Do supplements really help when it comes to cognitive decline or are they money wasted down the toilet?!
We believe that the science supports the use of correct supplementation in order to reduce risk of dementia and Alzheimer’s – so what is going on and what does the research really say?
The WHO report saying supplements are ‘not recommended’
A 2018 report by the WHO states: ‘Vitamins B and E, PUFA and multi-complex supplementation should not be recommended to reduce the risk of cognitive decline and/or dementia.’
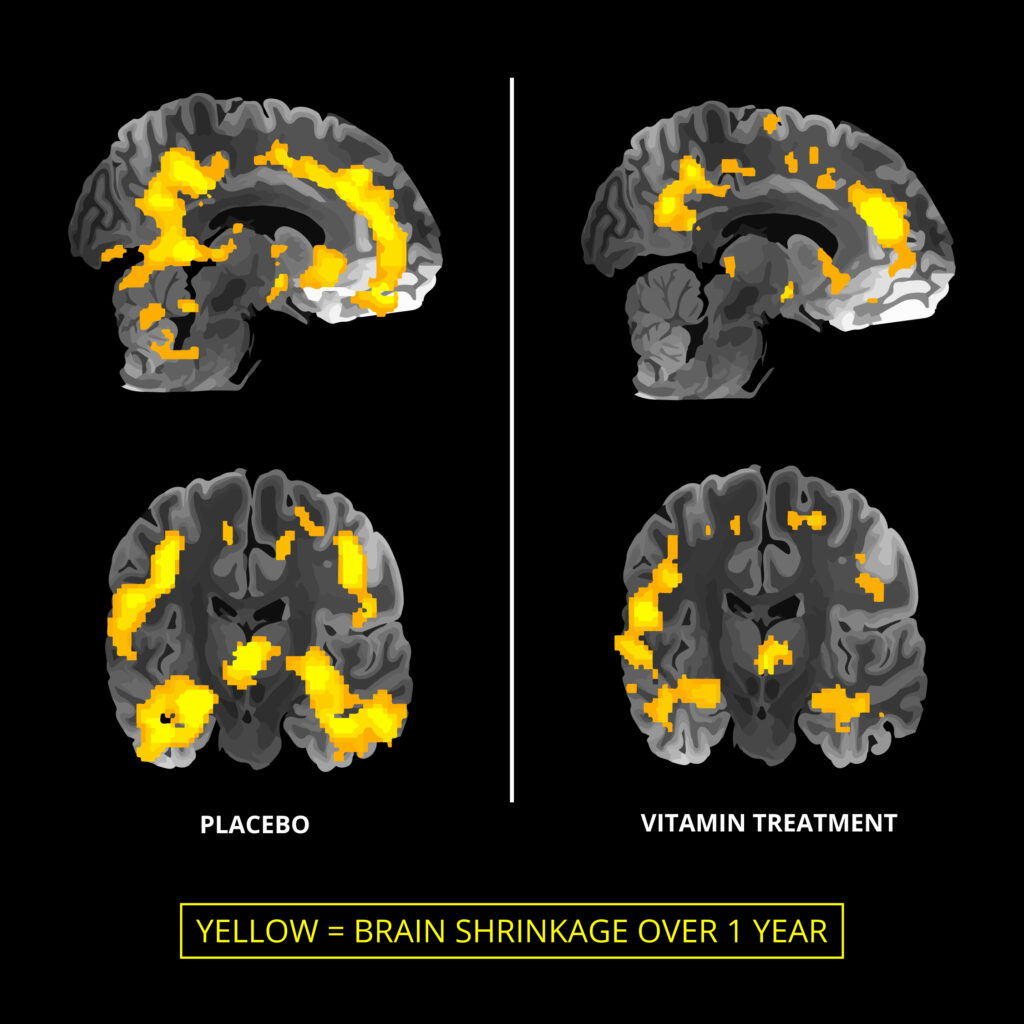
This 2018 WHO review makes no reference at all to the effect of B vitamins in slowing brain atrophy (1) and in improving cognition (2) in the rather large sub-group, estimated to be up to half of those over 65, with raised homocysteine. After all, why would B vitamins be expected to have an effect in those not deficient?
On closer inspection, three of the four cited studies in the WHO document are actually one meta-analysis (which is a statistical process of analysing and combining results from several similar studies). It cites only one paper which considered B vitamins (the one part-funded by Alzheimer’s Research UK) which showed a clear effect of B vitamins improving cognition in those with raised homocysteine, and one study on omega-3 DHA, which also shows clear benefit as stated in the studies summaries. Thus, it misrepresented the study that ARUK part funded on B vitamins as negative, when they had a clearly positive effect.
