We now know that today’s diet, lacking in brain-friendly fats and other nutrients, yet high in sugar and ultra-processed food, is likely to be shrinking our brains, dumbing us down and triggering a big increase in mental health problems. But it isn’t just nutrition that is creating the perfect storm for our mental demise.
The digital culture we exist in is pushing us towards a whole new paradigm of background stress. This is partly because the marketeers have learnt how to get us addicted to their products – applying a level of stress and variable reward to trick the brain’s reward system – leaving you with a ‘gotta have it’ feeling.
This mechanism of ‘variable reward’
This was first discovered in the 1930’s by the psychologist B.F. Skinner. He found that mice responded most frequently to reward-associated stimuli when the reward was given after a varying number of responses – so the animal didn’t know when it would get the prize. It seems we are no different; if we perceive a reward to be delivered at random, and if checking for that reward comes at little or no cost, we end up checking habitually.
So is this where smartphone addiction comes from?
This manipulation of the stress/reward response is one of the oldest mechanisms of the brain. It is both core for our survival, but also makes us more impulsive, manipulatable and, effectively, stupid.
Most of all, it makes us good consumers. Reward, based on dopamine, equals pleasure. We are living in space-age times with stone age minds and multinational companies have learnt how to get us hooked – literally neurochemically addicted to consuming their products.
We are being sold pleasure in the guise of happiness: the happy hour, the happy meal, happiness in a can. But joy and happiness are regulated by the neurotransmitter serotonin, not the latest special offer. And in fact, this pleasure-seeking may be counterproductive.
“The more pleasure you seek, the more unhappy you get” says Professor Robert Lustig, author of ‘Hacking the American Mind’. This is because too much dopamine (the ‘reward’ neurotransmitter) suppresses serotonin (the ‘happy’ neurotransmitter) and we end up feeling unhappy and depressed. This brain hijack may be why depression, suicide and psychiatric drug prescriptions have rocketed to the point where, in the UK and US (and probably elsewhere), there are almost twice as many prescriptions for psychiatric drugs per year than there are people.
“We are the most in debt, the most obese, the most medicated and the most drugged up adult population in human history” says Lustig. We have literally learnt how to fool our brains and in doing so have fooled ourselves, by creating addictive behaviours and addictive foods.
An example of this is what happens in your brain if you eat sugar and/or fat.
Sugar…just like cocaine and heroin?
Sugar, just like cocaine and heroin, stimulates dopamine and endorphins. It triggers the reward system but with overuse, leads to reward deficiency (1). Dr Candace Pert, Research Professor in the Department of Physiology and Biophysics at Georgetown University Medical Center in Washington DC, and author of the seminal book ‘The Molecules of Emotion’, was the first to point this out in no uncertain terms: “I consider sugar to be a drug, a highly purified plant product that can become addictive. Relying on an artificial form of glucose – sugar – to give us a quick pick-me-up is analogous to, if not as dangerous as, shooting heroin. (2)” At the time, this was heresy but, today, most people are well aware of this. But it’s not just sugar that’s feeding our addiction.
Neuropharmacologist Professor Paul Kenny, a Dubliner now working in his Manhattan lab at Mount Sinai Hospital, discovered this when he started feeding rats different diets. When he fed one group of rats either lots of sugary foods and another group lots of fatty foods, neither group would gain much weight. They’d control their intake and it would take over a month to see a small weight gain.
However, when he fed them a combination of 50% sugar and 50% fat, such as in a cheesecake, he noted the mice would “dive head first into a slice and gorge so vigorously that it covered its fur in blobs. It’s not pleasant.” After a binge on cheesecake they continued to graze, constantly eating food, he says, as if the off-switch telling them they were full had malfunctioned. “It completely changed them.” They stopped exercising and gained significant weight after only seven days. They also became addicted (3). When he took away the junk food and replaced it with healthy food they went on a hunger strike, refusing to eat it.
