to new ways to cut the risks of these chronic disorders. Adenosine triphosphate (ATP) is a molecule that stores and provides energy for cells. It’s a key biomolecule that’s involved in almost all cellular processes.
A simple, but very effective solution, is to run a blood test – HbA1c – the gold standard test GPs use to screen for diabetes. HbA1c is a test that measures your average blood sugar level (glucose) over the past two to three months. A recent study of 374,021 older men with diabetes found that keeping the level of HbA1c stable at an optimal level over a period of three years cut risk of dementia by a third. Similar benefits have been found with patients with pre-diabetes (Prediabetes means that your blood sugars are higher than usual, but not high enough for you to be diagnosed with type 2 diabetes. It also means that you are at high risk of developing type 2 diabetes.) But far lower levels of HbA1c than those used to diagnose diabetes are associated with the first signs of brain shrinkage, which is the hallmark of cognitive decline, even in teenagers.
That is why we offer, as part of our ‘citizen science’ research, an at home pin-prick test of HbA1c, to find out not only who is at risk, but also how to reverse that risk. It also works alongside the free Cognitive Function Test that calculates your future Dementia Risk Index and suggests various lifestyle and nutrition changes to help reduce it, including a low fructose diet (Find out more about low fructose foods here).
We also recommend increasing omega-3 intake from oily fish, increasing B vitamins, especially B12, as well as an active lifestyle, as part of COGNITION, our personalised 6-month programme. In this programme we also dive deeper into lowering your ‘glycaemic load’ (GL), which is low in fructose, alongside periods of time of eating in a ‘ketogenic’ way by keeping sugar and carbohydrates to a minimum. The body responds by creating ketones, energy packets that can replace glucose as an energy source for the brain, helping to undo the damage.
(You get access to COGNITION when you become a FRIEND of Food for the Brain here)
‘Burning ketones can also increase the number and output of the cell’s energy factories, known as mitochondria, which are damaged by fructose,’ says Professor Robert Lustig of the University of California, author of the best-selling book Metabolical and who sits on our Scientific Advisory Board. You can read more in his detailed article here.
Both Professor Johnson and Professor Lustig are also part of the Alzheimer’s Prevention Expert Group who have written to UK dementia prevention authorities to add sugar, and specifically a high fructose diet, to the list of known risk factors.
—
The connection to Ozempic…
This low fructose approach also naturally promotes the enzyme GLP-1, targeted by the weight loss drugs Ozempic and Wegovy, but without the side-effects or rebound weight gain.
Our founder Patrick Holford says: “Today’s typical diet of burgers, carbonated drinks, fruit juice, ice cream, bread, biscuits, cakes and confectionery, plus alcohol and salt, is a dementia time-bomb. Our brains are literally being ‘fructed’. We see the same shrinkage in the same regions of the brain in teenagers with a high sugar intake that are seen in older Alzheimer’s patients. We think of the resulting dementia as type-3 diabetes.”
—
Actions
- To find out more about low fructose foods visit www.foodforthebrain.org/fructose
- Click here to join our research and test your HbA1c with us
- Support our charitable work and research by becoming a FRIEND
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References:
- Johnson RJ et al. The fructose survival hypothesis for obesity. Philos Trans R Soc Lond B Biol Sci. 2023 Sep 11;378(1885):20220230. doi: 10.1098/rstb.2022.0230
- Underwood PC et al HbA1cTime in Range and Dementia JAMA Netw Open. 2024 Aug 1;7(8):e2425354. doi: 10.1001/jamanetworkopen.2024.25354
- Yau PL et al Obesity and metabolic syndrome and structural brain impairments in adolescence. Pediatrics. 2012 Oct;130(4):e856-64. doi: 10.1542/peds.2012-0324
Your Glutathione Index Defines How Your Cells Are Ageing
Your Glutathione Index Defines How Your Cells Are Ageing

Nutritional therapists have been measuring red cell glutathione and supplementing glutathione or its precursor N-Acetyl-Cysteine (NAC) for decades. But it’s really hard, and expensive, to measure accurately. Until now.
So how does the Glutathione Index work?
All of life is a balance between antioxidants and oxidants. That is why we, an oxygen based lifeform, have a finite life. Inside your cells glutathione (GSH) is working every second to stop harmful oxidants from ageing you. The result is spent or oxidised glutathione (GSSG). Our new test – a world first – measures the ratio between fully loaded glutathione (GSH) and oxidised glutathione (GSSG). The Glutathione index (GSH/GSSG) shows you how much antioxidant potential you have and how many metabolic fires you’ve extinguished. This ratio is the difference between mental health and mental illness.
Why does knowing this single marker help with Alzheimer’s, diabetes, schizophrenia, severe autism, depression & more?
Why Does Knowing This Single Marker Help With Alzheimer’s, Diabetes, Schizophrenia, Severe Autism, Depression and More?
The Science
NAC has plenty of evidence to support its use as a promoter of glutathione and mental health, thus reducing the brain’s oxidative stress. The latest 2022 review states:
“N-acetyl-L-cysteine (NAC) is a compound of increasing interest in the treatment of psychiatric disorders. Primarily through its antioxidant, anti-inflammatory, and glutamate modulation activity, NAC has been investigated in the treatment of neurodevelopmental disorders, schizophrenia spectrum disorders, bipolar-related disorders, depressive disorders, anxiety disorders, obsessive compulsive-related disorders, substance-use disorders, neurocognitive disorders, and chronic pain. Currently NAC has the most evidence of having a beneficial effect as an adjuvant agent in the negative symptoms of schizophrenia, severe autism, depression, and obsessive compulsive and related disorders.” (1)
Glutathione and Schizophrenia
Quoting Lorraine Wilder (whose MSc in schizophrenia we funded) “Glutathione (GSH) is an important antioxidant and free radical scavenger that has been found to be decreased in the brains of people with schizophrenia [2, 3]. Although oral GSH supplementation has poor bioavailability [4], N-Acetyl Cysteine (NAC) has been shown to successfully raise plasma glutathione levels in those with schizophrenia [5]”.
