Why Gut Health Matters for Brain Health More Than You Think
Why Gut Health Matters for Brain Health More Than You Think

Why Some Brains Improve and Others Don’t
Many people are doing more than ever to protect their brain. They eat well. Take supplements. Exercise. Stay mentally active.
Yet outcomes vary dramatically.
Some improve. Others stall. A few decline despite doing everything “right”.
The missing question is not what else to add, but what environment those interventions are landing in.
Cognitive decline rarely stems from one isolated failure. It emerges when the body’s internal environment no longer supports protection, repair, and resilience. This systems-based understanding underpins the work of Food for the Brain, and explains why gut health plays a central role in our COGNITION brain upgrade programme.
The terrain model of brain health
In medicine, there is a long-established principle that disease does not arise from a trigger alone, but from the biological environment in which that trigger operates. This is often described as the terrain.
From a brain health perspective, terrain includes inflammatory load, metabolic health, immune balance, nutrient availability, and cellular repair capacity. These systems interact constantly. When they stay in balance, the brain shows remarkable resilience. When they become disrupted, vulnerability increases.
Neurodegenerative conditions, including Alzheimer’s disease, are now understood to arise from multiple interacting biological pressures rather than a single pathological process. Many of these systems are shaped upstream by gut related processes.
The gut as a regulator, not a root cause
The gut is often discussed as if it were a standalone digestive organ. In reality, it plays a regulatory role in shaping systemic inflammation, metabolic function, and immune signalling.
When gut barrier integrity is compromised, bacterial components such as lipopolysaccharides can enter circulation. This process increases immune activation and drives chronic low-grade inflammation, a state strongly associated with insulin resistance and cognitive decline [1,2].
In this context, gut dysfunction is not “causing” brain disease. It is influencing the conditions in which brain protection and repair either succeed or struggle.
Why prevention struggles in an inflamed system
Brain health interventions that we talk about here at Food for the Brain do not operate in isolation. Their effectiveness depends on the biological environment in which they are applied.
This is particularly clear in nutritional research.
B vitamin supplementation has been shown to slow brain atrophy, but only in individuals with raised homocysteine levels and a metabolic environment that allows normal methylation processes to function [3]. Similarly, omega 3 fatty acids support neuronal membrane structure and signalling, yet their cognitive benefits are reduced in the presence of inflammation and insulin resistance [4].
Inflammation interferes with digestion, absorption, transport, and cellular uptake of nutrients. Pro inflammatory cytokines also impair intracellular metabolic pathways, shifting the body toward defence rather than repair. In this terrain, even well evidenced interventions may have limited effect.
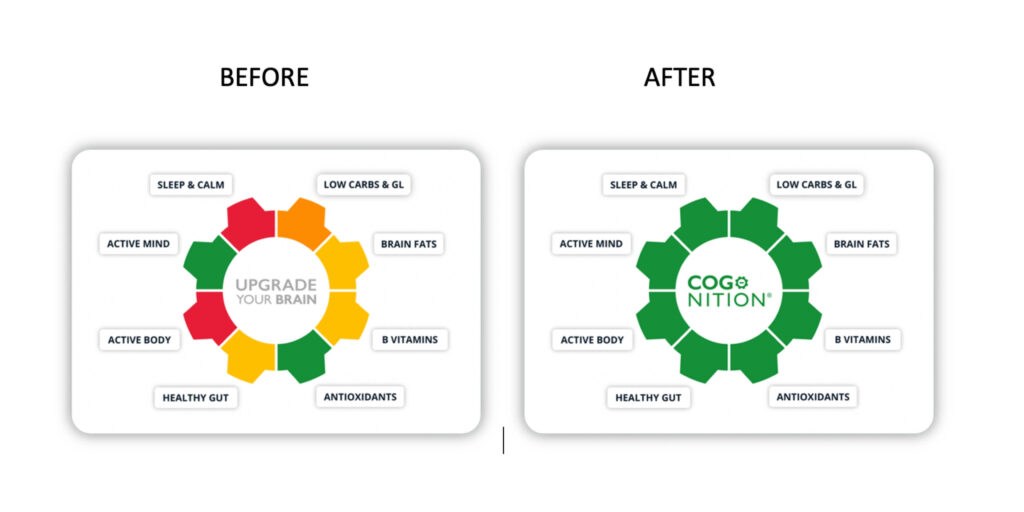
The same principle applies to lifestyle strategies. Physical activity, cognitive stimulation, and stress reduction are all protective, but their impact is blunted when inflammatory and metabolic pressures remain unaddressed. That is why in COGNITION we target all 8 modifiable nutrition and lifestyle factors, so that you are not just targeting a specific nutrient but you are changing the environment.