He even tried to stop them by giving them an electric shock to their feet. “We then warned the rats as they were eating—by flashing a light—that they would receive a nasty foot shock. Rats eating the bland chow would quickly stop and scramble away, but time and again the obese rats continued to devour the rich food, ignoring the warning they had been trained to fear. Their hedonic desire overruled their basic sense of self-preservation.”
Overeating, he found, juices up the reward systems in the brain — so much so, that in some people, it can overpower the brain’s ability to tell them to stop eating when they have had enough. As with alcoholics and drug addicts, the more they have, the more they want, creating a vicious cycle of dopamine resistance, eventually leading to the brain’s receptors for dopamine to shut down.
It seems dopamine, the brain’s main neurotransmitter of reward and desire, is the key.
Obese people and drug addicts have been shown to have less dopamine D2 receptors (D2R)s (4). People who are born with reduced levels of D2R are therefore at greater genetic risk of developing obesity and drug addiction – so you can be genetically predisposed to addiction. Researchers at Brookhaven National Laboratory and the Oregon Research Institute have shown that the reward system in obese people responds weakly to food, even to junk food(5). How does an individual overcome this absence of pleasure? By eating more pleasure foods to gain a temporary boost, thereby perpetuating the cycle. The researchers found that obese people may overeat just to experience the same degree of pleasure that lean individuals enjoy from less food.
Nicole Avena of the University of Florida, and others, have found that particular fats or sugars, sugars together with fats, and possibly salt, are the most addictive (6). A study by Professor David Ludwig of Boston Children’s Hospital suggests that highly processed, quickly digested fast carbs could trigger cravings (7). But research overall indicates that no one ingredient stokes food addiction better than the combo of fats and sugars, high in calories. Nature just doesn’t make these kinds of foods. Only the food industry does.
Similarly, cola drinks combine the stimulant caffeine, with sugar and salt, to make you drink more. And we crave sugary food and drink even more when fructose is used instead of glucose. Why? Because our cells run on glucose and quickly feedback when we’ve had enough. Fructose (or high fructose corn syrup, derived from corn) takes longer to send us that signal, leading us to consume more. No wonder then that glucose has been replaced by fructose and is a key ingredient in today’s ultra-processed foods.
Are you addicted to your smartphone?
Of all the changes that have taken place in the 21st century, the ‘digital revolution’ has changed our world beyond recognition, seemingly speeding up time. Yes, our diet and environment have changed a lot, but what’s really changed, especially in cities that now house half of humanity and an estimated two-thirds of the world’s population by 2035, is the pace of life. People all over the world are sleeping less, having less downtime, feeling more anxious and stressed and burning out at a far higher rate. This is reflected in the increasing rate of work absenteeism, depression and suicide, especially in cities.
The speeding up of communication – emails, smartphones and digital media – means that we are supposed to react to demands, and are bombarded with them, at an ever-increasing speed.
We have literally become addicted to our phones(8). The average person picks up their phone 352 times a day – more than every three minutes, and swipes it thousands of times a day. A UK survey reports 62% cannot make it through dinner without checking their phone. Almost half of us report anxiety if we don’t have our phone, or a signal, suffering ‘nomophobia’. We are going to sleep with our phones and checking them first thing on waking up. One survey found that one in ten university students in the US admitted to having checked their smartphones during sex!
Why? Basically, to sell stuff. “I feel tremendous guilt,” admitted Chamath Palihapitiya, former Vice President of User Growth at Facebook, to an audience of Stanford students. “The short-term, dopamine-driven feedback loops that we have created are destroying how society works.” Whether it’s Facebook, Instagram, Twitter, Snapchat, LinkedIn or any other platform, the core design is to get your attention, then show you ads tailored to your attributes and behaviours which the technology learns about you. Facebook, for example, has learnt how to do this with prompts, swipe downs, red icons that you press and don’t know what you receive. Is it a ‘like’? Do I have more ‘friends’? Or has another person ‘linked’ to me on LinkedIn etc.