Clinical Evidence and Case Studies
In a case study of a 24 year old woman with chronic and worsening paranoid-type schizophrenia that was generally unresponsive to anti-psychotic treatment, the addition of NAC supplementation improved the patient’s symptomatology in seven days. In addition to the schizophrenia-specific symptoms, improvements were observed in spontaneity, social skills and family relations by both the patient and family members. A randomised placebo-controlled trial (RCT) including 42 participants with schizophrenia, who were experiencing an acute phase of symptomatology, were randomly assigned to receive up to 2 g/d of NAC plus up to 6 mg/d of risperidone for 8 weeks as an adjunct intervention. Significant negative symptoms were found in the active treatment group compared to controls but not in positive or general psychopathology [6].
Larger Trials and Longer-Term Findings
Furthermore, a larger RCT of 140 participants observed significant improvements on global symptomatology and general and negative symptoms of schizophrenia in the NAC supplementation (2 g/d; in addition to anti-psychotic medication) group in comparison to the placebo group over a 24-week period, but not positive symptoms [7]. Notably, after a 4-week washout period these beneficial effects diminished, with the exception of clinical severity scores.
Expert Perspective on Brain Oxidative Stress
According to Dr Chris Palmer, assistant professor at HarvaWhy the Glutathione Index Is the Best Indicator of Brain Oxidative Stress
rd Medical School:“Glutathione (GSH), the brain’s primary antioxidant, plays a crucial role in maintaining redox balance. Magnetic resonance studies have provided mixed results regarding GSH levels in schizophrenia patients, with some studies indicating decreased levels in chronic schizophrenia, while others found no significant differences. However, these inconsistencies may be due to variations in disease chronicity, age, and symptom severity among study participants. The findings from these studies suggest several potential therapeutic targets for schizophrenia. Addressing mitochondrial dysfunction, redox imbalance, and impaired energy metabolism could lead to more effective treatments. For instance, N-acetylcysteine (NAC), a precursor to GSH, has shown promise in increasing brain GSH levels and improving symptoms in first episode psychosis patients.”
Why the Glutathione Index Is the Best Indicator of Brain Oxidative Stress
The GSH/GSSG ratio reflects the activity of the enzyme glutathione reductase which is responsible for the transformation of GSSG (used, oxidised) to GSH (the reduced or fully loaded form that acts as a radical scavenger).
—
Glutathione Reductase and Dementia
Reductions in glutathione reductase (GR) enzyme levels in patients with dementia are well established. GR levels alone are therefore a fairly good biomarker of dementia. But the mere presence of the enzyme does not guarantee its high activity. GR needs to consume NADP molecules to function properly. The advantage of our test is, therefore, that it shows changes in GR activity not only due to higher/lower GR gene activity but also due to the absence of the reaction cofactor NADP.
Impaired Glutathione Recycling in Dementia
As shown by Irene Martinez de Toda et al 2019 (8) data, patients with dementia have a reduction in both the enzymes (GR and GP) that recycle glutathione. Thus, in general, it can be said that the glutathione metabolism (recycling) loop in those with dementia ‘spins’ much slower than in healthy patients. As a result, dementia patients have a lower potential to dynamically fight free radicals and will have a worse Glutathione Index.
What Happens When Recycling Slows Down
In patients, the enzyme GR, which is responsible for recycling spent/oxidised glutathione back to fully loaded, slows down, which leads to the accumulation of oxidised glutathione (GSSG) and the depletion and inability to produce GSH.
Thus, the concentration of GSH decreases while that of GSSG increases. Hence the Glutathione Index gets worse / is lower.
Developing the Glutathione Index Test

This is why we have created the Glutathione Index test alongside analytic chemist, Dr Konrad Kowalski. “This ratio, the Glutathione Index, is a biomarker for many diseases, including both type 1 and 2 diabetes, liver cirrhosis, multiple sclerosis and Alzheimer’s disease.” says Dr Kowalski, “As a result of having good data, our scientists are currently reviewing the reference ranges to be even more accurate. Having a way to measure brain ageing with a home test kit from a pin prick of blood, means we can realistically see what the impact of specific diet changes and antioxidant supplements might be.”
We now know that a desirable level is above 800. Below 500 is an indicator that you need to increase your intake of antioxidants from food and/or supplements, and/or reduce your intake of oxidants from smoking, pollution or fried food.
So will you join us and become a part of our Anti-Age Your Brain Campaign? We need Citizen Scientists to order and complete the test so you can start to protect your brain from ageing and so we can research what the ‘perfect number’ is.

Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
1. Bradlow RCJ, Berk M, Kalivas PW, Back SE, Kanaan RA. The Potential of N-Acetyl-L-Cysteine (NAC) in the Treatment of Psychiatric Disorders. CNS Drugs. 2022 May;36(5):451-482. doi: 10.1007/s40263-022-00907-3. Epub 2022 Mar 22. Erratum in: CNS Drugs. 2022 Apr 28;: PMID: 35316513; PMCID: PMC9095537.
2 Yao JK, Leonard S, Reddy R: Altered glutathione redox state in schizophrenia. Dis Markers 2006, 22(1):83–93.
3 Gawryluk JW, Wang J-F, Andreazza AC, Shao L, Young LT: Decreased levels of glutathione, the major brain antioxidant, in post-mortem prefrontal cortex from patients with psychiatric disorders. Int J Neuropsychopharmacol 2011, 14(01):123–130.
4 Witschi A, Reddy S, Stofer B, Lauterburg B: The systemic availability of oral glutathione. Eur J Clin Pharmacol 1992, 43(6):667–669.
