The Four Horsemen of the Mental Health Apocalypse #1 – Brain Fats & Methylation
By Patrick Holford. This is part one, read part two here.

Few people realise the catastrophic decline in mental health that has occurred over the past 50 years.
—
‘Brain health conditions have become a global health emergency,’ according to the Federation of European Neuroscience Societies last year (1).
Globally, 15 per cent of all disability is due to brain and mental health disorders. The lifetime cost of Alzheimer’s in 2022 was estimated to be €1.2 trillion across the EU which is half the UK’s total GDP! This burden and costs exceeds that of all diseases, including cancer and heart disease. But most worrying are the trends of falling IQ at a rate of about 7 per cent a generation and the steady increase in young people with four in ten now reporting persistent feelings of sadness or hopelessness and almost a quarter (22 per cent) contemplating suicide (2).
On this flight path, by 2080, suicide may well become the leading cause of death in those under 24. Also, more than a third of children will have severe neurodevelopmental impairment, defined as significantly below the norm for IQ. That’s the conclusion of Professor Michael Crawford who discovered the essentiality of omega-3 DHA for the brain. Alarmingly, brain size, deduced from cranial capacity of skulls, has shrunk by a staggering 20 per cent over a mere 30,000 years. It took over six million years for brain size to increase from that of a chimpanzee (350cc) to a peak of 1,600 to 1,700 cc with Cro Magnon man thirty thousand years ago. Today, brain size averages 1,350cc (3). There is no question that we are devolving mentally with an endless escalation of rates of ADHD, autism, depression, anxiety, insomnia, schizophrenia, dementia and Alzheimer’s, as well as strokes, Parkinson’s and multiple sclerosis.
The big question is: why?
—
Introducing the four horsemen…
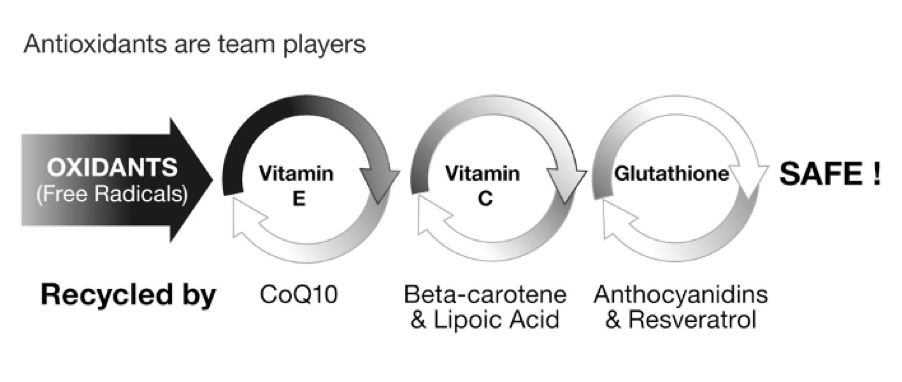
I’m proposing that there are four main biological drivers of our demise which I’m calling the four horsemen of the mental health apocalypse: a lack of brain fats, messed up methylation, loss of glucose control and excessive oxidation.
The first two – brain fats and methylation – are vital for the integral structure of neuronal membranes. The second two are vital for the function of brain cells, supplying fuel and coping with the oxidant ‘exhaust fumes’ of energy metabolism.
—
Brain fats in short supply
The dry weight of the brain is 60 per cent fat, and omega-3 DHA makes up the majority of the structural fat of neurons, followed closely by Arachidonic Acid (AA), an omega-6 fat. ALL BRAINS OF ALL ANIMALS contain predominantly these two essential brain fats. It is the available supply of these that determine whether an animal ends up with a big or small brain. The link between omega-3 DHA and brain function is beyond doubt, with study after study confirming the scientific evidence. Only last month, a study from the UK BioBank reported a 30 per cent lower risk of dementia in those with a higher omega-3 status in their blood (4). This confirmed the results of a US study (5) that found a 49 per cent reduced risk for dementia in those with the highest DHA level (top fifth) in their red blood cells versus the lowest (bottom fifth). A meta-analysis of 48 studies in the American Journal of Clinical Nutrition in 2023 (6) concludes that ‘a moderate-to-high level of evidence suggested that dietary intake of omega-3 fatty acids could lower risk of all-cause dementia or cognitive decline by about 20 per cent, especially for docosahexaenoic acid (DHA) intake’. Each 100mg increment of DHA was associated with an 8–10 per cent lower risk of dementia. And a 2023 study, by psychologists at the Linda Loma University in California and published in the journal Brain Sciences (7), reported that the higher a person’s omega-3 blood index was, the more white matter there was in their brain, and the better they performed on cognitive tests that predict less risk for dementia.