Facebook even knows when you’re feeling ‘insecure’, ‘worthless’ and ‘need a confidence boost’ or are ‘bored’, and can make sure you receive a notification of a ‘like’ at just the right time to keep you hooked. If you find yourself checking your phone at the slightest feeling of boredom, purely out of habit, know that programmers work very hard behind the screens to keep you doing exactly that. A study of 143 undergraduates at the University of Pennsylvania, limiting use to 30 minutes a day versus a control group found significant reductions in loneliness and depression (9). The researchers concluded, “Our findings strongly suggest that limiting social media use to approximately 30 minutes per day may lead to significant improvement in well-being.”
Whether it’s a text, a notification or a ‘like’, just like sugar, this digital consumption triggers a reward signal in our brains. The marketing algorithms schedule the precise times to deliver our digital diet and serve up the extra addictive quality of a variable reward.
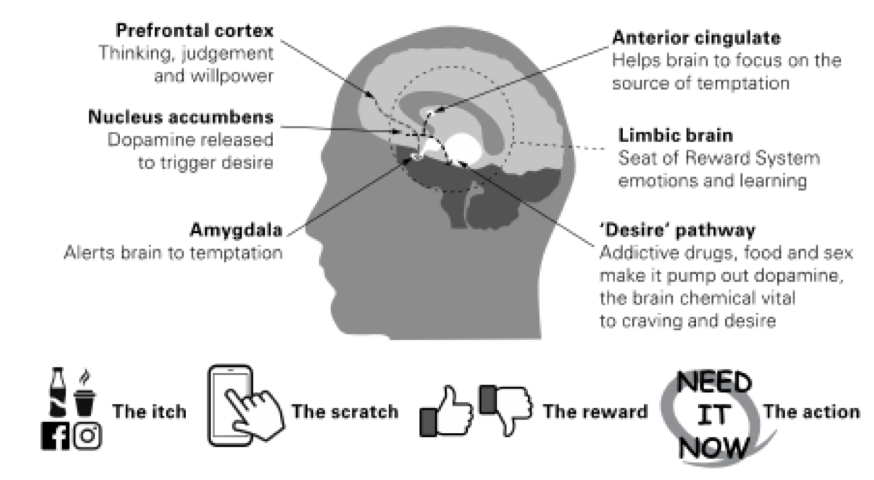
Your brain’s reward system
It’s to do with a tiny organ in the central hippocampal area of the brain called the nucleus accumbens. This is the headquarters of our dopamine-based ‘reward’ system.
The more dopamine you release the more receptors shut down, so you seek more pleasurable behaviours and foods. Insidiously and unknowingly your brain has been hijacked and the symptoms you feel are the direct consequences of an intended addiction. Gambling, gaming, overeating, sex, drugs, food, social media and other digital addictions are all part of it. We end up needing this constant stimulation and, to fuel that, need instant energy foods and drinks – sugar and coffee.
Alcohol – the opiate of the masses
Whether you’ve become addicted to sugar, food, caffeinated drinks, social media, gambling, gaming or non-stop stimulation, or simply get caught in the stress trap, perhaps due to work and life demands and debts, this often results in an inability to switch off with a background feeling on anxiety and stress without alcohol, and difficulty sleeping.