5. Lavoie S, Murray MM, Deppen P, Knyazeva MG, Berk M, Boulat O, Bovet P, Bush AI, Conus P, Copolov D, Fornari E, Meuli R, Solida A, Vianin P, Cuénod M, Buclin T, Do KQ:Glutathione precursor, N-acetyl-cysteine, improves mismatch negativity in schizophrenia patients. Neuropsychopharmacology 2008, 33(9):2187–2199.
6. Farokhnia M, Azarkolah A, Adinehfar F, Khodaie-Ardakani M-R, Hosseini S-M-R, Yekehtaz H, Tabrizi M, Rezaei F, Salehi B, Sadeghi S-M-H, Moghadam M, Gharibi F, Mirshafiee O:, Akhondzadeh S: N-acetylcysteine as an adjunct to risperidone for treatment of negative symptoms in patients with chronic schizophrenia: a randomized, double-blind, placebo-controlled study. Clin Neuropharmacol 2013, 36(6):185–192.
7. Berk M, Copolov D, Dean O, Lu K, Jeavons S, Schapkaitz I, Anderson-Hunt M, Judd F, Katz F, Katz P, Ording-Jespersen S, Little J, Conus P, Cuenod M, Do KQ, Busha AI: N-acetyl cysteine as a glutathione precursor for schizophrenia—a double-blind, randomized, placebo-controlled trial. Biol Psychiatry 2008, 64(5):361–368.
8. Martínez de Toda I, Vida C, Sanz San Miguel L, De la Fuente M. Function, Oxidative, and Inflammatory Stress Parameters in Immune Cells as Predictive Markers of Lifespan throughout Aging. Oxid Med Cell Longev. 2019 Jun 2;2019:4574276. doi: 10.1155/2019/4574276. PMID: 31281577; PMCID: PMC6589234.
What Has Standing On Your Head, Paragliding, Foraging & Lifting Weights Got In Common?
In a world often filled with daunting health challenges, Alzheimer’s Prevention Day stood out as a beacon of hope and action.
This year was the first launch of this global initiative and we were privileged to witness an incredible turnout: over 10,000 individuals visited our site, driven by a shared determination to tackle Alzheimer’s disease head-on. The day was not just about awareness but about tangible actions that each person can take to safeguard their cognitive health.
One of the highlights was our interactive 3-minute Alzheimer’s Prevention Check, which 8,000 participants eagerly completed. This simple yet impactful test empowers individuals to assess their cognitive health and take proactive steps towards prevention.
Moreover, the 30-second challenge captured hearts and imaginations alike. We asked people to share on video what they do to help prevent Alzheimer’s each day?
And the answers are astounding!
From paragliding adventures to quirky activities like standing on one’s head or foraging in local forests, participants demonstrated that preventing Alzheimer’s can be both effective and fun.
Ali’s daring paragliding escapade, Zoe’s upside-down yoga prowess, and Nodge’s foraging adventures exemplify the creativity and commitment shown by our community. These actions not only inspire but also remind us that preventing Alzheimer’s is within everyone’s reach, with room for creativity and enjoyment along the way.
Central to the success of Alzheimer’s Prevention Day were the dedicated individuals behind the scenes. We extend heartfelt thanks to Cath and the team for their meticulous editing of inspiring films, and to Alex for crafting a user-friendly website that hosted invaluable resources and engaging content.
—
A BIG thank you!
Behind every groundbreaking initiative are the scientists and professors whose expertise and dedication drive progress. Their research forms the backbone of our mission, guiding us towards effective prevention strategies and empowering individuals to make informed choices about their cognitive health.
As we reflect on the triumphs of Alzheimer’s Prevention Day, we invite you to join us in building a repository of inspiring actions. Visit our website to explore videos showcasing innovative ways people are preventing Alzheimer’s, and most importantly, create your own 30-second film. Share your daily practices that promote brain health, from physical activities to dietary choices, and inspire others to do the same.
Together, let’s continue to raise awareness, take meaningful action, and pave the way towards a future where Alzheimer’s is preventable. Visit Alzheimer’s Prevention Day website to learn more and get involved today.
Your actions today can make a difference tomorrow.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
Make Eating Less Sugar Easier (& a FREE Recipe!)
Too much sugar shrinks the brain, but it’s so attractive. Why?
We are led by the science here at Food for the Brain, so we know that one of the best things you can do for your brain is to reduce your sugar and support your insulin control. That is why it is one of our key lifestyle domains in the COGNITION programme.
However, you probably already know too much sugar isn’t great for health but how can we make eating a lower carb and sugar life easier?
—
First, let’s recap the science…
Dr. Robert Lustig, a renowned expert on brain health and a member of our scientific advisory board, highlights the significant role of insulin control and dietary choices in preventing cognitive decline.
Research from Columbia University in 2004 revealed that individuals with high insulin levels, (a primary indicator of metabolic dysfunction), were twice as likely to develop dementia compared to those with healthy insulin levels (1). Furthermore, those with the highest insulin levels exhibited the worst memory retrieval abilities (1). Similarly, an Italian study linked elevated insulin levels to declining mental function (2).
Several studies have established a connection between high sugar consumption and poor cognitive outcomes. For instance, a study among Puerto Ricans found that high sugar intake doubled the risk of cognitive impairment (3), while another U.S. study correlated elevated blood sugar levels with memory loss (4). The detrimental impact of high dietary glycaemic load (GL) on cognitive function has been observed in studies from Ireland and the United States, indicating that high GL diets are strongly associated with Alzheimer’s-related pathological changes (5,6).
—
What is Glycaemic load?