The only cited B vitamin study (2) states, “The mean plasma total homocysteine was 30% lower in those treated with B vitamins relative to placebo. B vitamins stabilised executive function (CLOX) relative to placebo. There was significant benefit of B-vitamin treatment among participants with baseline homocysteine above the median in global cognition, episodic memory and semantic memory. Clinical benefit occurred in the B-vitamin group for those in the upper quartile of homocysteine at baseline in global clinical dementia rating score… In this small intervention trial, B vitamins appear to slow cognitive and clinical decline in people with mild cognitive impairment (MCI), in particular in those with elevated homocysteine.”
The only cited study on omega-3 fish oils (3) states, “The fish oil group showed significant improvement in short-term and working memory.” The 12-month change in memory was significantly better in the fish oil group. This study suggested the potential role of fish oil to improve memory function in MCI subjects.
So, even based on its own cited evidence, the benefit of both B vitamins and omega-3 fish oils is supported.
How the WHO statement then recommends the opposite, ‘Vitamins B and E, PUFA and multi-complex supplementation should not be recommended to reduce the risk of cognitive decline and/or dementia.’ beggars belief. But the real problem is not the shoddy research, from 2015, used to produce this report but that it is out of date. The WHO ‘rules’ for this report was to ignore any study that was more than 5 years old, yet the WHO authors republished this same report, with the same conclusions, in 2022, by then redundant according to its own rules!
What we’ve learned since 2018
Also, much has been learnt, and published, since 2018. There is now evidence that homocysteine lowering B vitamins are most effective in those with sufficient omega-3 status and omega-3 fish oils are most effective in those with low homocysteine. This is clinical confirmation of the known mechanism of co-dependence and illustrates why the WHO document is now out of date. We prefer published, peer-reviewed reviews such as the editorial in the American Journal of Clinical Nutrition in 2021 (4) and a meta-analysis in 2023 (5).
Additionally, since 2018, there have been at least 17 studies (6-22), including both randomised controlled trials and cohort studies which show benefit of either omega-3 fish oil supplementation, or higher intake from seafood with resultant higher omega-3 blood levels, in reducing risk for and incidence of dementia or cognitive decline.
This is another example showing why the WHO document is no longer current and relevant. Yet leading Alzheimer’s charities such as the Alzheimer’s Society and Alzheimer’s Research UK (ARUK – who part funded the highly effective B vitamin trial) still refer to this redundant report.
With regard to multivitamins, the latest meta-analysis states (7), “The meta-analysis of COSMOS substudies showed clear evidence of multivitamin-mineral benefits on global cognition and episodic memory; the magnitude of effect on global cognition was equivalent to reducing cognitive ageing by 2 years”. B vitamins, given to those with raised homocysteine, are much more effective than multivitamins given to all – and more effecctive in those with sufficient omega-3 status.
Summary
In conclusion, the 2018 WHO report is so sloppy, and out of date – by its own rules. It would be wise for WHO to withdraw this misleading report and certainly for both ARUK and the Alzheimer’s Society and any other Alzheimer’s or dementia organisations to stop referring to it in the context of omega-3, B vitamins or multivitamins, if they are to maintain credibility in being science-based.
Note: Many people are not aware that the WHO is no longer only funded by donations from the countries that it is supposed to serve but is now also privately funded, with the second largest funder being the Bill Gates Foundation, which accounts for 10% of its budget, leading to questions over influences on its agenda.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
1. Smith AD, Smith SM, de Jager CA, Whitbread P, Johnston C, Agacinski G, et al. Homocysteine-lowering by B vitamins slows the rate of accelerated brain atrophy in mild cognitive impairment: a randomized controlled trial. PloS one 2010;5(9):e12244.
2. de Jager CA, Oulhaj A, Jacoby R, Refsum H, Smith AD. Cognitive and clinical outcomes of homocysteine-lowering B-vitamin treatment in mild cognitive impairment: a randomized controlled trial. International journal of geriatric psychiatry 2012;27(6):592-600.
3. Lee et al 2013 – https://pubmed.ncbi.nlm.nih.gov/22932777/
4. Smith AD, Jernerén F, Refsum H. ω-3 fatty acids and their interactions. Am J Clin Nutr 2021;113(4):775-8.
5. Fairbairn P, Dyall SC, Tsofliou F. The effects of multi-nutrient formulas containing a combination of n-3 PUFA and B vitamins on cognition in the older adult: a systematic review and meta-analysis. The British journal of nutrition 2023;129(3):428-41.
6. Liu X, Zhuang P, Li Y, Wu F, Wan X, Zhang Y, et al. Association of fish oil supplementation with risk of incident dementia: A prospective study of 215,083 older adults. Clinical nutrition (Edinburgh, Scotland) 2022;41(3):589-98.