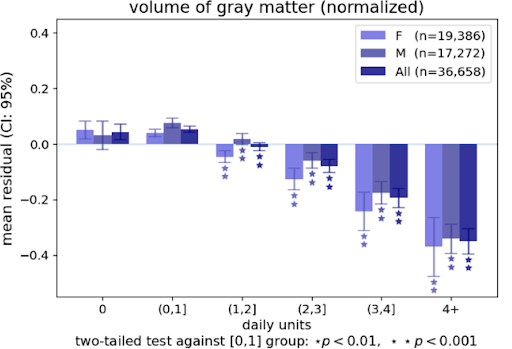
You may find, in time, that your need for alcohol increases – from a glass a night to two, three, half a bottle or even more. Alcohol, a well-established neurotoxin (10), surely is the opiate of the masses. Consumption keeps going up. It’s the currency of a good time, normalised as a response to stress, glorified in movies and at the core of our modern culture, with a 1.5 trillion dollar industry, expected to rise to 2 trillion by 2027 (11), promoting its use. While smoking has become frowned upon, anything other than heavy drinking is considered socially acceptable. Yet according to WHO alcohol is in the top five causes of death and disability, and has become the most common cause of death in men under 50 (and soon will be for women), accounting for one-fifth of all deaths under 50 and almost 30,000 deaths a year overall, roughly a third that of smoking and ten times more than opioids (inc heroin) and is ranked more harmful than any other drug, including opioids (12). This addictive drug is so socially acceptable that governments avoid attempts to curtail its use for fear of voter reprisals.
A commonly unknown fact is that death or disability from alcohol doesn’t only occur in heavy drinkers. The risk goes up exponentially with the quantity you drink. The good news is that small reductions have big positive effects on your health. To make this real, a 12.5% vol. bottle of wine contains 75g alcohol: drinkers who have 2/3rds of a bottle of wine (two large glasses) or the equivalent 50g of alcohol, have a lifetime risk of death of 16%. But one medium glass (175ml) of wine (17.5g of alcohol) brings that risk below 1%. In terms of mitigating serious health risks, including death, the advice of the UK government’s former advisor, Professor David Nutt, is for women to consume no more than 15g of alcohol per day and for men no more than 20g alcohol per day, and to have at least two alcohol-free days per week. Sadly, Professor Nutt was sacked for saying that alcohol was a ‘time bomb’ and more dangerous than Ecstasy, but the statistics point to this being true.
The trouble is, when you get stuck in the cycle of seeking rewards, needing stimulants and relaxants, you become more tired, more anxious and may even have started to feel more depressed.
When things get bad and you visit your doctor they may prescribe antidepressants, tranquillisers (short-term use only) or sleeping pills. Others learn to use illicit uppers and downers.
Are you addicted to stimulants?
The other major acceptable and glorified drug is caffeine, mainly in the form of coffee, although many people don’t realise that strong tea has as much caffeine as a regular cup of coffee. Like sugar, alcohol and our digital diet, it stimulates dopamine release and the feeling of pleasure or reward. Imagine a day with no coffee, tea, sugar, chocolate or that well-earned glass of something! If you shout, ‘No way!’ there is a very real possibility that you have some level of addiction to these stimulants. This can range from a mild addiction that you can live with quite happily to a major problem that is controlling your life.
However, whatever the level of addiction, the net consequence is always less energy, not more. One of my clients, Bobbie, serves as a case in point. She was already eating a healthy diet and took a sensible daily programme of vitamin and mineral supplements. She had only two problems: a lack of energy in the morning and occasional headaches. She also had one vice: three cups of coffee a day. After some persuasion, she agreed to stop the coffee for a month. To her surprise, her energy levels rose and the headaches stopped.