Glycaemic load considers both the quality (GI – glycaemic index) and the quantity (carbohydrate content) of the carbohydrates in a food serving. It provides a more accurate picture of how a food will affect blood sugar levels. The formula for calculating glycaemic load is:
- GL = GI x carbohydrate / 100
A high GL diet measured by the total glucose load on the bloodstream, is linked to increased amyloid plaque formation and cognitive decline, particularly in individuals with the ApoE4 gene, which regulates fat metabolism (7). Even individuals with high-normal blood glucose levels experience greater brain shrinkage and cognitive impairment compared to those with lower levels, as shown in long-term studies (8).
Plus, the damage of a high-GL diet can start early in life. Dr. Lustig points out that overweight children on high-GL diets show signs of cognitive decline, and adolescents with metabolic dysfunction from such diets exhibit hippocampal shrinkage and other brain structure changes (9,10).
So it is clear that eating excess sugar or the wrong types of carbohydrates with a high GL is a problem, so what do you eat?
(Wondering if you’re eating too much sugar? Then test, don’t guess with our home HbA1c test – find out more here.)
—
What to eat?
There are two options: following a low GL diet or going a step further and adhering to a ketogenic approach (or switching between the two as Patrick highlights in the Hybrid Diet book). For more info on the ketogenic diet click here to find out more
A low GL diet is focused on consuming foods that have a minimal impact on blood sugar. Basically a diet rich in:
- Vegetables: Most non-starchy vegetables like spinach, broccoli, and bell peppers.
- Fruits: Berries, cherries, grapefruit, and apples.
- Legumes: Lentils, chickpeas, and black beans.
- Whole Grains: Barley, quinoa, and whole oats.
- Fish and meat or tofu/tempeh: unprocessed
- Dairy: Plain yoghurt and milk (unsweetened).
- Nuts and Seeds: Almonds, walnuts, chia seeds, and flaxseeds.
Whilst eating this way can support your brain health it can also help you sustain energy levels, help with weight loss and improve heart health.
—
So how can we make it easier?
At Food for the Brain we have a few ways to help you feed your brain on the right foods:
- Complete the Cognitive Function Test and join COGNITION so we can walk you through how to reduce sugar and upgrade your brain over the next few months.
- Upgrade Your Brain Cook App – full of low GL recipes and coming soon. Help us by pre ordering today to get brain-loving recipes at your fingertips.
- Here is a recipe sample:
—

Almond and coconut porridge
Breakfast Serves 2, generously
TOTAL GLs: 4
Ingredients:
2 tbsp milled flaxseed
2 tbsp coconut flour
2 tbsp whole flaxseed
2 tbsp chia seeds
2 tbsp coconut flakes, toasted in a dry pan
2 tbsp raspberries
2 tbsp blueberries
2 strawberries
8 walnuts, broken up
1 tbsp soft brown sugar alternative (or sweetener of choice)
300ml unsweetened almond milk
1 tbsp chicory root syrup (or sweetener of choice)
Instructions:
- Stir everything (except the desiccated coconut, nuts and berries) together in a saucepan and let sit for 10 mins.
- Gently heat through until thickened – add a little more milk if needed to get the consistency you like.
- Top with the berries, nuts and toasted coconut – add some natural yoghurt if you like.
- Drizzle with the chicory syrup
Cooks Notes
It’s worth seeking out the chicory syrup – very low sugar and also high fibre.
Nutrition Highlights
- Antioxidants: High in antioxidants, particularly vitamins A, C, and E, which help protect cells from damage and support immune function.
- Protein: A moderate source of protein, supporting muscle maintenance and repair.
- Fibre: Contains a high amount of fibre, aiding in digestion and promoting satiety.
—
Other resources
Here are a few other resources to make low sugar easier,
- FATT bars – easy low GL and low carb snacks for on-the-go. Use the code FFTB10 to save 10% and FATT will donate to the charity with every purchase.
- Dillon bread – low carb bread and their brand new high fibre, low GL, Chicory Fibre Syrup perfect for adding to porridge and also suitable for diabetics. Use code FFB10 to save 10% and Dillon will donate 10% with every purchase.
- Keto Mojo – if you want to take it a step further and follow a ketogenic diet then grab one of their ketone readers to make life easier and to check you are in ketosis. Use code FFB10 to save 10%.
These companies are some of our supporting organisations – find out more here.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
- Abbatecola AM, Paolisso G, Lamponi M, Bandinelli S, Lauretani F, Launer L, Ferrucci L. Insulin resistance and executive dysfunction in older persons. J Am Geriatr Soc. 2004 Oct;52(10):1713-8. doi: 10.1111/j.1532-5415.2004.52466.x. PMID: 15450050.
- Abbatecola AM, Paolisso G, Lamponi M, Bandinelli S, Lauretani F, Launer L, Ferrucci L. Insulin resistance and executive dysfunction in older persons. J Am Geriatr Soc. 2004 Oct;52(10):1713-8. doi: 10.1111/j.1532-5415.2004.52466.x. PMID: 15450050.
- Ye X, Gao X, Scott T, Tucker KL. Habitual sugar intake and cognitive function among middle-aged and older Puerto Ricans without diabetes. Br J Nutr. 2011 Nov;106(9):1423-32; doi: 10.1017/S0007114511001760. Epub 2011 Jun 1. PMID: 21736803; PMCID: PMC4876724.
- Power SE, O’Connor EM, Ross RP, Stanton C, O’Toole PW, Fitzgerald GF, Jeffery IB. Dietary glycaemic load associated with cognitive performance in elderly subjects. Eur J Nutr. 2015 Jun;54(4):557-68. doi: 10.1007/s00394-014-0737-5. Epub 2014 Jul 18. PMID: 25034880.