7. Vyas CM, Manson JE, Sesso HD, Cook NR, Rist PM, Weinberg A, et al. Effect of multivitamin-mineral supplementation versus placebo on cognitive function: results from the clinic subcohort of the Cocoa Supplement and Multivitamin Outcomes Study (COSMOS) randomized clinical trial and meta-analysis of 3 cognitive studies within COSMOS. Am J Clin Nutr 2024;119(3):692-701.
8. Jerneren F, Cederholm T, Refsum H, Smith AD, Turner C, Palmblad J, et al. Homocysteine Status Modifies the Treatment Effect of Omega-3 Fatty Acids on Cognition in a Randomized Clinical Trial in Mild to Moderate Alzheimer’s Disease: The OmegAD Study. Journal of Alzheimer’s disease : JAD 2019.
9. Rouch L, Virecoulon Giudici K, Cantet C, Guyonnet S, Delrieu J, Legrand P, et al. Associations of erythrocyte omega-3 fatty acids with cognition, brain imaging and biomarkers in the Alzheimer’s disease neuroimaging initiative: cross-sectional and longitudinal retrospective analyses. Am J Clin Nutr 2022;116(6):1492-506.
10. He X, Yu H, Fang J, Qi Z, Pei S, Yan B, et al. The effect of n-3 polyunsaturated fatty acid supplementation on cognitive function outcomes in the elderly depends on the baseline omega-3 index. Food & function 2023;14(21):9506-17.
11. Doughty KN, Blazek J, Leonard D, Barlow CE, DeFina LF, Omree S, et al. Omega-3 index, cardiorespiratory fitness, and cognitive function in mid-age and older adults. Prev Med Rep 2023;35:102364.
12. Loong S, Barnes S, Gatto NM, Chowdhury S, Lee GJ. Omega-3 Fatty Acids, Cognition, and Brain Volume in Older Adults. Brain Sci 2023;13(9).
13. Maltais M, Lorrain D, Léveillé P, Viens I, Vachon A, Houeto A, et al. Long-chain Omega-3 fatty acids supplementation and cognitive performance throughout adulthood: A 6-month randomized controlled trial. Prostaglandins, leukotrienes, and essential fatty acids 2022;178:102415.
14. Andriambelo B, Stiffel M, Roke K, Plourde M. New perspectives on randomized controlled trials with omega-3 fatty acid supplements and cognition: A scoping review. Ageing Res Rev 2023;85:101835.
15. Wei BZ, Li L, Dong CW, Tan CC, Xu W. The Relationship of Omega-3 Fatty Acids with Dementia and Cognitive Decline: Evidence from Prospective Cohort Studies of Supplementation, Dietary Intake, and Blood Markers. Am J Clin Nutr 2023;117(6):1096-109.
16. Grande de França NA, Díaz G, Lengelé L, Soriano G, Caspar-Bauguil S, Saint-Aubert L, et al. Associations Between Blood Nutritional Biomarkers and Cerebral Amyloid-β: Insights From the COGFRAIL Cohort Study. The journals of gerontology Series A, Biological sciences and medical sciences 2024;79(1).
17. Sasaki N, Jones LE, Carpenter DO. Fish consumption and omega-3 polyunsaturated fatty acids from diet are positively associated with cognitive function in older adults even in the presence of exposure to lead, cadmium, selenium, and methylmercury: a cross-sectional study using NHANES 2011-2014 data. Am J Clin Nutr 2024;119(2):283-93.
18. van Soest APM, van de Rest O, Witkamp RF, Cederholm T, de Groot L. DHA status influences effects of B-vitamin supplementation on cognitive ageing: a post-hoc analysis of the B-proof trial. European journal of nutrition 2022;61(7):3731-9.
19. Gao J, Fan H, Wang X, Cheng Y, Hao J, Han S, et al. Association between serum omega-3 PUFAs levels and cognitive impairment in never medically treated first-episode patients with geriatric depression: A cross-sectional study. J Affect Disord 2024;346:1-6.
20. He Y, Huang SY, Wang HF, Zhang W, Deng YT, Zhang YR, et al. Circulating polyunsaturated fatty acids, fish oil supplementation, and risk of incident dementia: a prospective cohort study of 440,750 participants. GeroScience 2023.
21. Chedid G, Malik A, Amangurbanova M, Khraishah H, Welty FK. Docosahexaenoic Acid Levels and Omega-3 Index, but Not Eicosapentaenoic Acid Levels, Are Associated With Improved Cognition in Cognitively Healthy Subjects With Coronary Artery Disease. Arteriosclerosis, thrombosis, and vascular biology 2022.
22. Duchaine CS, Fiocco AJ, Carmichael P-H, Cunnane SC, Plourde M, Lampuré A, et al. Serum ω-3 Fatty Acids and Cognitive Domains in Community-Dwelling Older Adults from the NuAge Study: Exploring the Associations with Other Fatty Acids and Sex. The Journal of nutrition 2022;152(9):2117-24.
Further info