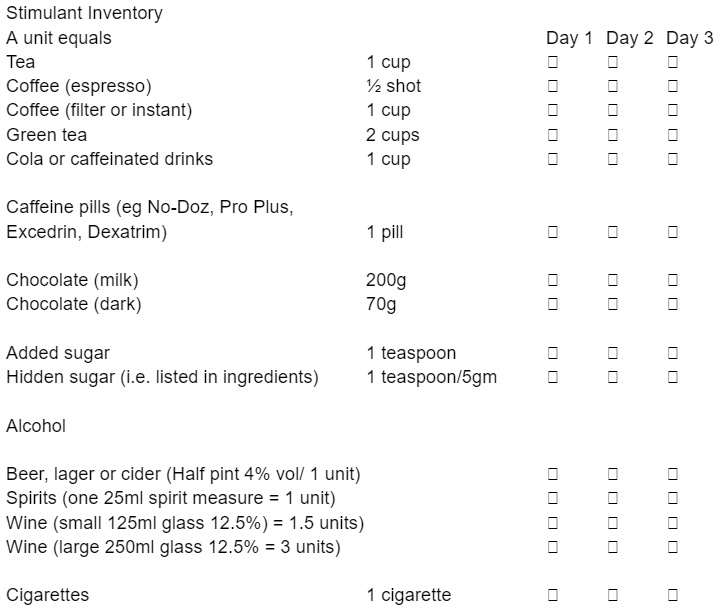
Like Bobbie, it’s useful to audit your stimulant consumption from time to time. Using a Stimulant Inventory below can be helpful, but in making an accurate assessment of your current relationship to stimulants, you need to be honest with yourself about how you use them. There’s a space for alcohol which, while not a stimulant, still triggers those dopamine receptors.
It’s useful to write down the time of day you consume the above and to spend time thinking about what your relationship to these substances is.
- Do you, for example, ever buy sweets and hide the wrappers so other people don’t know you’ve eaten them?
- Do you swoon at the dessert menu in restaurants?
- How much do you think about and look forward to that morning cup of coffee or a mid-morning second cup?
- How important is that drink after work?
- Does everyone really know how much you smoke?
- Have you cranked up your caffeine intake to ‘double espresso’ equivalent drinks using more coffee at home than you used to?
- Do you need more to get a ‘kick’ if you even get one, or does coffee now just relieve the fuzzy tiredness you feel without it?
This kind of relationship to stimulants, often cloaked in an attitude that they are just some of the innocent pleasures of life, is indicative of an underlying chemical imbalance that depletes your energy and peace of mind and, at its worst, feeds into mental health issues.
Coffee and Caffeine Withdrawal and Sleep
If you wake up feeling good and can function without a coffee, and have no major mental health issues, sleeping well for example, but enjoy one coffee a day which will give you a dopamine kick, that’s not a problem. The best measure of your relationship with coffee or caffeine, and whether your brain has ‘downregulated’ dopamine and adrenaline receptors is what happens when you quit. If the answer is nothing then there’s no issue. If, on the other hand, you get a variety of withdrawal symptoms (13), including headaches, tiredness and irritability that means your neurotransmitter receptors have downregulated and it will take a few days for them to upregulate and bring you back to normal. For many just one cup of coffee a day can result in withdrawal effects if stopped (14). It’s also worth knowing that coffee, or caffeine, consumed 6 hours before sleep, which is about as long as caffeine stays in the system, is associated with disturbed sleep (15) – either difficulty falling asleep or waking in the night so, at least, it is wise to consume no caffeine after noon, especially if you have issues with sleeping.
Tea or coffee?
The caffeine in both coffee and tea increases the release of adrenalin, cortisol and dopamine in your body and brain, while inhibiting the absorption of adenosine, a brain-calming chemical. The release of adrenaline into your system gives you a temporary boost, but frequently makes you fatigued and depressed later. If you take more caffeine to counteract these effects, you end up spending the day in an agitated state, and might find yourself jumpy and edgy by night.
Tea contains caffeine, but also theanine, which has a more calming amino acid shown to enhance cognitive abilities (16). It also protects GABA receptors, which is the brain’s adrenalin off switch. Overall then, tea is better for you. Green tea may also have some benefits over black tea (the same plant, but processed differently such that green tea contains more antioxidants and polyphenols, which are good guys as far as our bodies are concerned).
Benefits or excuses?
Many things could be written on the apparent benefits of tea, coffee, even some forms of alcohol. We read about the beneficial effects of resveratrol in red wine, polyphenols in coffee and cacao and other antioxidants in tea. However, the nature of ANY dependence creates a psychological set of ‘excuses’ that we use to justify our addictive behaviour.