- Seetharaman S, Andel R, McEvoy C, Dahl Aslan AK, Finkel D, Pedersen NL. Blood glucose, diet-based glycemic load and cognitive aging among dementia-free older adults. J Gerontol A Biol Sci Med Sci. 2015 Apr;70(4):471-9. doi: 10.1093/gerona/glu135. Epub 2014 Aug 22. PMID: 25149688; PMCID: PMC4447796.
- Taylor MK, Sullivan DK, Swerdlow RH, Vidoni ED, Morris JK, Mahnken JD, Burns JM. A high-glycemic diet is associated with cerebral amyloid burden in cognitively normal older adults. Am J Clin Nutr. 2017 Dec;106(6):1463-1470. doi: 10.3945/ajcn.117.162263. Epub 2017 Oct 25. PMID: 29070566; PMCID: PMC5698843.
- Taylor MK, Sullivan DK, Swerdlow RH, Vidoni ED, Morris JK, Mahnken JD, Burns JM. A high-glycemic diet is associated with cerebral amyloid burden in cognitively normal older adults. Am J Clin Nutr. 2017 Dec;106(6):1463-1470. doi: 10.3945/ajcn.117.162263. Epub 2017 Oct 25. PMID: 29070566; PMCID: PMC5698843.
- M.E. Mortby et al., ‘High “normal” blood glucose is associated with decreased brain volume and cognitive performance in the 60s: the PATH through Life Study’, PLoS One (2013), vol 8
. - Yau PL, Castro MG, Tagani A, Tsui WH, Convit A. Obesity and metabolic syndrome and functional and structural brain impairments in adolescence. Pediatrics. 2012 Oct;130(4)
. doi: 10.1542/peds.2012-0324. Epub 2012 Sep 3. PMID: 22945407; PMCID: PMC3457620. - Lakhan, S.E., Kirchgessner, A. The emerging role of dietary fructose in obesity and cognitive decline. Nutr J 12, 114 (2013).
- Loef M, Walach H. Fruit, vegetables and prevention of cognitive decline or dementia: a systematic review of cohort studies. J Nutr Health Aging. 2012 Jul;16(7):626-30. doi: 10.1007/s12603-012-0097-x. PMID: 22836704.
Snacks for the brain – easy ways to feed your brain on the go!
The food you eat feeds your brain but how can you consistently eat healthy even on the go, or when life is busy?
We know here at Food for the Brain that a low Glycemic Load diet is one of the 8 ways you can reduce your risk of dementia and Alzheimer’s (and improve your Cognitive Function score – take the free validated online test here) – which is why we are creating our Recipe App so that you have access to lots of brain loving recipes.
But what can you eat when travelling, on the go or for an easy snack?
That is why we want to introduce you to FATT bars. As one of our supporting organisations, FATT provides a variety of good quality, sugar free, convenient and tasty snacks.
So if you are preparing for summer holidays, work trips or have a busy schedule then these might be the perfect way to nourish your brain!

Introducing FATT – Real Keto Snacks!
Feeding the brain is a no-brainer but picking the right foods can be hard.
At FATT we really love the brain and because we love the brain, we also love the gut.
Everything we pick must be right for both brain and gut which is why we really do love nuts and in particular almonds and macadamias. Nuts are smart as they are rich in protein, B vitamins and vitamin E but are also a good source of potassium, selenium, magnesium, zinc and copper.
Macadamias are also rich in omega 3 to help balance any omega 6 in your diet.
We then add in the inulin and chicory fibre for a prebiotic kick to feed your healthy gut bio.

Whether you are eating a cookie or a brownie, a bar or a bite, you can be sure that you are getting food for the brain and gut without compromise. At FATT we do not use any sweeteners (artificial or otherwise) that might interfere with your gut and your brain or even fool your body into thinking it is digesting sugar.
We allow the natural sweetness of nuts or butter or chicory to give you a gentle sweet taste knowing that your body will not have any blood sugar spike or any insulin release.
Try our unique range of healthy low carb but indulgent snacks at a special discount and we will also make a further charitable contribution to Food for the Brain and its amazing work.
You can pick from Almond + Vanilla Keto Cookie, Double Chocolate Keto Brownie, Caramel + Sea Salt Keto Bar, Chocolate + Mint Bites and MORE!
Go and order your first box or single bars at www.livefatt.com and use the unique code FFTB10 to get a special Food for the Brain charity discount.
—
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
Is the Easter Bunny’s Brain Shrinking Due to Pre-diabetes?
by Patrick Holford
Easter is meant to follow on from Lent – 40 days of fasting. There lies the problem.
—
‘We’ are the product of natural selection – survival of the fattest.
Those of us who can readily store carbs as fat through periods of famine have survived and become dominant. Now, there are no periods of famine, no ‘lent’ up, it’s just carbs all the way.
With one in six over 40 diabetic, the question is, are you heading in that direction?
Even raised glucose, but within the ‘normal’ range, in mid life increases Alzheimer’s risk by 14.5%.
—
Why not find out?
We have a simple pinprick blood test to help you do just that. It measures the percentage of your red blood cells that are sugar-damaged or ‘glycosylated’. It’s called glycosylated haemoglobin, or HbA1c. This simple pinprick blood test is, in effect, measuring the total blood sugar spikes you experienced over the past three months (red blood cells, called haemoglobin, live for three months).
—
What should you be aiming for?
Ideally, it should be 5% (31mmol/mol) or less. That’s healthy.
Above 5.4% (36) and in studies you can already pick up brain shrinkage and cognitive decline.
Above 6% (42) is considered pre-diabetic.
6.5% (48) or higher is considered diabetic.
For both brain and body health you certainly want it to be below 5.4%
(It’s measured slightly differently in the UK, in mmol/mol, which is the number shown in brackets.)
A recent study in Denmark of 20,000 people in their 60’s, published in the British Medical Journal [1], found that one in nine with an HbA1c of 6-6.1% developed diabetes in the next three years and one in five in the next five years. One in ten died.