Microbes, inflammation, and brain vulnerability
Human studies consistently show that individuals with cognitive impairment or Alzheimer’s disease have altered gut microbiome profiles alongside higher levels of systemic inflammatory markers [5].
This does not demonstrate that microbes cause dementia. What it does show is that microbial imbalance contributes to inflammatory load, which in turn increases brain vulnerability.
Over time, this vulnerability can translate into accelerated cognitive decline.
For this reason, the COGNITION brain upgrade programme actively addresses gut health as one of eight modifiable factors that influence dementia risk. Gut microbes actively shape the internal environment in ways that can either accelerate neurodegeneration or help slow it.
The metabolic bridge between gut and brain
The gut also plays a critical role in metabolic regulation.
Chronic gut driven inflammation worsens insulin resistance, reducing glucose uptake by brain cells. Impaired brain glucose metabolism is a recognised feature of cognitive decline and has led some researchers to describe Alzheimer’s disease as a form of brain specific metabolic failure [6,7].
In this model, the gut is not peripheral. It contributes upstream to the metabolic conditions that determine whether the brain can access adequate fuel to function and repair.
Again, the implication is not that gut health alone determines brain fate. It is that brain health strategies are less effective when the metabolic and inflammatory terrain is unfavourable.
Why Brain Health Advice Works for Some People and Not Others
A terrain based perspective offers something often missing from prevention conversations.
Understanding.
When people follow advice carefully and still do not improve, clinicians too often frame the explanation as lack of compliance or genetics. Systems thinking offers a different interpretation.
The tools may be appropriate but the environment may not yet support repair.
This reframes prevention as a personalised process rather than a universal checklist. Understanding an individual’s internal terrain helps identify where effort should go.
This is why Food for the Brain offers two complementary forms of assessment: the free, validated Cognitive Function Test and optional at home blood testing to assess key modifiable risk markers such as homocysteine, omega 3 status and glutathione.
The answer is not found in one nutrient
Viewing brain health through a terrain lens shifts prevention away from adding isolated solutions and toward restoring balance across systems.
The future of brain health does not lie in targeting one nutrient, one habit, or one molecule.
It lies in creating an internal environment where protection, repair, and resilience are possible.
Brains do not fail because one thing goes wrong. They decline when the terrain no longer supports them.
And that terrain forms quietly and cumulatively long before symptoms appear.
Next Steps
- Learn more about how gut health impacts brain health in our upcoming webinar here
- Complete the FREE, validated Cognitive Function Test today so you can get instant insight into your current brain health status
- Order your at home blood test here to get more personalised data on your body and contribute to our on going research
References:
- Cani PD, Amar J, Iglesias MA, Poggi M, Knauf C, Bastelica D, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56(7):1761–72.
- Hotamisligil GS. Inflammation and metabolic disorders. Nature. 2006;444(7121):860–7.
- Smith AD, Smith SM, de Jager CA, Whitbread P, Johnston C, Agacinski G, et al. Homocysteine-lowering by B vitamins slows the rate of accelerated brain atrophy in mild cognitive impairment. Proc Natl Acad Sci U S A. 2010;107(31):14187–92.
- Jernerén F, Elshorbagy AK, Oulhaj A, Smith SM, Refsum H, Smith AD. Brain atrophy in cognitively impaired elderly: the importance of long-chain omega-3 fatty acids and B vitamin status in a randomized controlled trial. Am J Clin Nutr. 2015;102(1):215–21.
- Vogt NM, Kerby RL, Dill-McFarland KA, Harding SJ, Merluzzi AP, Johnson SC, et al. Gut microbiome alterations in Alzheimer’s disease. Sci Rep. 2017;7(1):13537.
- Craft S. Insulin resistance and Alzheimer’s disease pathogenesis: potential mechanisms and implications for treatment. Arch Neurol. 2009;66(3):300–5.
- de la Monte SM, Wands JR. Alzheimer’s disease is type 3 diabetes–evidence reviewed. J Diabetes Sci Technol. 2008;2(6):1101–13.