This could be anything from ‘that’s a lovely sauce’ (sugar), ‘a little bit of what you fancy won’t harm you’ ‘I’m so stressed I have to have a drink’, ‘I’ve got to focus so I need a coffee’ and so on. Of course, all these substances work, otherwise we wouldn’t be attracted to them and, in that sense, mindful consumption in certain circumstances makes sense. For example, if someone experiences a shock, a sugary drink can help. And when a deadline looms and you need to burn the candle at both ends, caffeine can certainly help.
The issue here is to understand how the combination of sugar, caffeinated stimulants, alcohol, tech and social media addiction, shopping, gambling, gaming and so on can hijack your brain’s natural reward system and result in the opposite – you feeling more tired, anxious, unfulfilled and depressed. If that’s happened to you, rest assured there are some simple suggestions that will help you reclaim your brain’s full potential for feeling good, energised, clear, focussed and purposeful.
Simple ways to win back your brain
- Limit your time spent on social media – 30 minutes a day max is a good target but you may need to build down to this. Turn your phone off (or to ‘airplane’ mode) at least an hour before bed and keep it that way for at least an hour in the morning. If you have to have it on, don’t check social media for a couple of hours.
- Limit your intake of caffeine to under 100 grams a day – that’s one strong cup of coffee or two weaker cups of tea. If you have a second cup, use the same tea bag, or have a filter coffee ‘run through’. Avoid all caffeine after noon.
- Avoid buying food that contains added sugar, dates or raisins – if in doubt, read the label and remember sugar is often disguised as high fructose corn syrup. When looking at food labels remember 5g is a teaspoon of sugar and foods with more than 22.5g per 100g of sugar are considered high sugar and those with 5g or less per 100g are considered low sugar. Ideally, only have sugar in whole fresh fruits. Fruit juice is also high in sugar so best avoided or limited.
- Limit your daily intake of alcohol to 20 grams, or a maximum of two small glasses (125ml is one small glass) of wine. Have at least two days a week alcohol-free.
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
References
1 P. Holford, How to Quit Without Feeling S**t, Piatkus, 2008.
2 P. Holford, How to Quit Without Feeling S**t, Piatkus, 2008.
3 P.M. Johnson and P.J. Kenny ‘Dopamine D2 receptors in addiction-like reward dysfunction and compulsive eating in obese rats’, Nature Neuroscience (2010), vol. 13(5), pp. 635-641.
6 N.M. Avena and M.S. Gold, ‘Food Addiction – Sugars, Fats and Hedonic Eating’, Addiction (2011), vol. 106(7), pp. 1214-1215.
7 B. Lennerz et al., ‘Effects of dietary glycemic index on brain regions related to reward and craving in men’ The American Journal of Clinical Nutrition, Volume 98, Issue 3, 1 September 2013, Pages 641–647
14 Juliano LM, Griffiths RR. A critical review of caffeine withdrawal: empirical validation of symptoms and signs, incidence, severity, and associated features. Psychopharmacology (Berl). 2004 Oct;176(1):1-29. doi: 10.1007/s00213-004-2000-x. Epub 2004 Sep 21. PMID: 15448977.
15 Drake C, Roehrs T, Shambroom J, Roth T. Caffeine effects on sleep taken 0, 3, or 6 hours before going to bed. J Clin Sleep Med. 2013 Nov 15;9(11):1195-200. doi: 10.5664/jcsm.3170. PMID: 24235903; PMCID: PMC3805807.
16 Anas Sohail A, Ortiz F, Varghese T, Fabara SP, Batth AS, Sandesara DP, Sabir A, Khurana M, Datta S, Patel UK. The Cognitive-Enhancing Outcomes of Caffeine and L-theanine: A Systematic Review. Cureus. 2021 Dec 30;13(12):e20828. doi: 10.7759/cureus.20828. PMID: 35111479; PMCID: PMC8794723.
Further info