—
How to lower your score?
It is easy to lower, if you need to. But first, you need to know where you are starting from. Then you can retest three months later and find out if what you’ve done has worked.
There are several approaches.
- A low GL diet (read Patrick Holford’s Low GL Diet Cookbook).
- An intermittent fasting approach, doing all your eating in a six hour window with dinner at eg 7pm then lunch at 1pm.
- Going ‘keto’, which Dr Georgia Ede explained in our recent webinar which you can watch here.
- There are even supplements that can help – chromium, HCA (Hydroxycitric acid) found in a type of tamarind and glucomannan fibre.
You will learn about all these and more if you’ve signed up for the COGNITION programme by becoming a FRIEND and select the ‘Low carbs and GL’ section. Jill, a retired teacher, lost almost a stone following this advice.
—
But first, we suggest you measure your baseline HbA1c.
It’s more predictive of your blood sugar control than just your weight or waist circumference. In fact, it is the single most important measure of your glucose balance ‘resilience’ which is why it’s one of the four ‘essentials’ in our DRIfT test – the others being vitamin D, omega-3 and homocysteine (B vitamins).
We want to wish you a Healthy Easter by giving you £10 off your HBA1c test when you buy before Easter.
So that’s £39.95, not £49.95.
Also, if you book a repeat test in 3 months, which is how long it takes to ‘renew’ all your red blood cells, hopefully no longer sugar-coated, you’ll save a further 6%, bringing the cost down to £37.55, saving you £12.40 now and in 3 months time. That’s £24.80 in total. This offer ends on April 10th 2024.
Use the coupon code: easter at check out to save

(Discount applies to the HBa1c test only.)

Remember every test kit you order will not only help you upgrade your brain it will also help us in our vital research – you will become a part of our ‘Citizen Science’ team and be donating to our wider charitable work and research.
Thank you!
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References:
1 http://dx.doi. org/10.1136/bmjdrc-2022- 002946
The Four Horsemen of the Mental Health Apocalypse #2 – Brain Fuel & Antioxidants
By Patrick Holford

—
Few people realise the catastrophic decline in mental health that has occurred over the past 50 years.
‘Brain health conditions have become a global health emergency,’ according to the Federation of European Neuroscience Societies last year (1).
The big question is: why?
—
Introducing the four horsemen (recap)
I’m proposing that there are four main biological drivers of our demise which I’m calling the four horsemen of the mental health apocalypse: a lack of brain fats, messed up methylation, loss of glucose control and excessive oxidation.
The first two – brain fats and methylation – are vital for the integral structure of neuronal membranes.
The second two are vital for the function of brain cells, supplying fuel and coping with the oxidant ‘exhaust fumes’ of energy metabolism.
—

—
Brain fuel
While omega-3 and B vitamins literally build a healthy brain, it is glucose and ketones that fuel it.
As a result of this process, oxidants are created which age the brain through the process of oxidation. Of course, oxidation can also occur through external causes, which is why smoking and air pollution are also established risk factors for Alzheimer’s.
Which leads us to the next two ‘horses of the mental health apocalypse’: the brain’s fuel supply and antioxidant protection. The brain consumes more energy than any other organ of the body. Neurons can only run on glucose or ketones. The irony is that the consequence of eating too many carbs and sugar is that the brain develops insulin resistance – effectively blocking the glucose from entering the mitochondria within the neurons. Starved of their energy source, we experience the consequences as mental fatigue and forgetfulness. According to Dr Robert Lustig, Emeritus Professor of Pediatrics at the University of California, San Francisco and a member of our Scientific Advisory Board, “This cognitive decline starts young. Cognitive decline in overweight children is associated with a high GL diet (1), and adolescents with metabolic dysfunction, driven by a high GL diet, have been shown to have shrinkage of the hippocampal area of the brain, as well as other structural changes and cognitive deficits (2).” This particular study showed actual shrinkage of the Alzheimer’s associated area of the brain in teenagers with metabolic syndrome as a consequence of too much sugar and ‘white’ carbs. The youngest age of an Alzheimer’s diagnosis, which requires proof of shrinkage of the hippocampal area of the brain, is age 19, in a young man in China who had no genetic risk factors (2).
It’s a biochemical storm.
As well as the fuel starvation that insulin resistance generates, the converse of blood sugar spikes, create Advanced Glycation End-products, or AGEs, that literally damage neurons. This ‘glycosylation’ is also seen in red blood cells, and why the HbA1c test which measures glycosylated haemoglobin is so good at predicting our health. If over 6.5% (or 48 mmol/mol) of these erythrocytes are sugar damaged, it’s a clear basis for a diabetes diagnosis. Just as for the omega-3 index, HbA1c is a reliable long-term measure showing the average sugar spikes over the past three months. You can assume what’s happening in the membranes of red blood cells is also happening to the neuronal membranes in the brain.
This is why the next brain essential is to measure HbA1c.
If 6.5% is the cut-off for a diabetes diagnosis, the ideal level is actually considerably lower. In what is usually considered to be the ‘normal range’, teenagers with HbA1c above 5.4% show cognitive decline and shrinkage of the hippocampus in the central area of the brain compared to those with lower HbA1c levels (3). “In teenagers with raised, but normal levels of HbA1c, there is clear evidence of the same kind of memory problems, and the same areas of brain shrinkage seen in patients with Alzheimer’s Disease” says Dr Robert Lustig.
Shrinkage of the hippocampus is the hallmark of Alzheimer’s and is used to diagnose the disease. A new study shows that 40-year-old adults with so-called normal glucose levels, but at the higher end of the normal range, have increased their risk of Alzheimer’s by 15%. (4)
A primary function of sleep is to repair all the neuronal membrane damage that occurs during the day. No sleep, no repair and the brain ages fast. This is mainly why lack of sleep is also a strong risk factor for Alzheimer’s.
—
Do ketones fill the energy gap?
There’s a growing interest in the role of ketogenic diets and ketone promoting supplements for brain health. Professor Stephen Cunnane, our expert in the new science of ‘keto therapeutics’ has shown that giving C8 oil or supplementing ketones can help to prevent Alzheimer’s, slow down cognitive decline, improve mood and lessen anxiety. His studies showed, in those with mild cognitive impairment, that taking 30g (two tablespoons) of mainly C8 oil, resulted in a 230% increased brain energy production from ketones with no change in energy derived from glucose (5), thus filling the ‘energy gap’ so often experienced by older people or those drifting towards insulin resistance. “Our research shows that the areas of the brain that have trouble using glucose for energy are able to use ketones perfectly well, even in moderately advanced dementia. This may explain why many people later in life who are given a supplement of C8 oil or MCT oil have improvements on a battery of cognitive tests. They often feel it brings their brain power back to life” says Cunnane.
Many people also report feeling calmer, less anxious and less depressed on ketogenic diets. A new book, Change Your Diet, Change Your Mind, out next month by psychiatrist Dr Georgia Ede digs deep into the growing evidence that a ketogenic diet, or at least one low in carbohydrates, is brain-friendly and helps people out of various mental health disorders. Or you can watch the recent webinar she did with us here.
—
Antioxidant and polyphenol power
The more biologically active an essential fat is (with DHA at the top), the more prone it is to oxidation.
It is literally this ability of DHA to absorb energy (photons from light) that creates the impulse that passes information from the eye to the brain. It explains the origin of the brain and nervous system, going back a billion years to a rudimentary single cell called dynoflagellate. This little organism basically used the electric shock from photons to create the first ‘twitch’ towards light. Where there was light, there was food, and ultimately the evolution of the nervous system and brain. In simple terms, we can see that the brain is really an extension of the eye. How do we see with such precision and speed? Until now, no-one has been able to explain this satisfactorily. At the age of 93, Professor Michael Crawford, who helped our charity get started, has worked out how this occurs and how we see in colour. It requires knowledge of quantum physics, explained in a recent paper entitled ‘Docosahexaenoic Acid Explains the Unexplained in Visual Transduction’.(6)
With all this volatile fatty acid and mitochondrial energy production, cleaning up the oxidant exhaust fumes is a vital function for a healthy brain. So how do we achieve protection and how do we measure it?
There are hundreds, if not thousands of antioxidants and polyphenols in our food. Foods can be measured for their ‘Total Antioxidant Capacity’ or TAC for short. It’s worked out from an equation involving eight key antioxidants from vitamin A, carotenes (think carrots), lycopenes (rich in tomatoes), lutein and zeaxanthine (rich in green vegetables), vitamin E (in nuts and seeds), but most of all vitamin C (rich in berries, broccoli, peppers and other vegetables).
Vitamin C is a keystone nutrient as far as swinging the antioxidant equation in our favour. Individually, the impact of these nutrients on our health may be less than when combined. For example, a study of 4,740 Cache County Utah elderly residents found that those supplementing both vitamin E and C cut their risk of developing Alzheimer’s by two thirds (66%). Taking just one cut the risk by a mere quarter (25%). (7)
The higher the TAC score of our diet, the lower our risk of memory decline becomes. This was the finding of a recent study of 2,716 people over age 60. Higher TAC scores correlated with better memory function (8). Those in the highest quarter of TAC scores had half the risk of decreasing memory. Powerful stuff!
Tea, cacao, red wine, red onions, olives and berries are rich sources of polyphenols. Many of these polyphenol-rich foods improve circulation, lower blood pressure and dampen down inflammation which lies behind many brain and heart health problems.
More than a decade ago research in Norway (9) found that the more tea you drink the better; a small glass of wine (125ml) a day (preferably red, as it is rich in resveratrol) reduces the risk of cognitive decline. Cacao is also beneficial, ideally no more than 10g, (about 3 pieces) of dark, 70 percent or more. Other studies based on adding cacao to the diet have shown improved cognition, possibly by improving circulation. This was recently confirmed in a big ‘COSMOS’ trial involving over 20,000 people given a cacao extract supplement versus a placebo for five years (10). The reduction in cardiovascular risk was even greater than that of a Mediterranean diet.
The take-away message? Polyphenols are a vital part of a healthy diet for both our heart and our brain.
So, what do we need to eat and drink to protect our brain and body? Basically, eat a Mediterranean-style ‘rainbow coloured’ diet. A Mediterranean diet has more fish, less meat and dairy, more olive oil, fruit and vegetables including tomatoes, legumes (beans and lentils), and whole grain cereals than a standard Western diet. It also includes small quantities of red wine. There are variations of this kind of diet, called the MIND diet and the DASH diet, but the core components are the same. As researchers drill down, we are learning what to eat and drink and how much, to keep our minds sharp and brain young.
The trick is to really start thinking of the colours we are eating and gravitate to the strong colours, choosing organic where possible. Mustard and turmeric, for example, are strong yellows. Bright oranges include butternut squash, sweet potato, carrots. For red, think tomatoes and watermelons. Anything purple, magenta or blue is brilliant for us too. From beetroots (eat them raw, grated into salads) to blueberries, blackberries to raspberries, all these foods are fantastically good for us, so tuck in!
In addition to food, as a health aspiring 65-year-old, I both supplement 1 gram of vitamin C twice a day and take an AGE Antioxidant containing Co-Q10, alpha lipoic acid, n-acetyl cysteine (NAC – as a precursor to glutathione which is the master antioxidant) and resveratrol as well as vitamin E and A – both beta-carotene and retinol. Many people think that there is no point supplementing glutathione because it is so rapidly oxidised, or sacrificed, to disarm oxidants, but it is also rapidly recycled by anthocyanidins in blue/red berries. So, combining the two reloads glutathione. This film shows how.

But how do we measure our antioxidant status?
My research team is working on exactly this challenge and we are finding that the ratio between reduced glutathione (GSH) and oxidised glutathione (GSSG) in red blood cells is probably the best biological determinant. We hope to introduce that into our panel of functional indicators, and research how it correlates with dietary intake and lifestyle habits as well as cognitive function.
We are due to launch a DRIfT Test as part of a global prevention initiative, which will be a 4 in 1 test
The UK Biobank has collected data on 500,000 people since 2006, inviting people to fill in questionnaires, give blood and carry out certain tests. We are funded by ‘Friends’ who pay £50/$60/€60 a year. So far we have collected data on 410,000 people and this number is growing by about a hundred a day.
In addition to taking the blood test, participants are invited to complete a validated online Cognitive Function Test (not a questionnaire), followed by a comprehensive 144 question Dementia Risk Index diet and lifestyle questionnaire which takes 20-25 minutes. This works out a person’s future risk and shows what’s driving the risk. This is a free service.
We run the UK’s leading dementia prevention charity which is running the prevention project together with Dr Tommy Wood, Assistant Professor at the University of Washington. “By tracking a person’s blood sugar, vitamin B, D and omega-3 status against changes in cognitive function over time, in addition to lifestyle factors such as sleep and physical activity, we can learn what really helps prevent cognitive decline.” says Dr Wood, the principal investigator for the study.
Citizen Science
All donations are put back into research, and the results of the research are shared back to the people.
This is science for the people, funded by the people, shared back with the people. We call them Citizen Scientists and we hope to reach a million people around the world within a year or so making this the biggest prevention-focussed study of its kind. The purpose of research is to help people. Too often great scientists do great studies, which get published and ignored. We have to face the fact that, in the UK as an example, the Government has commissioned four reports on mental health and Wellcome did a further independent report, all showing we have a cerebral tsunami with brain and mental health disorders ahead of every other disease.
They have ignored every single one.
Change is not going to come from the Government or the NHS. It is going to have to come from us, the people. I urge everyone in natural medicine to take the test themselves, share it with others and support us by becoming Friends and donating £50 a year, getting so much in return.
This is how we are funding our amazing research team. We are a lean, keen, small but mighty team.
Every donation, big or small, goes right back into helping people prevent these preventable and terrible diseases such as dementia.
Together, we can change the world.
We need to because time is running out.
We will lose our humanity if we don’t stop this brain drain.
—
Want to learn more about homocysteine and how to reclaim your brain? Join us for the Homocysteine Unplugged webinar.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
1 Lakhan, S.E., Kirchgessner, A. The emerging role of dietary fructose in obesity and cognitive decline. Nutr J 12, 114 (2013).
3 Yau PL, Castro MG, Tagani A, Tsui WH, Convit A. Obesity and metabolic syndrome and functional and structural brain impairments in adolescence.
Pediatrics. 2012 Oct;130(4):e856-64. doi: 10.1542/peds.2012-0324. Epub 2012 Sep
4 Zhang X, et al Midlife lipid and glucose levels are associated with Alzheimer’s disease. Alzheimers Dement. 2023
5 Fortier M, Castellano CA, St-Pierre V, Myette-Côté É, Langlois F, Roy M, Morin MC, Bocti C, Fulop T, Godin JP, Delannoy C, Cuenoud B, Cunnane SC. A ketogenic drink improves cognition in mild cognitive impairment: Results of a 6-month RCT. Alzheimers Dement. 2021 Mar;17(3):543-552. doi: 10.1002/alz.12206. Epub 2020 Oct 26. PMID: 33103819; PMCID: PMC8048678.
6 Crawford, M.A..; Sinclair, A.J.; Wang, Y.; Schmidt, W.F.; Broadhurst, C.L.; Dyall, S.C.; Horn, L.; Brenna, J.T.; Johnson, M.R.; Docosahexaenoic Acid Explains the Unexplained in Visual Transduction. Entropy 2023, 25, x. https://doi.org/10.3390/xxxxx
7 Basambombo LL, Carmichael PH, Côté S, Laurin D. Use of Vitamin E and C Supplements for the Prevention of Cognitive Decline. Ann Pharmacother. 2017 Feb;51(2):118-124. doi: 10.1177/1060028016673072. Epub 2016 Oct 5. PMID: 27708183.
8 Peng, M., Liu, Y., Jia, X. et al. Dietary Total Antioxidant Capacity and Cognitive Function in Older Adults in the United States: The NHANES 2011–2014. J Nutr Health Aging 27, 479–486 (2023). https://doi.org/10.1007/s12603-023-1934-9
9 Nurk E, Refsum H, Drevon CA, Tell GS, Nygaard HA, Engedal K, Smith AD. Intake of flavonoid-rich wine, tea, and chocolate by elderly men and women is associated with better cognitive test performance. J Nutr. 2009 Jan;139(1):120-7. doi: 10.3945/jn.108.095182. Epub 2008 Dec 3. PMID: 19056649.
10 Sesso HD, Manson JE, Aragaki AK, Rist PM, Johnson LG, Friedenberg G, Copeland T, Clar A, Mora S, Moorthy MV, Sarkissian A, Carrick WR, Anderson GL; COSMOS Research Group. Effect of cocoa flavanol supplementation for the prevention of cardiovascular disease events: the COcoa Supplement and Multivitamin Outcomes Study (COSMOS) randomized clinical trial. Am J Clin Nutr. 2022 Jun 7;115(6):1490-1500. doi: 10.1093/ajcn/nqac055. PMID: 35294962; PMCID: PMC9170467.