It’s compelling science. That is why my first recommendation is to always test your omega-3 index.
This is the percentage of omega-3 DHA and EPA in the membrane of red blood cells, and it is a direct reflector of the membrane levels in your brain. Red cells last for three months so this is a long-term measure of your omega-3 status. In countries such as Japan, known for a high fish diet, the omega-3 index is around 10 per cent on average. Ideally, a level of above 8 per cent is optimal. I thought I was doing well, supplementing daily 575mg of EPA and DHA combined, plus eating oily fish three times a week but I scored just under – 7.7 per cent. I’ve since upped my intake of DHA by 500 mg, to 750 mg total daily intake.
In its pure form, DHA isn’t enough, it has to become ‘phosphorylated’ to work. It’s a bit like using those glues where you have two tubes and have to mix a squeeze of one with the other for the glue to work. The ‘mixer’ in this case is the B vitamins in your body attaching the DHA to the phospholipids such as phosphatidylcholine (PC). If you have no phospholipids, or no DHA or B vitamins, the mix is not going to work. While the body can synthesise DHA, to reach the levels we need requires good quality food sources such as seafood, by far the richest source of (already) phosphorylated DHA. If fish isn’t your thing, supplementing with lecithin (granules or capsules) is a must – aim for two 1200mg capsules or 250mg of PC per day.
—
Vitamin D is a mental health essential
The other essential brain fat, which is actually a hormone, is vitamin D.
A large-scale study earlier this year, involving over twelve thousand dementia-free 70+ year olds (8), found that more than a third (37 per cent) took supplements of vitamin D and those that did had a 40 per cent lower incidence of dementia. Many nutrition professionals recommend supplementing around 3,000 iu in the winter to achieve an adequate blood level of 75 nmol/L or more, advice that is backed up by a consortium of some 35 vitamin D researchers.(9) The UK Government also recommends supplementing vitamin D, although the recommended 400iu falls far short of the amount needed for brain health. In a study in France, those with low vitamin D levels, below 50 nmol/L, had a nearly three-fold increased risk of Alzheimer’s (10) and worryingly, over sixty per cent of people in the UK have lower levels than this (11), while half are unaware of the need to supplement in the winter and only one in ten actually do (12). (Back in 2010, I was reported to the Advertising Standards Agency for suggesting that people had to supplement vitamin D in the winter because diet alone was not sufficient – how times change!)
Research continues to investigate whether having a higher blood level of vitamin D, perhaps 100 nmol/L, is even better for brain health. If you know your vitamin D level, you can help with this research by completing the Cognitive Function Test, and providing your vitamin D level. Or you can join our MIND project which includes a home test kit to measure your vitamin D level. We’ve tested 410,000 people’s cognitive function so far but need more people who know, or are willing to test their vitamin D.
Methylation and homocysteine-lowering B vitamins
Omega-3 DHA can only become active by the process of methylation, which attaches the DHA to a phospholipid and thereby enables it to be incorporated into the neuronal membrane. The process of methylation is totally dependent on vitamins B6, B12 and folate. Our methylation-ability is beautifully defined by our homocysteine level. Homocysteine rises if the biochemical pathway between the amino acid methionine converting to the methyl-donor SAMe is blocked. Without adequate vitamin B6, B12, folate or, in the liver, zinc and tri-methyl glycine (TMG), homocysteine will rise.
Lowering homocysteine with B vitamins is the greatest evidenced disease-modifying treatment, as shown in the best meta-analysis of 396 trials (13) by China’s leading Alzheimer’s prevention expert, Professor Jin-Tai Yu, whom we are honoured to have in our Scientific Advisory Board. It was also rated so by the US National Institutes of Health researchers (14).

Homocysteine is also a biomarker for over 100 diseases including almost all mental and neurological diseases. The seminal paper by Professors David Smith and Helga Refsum on the subject is vital for all to read. For example, just one recent meta-analysis showed that both homocysteine, vitamin B12, and folic acid predict the onset and development of Parkinson’s. Homocysteine levels above 11µmol/L are a clear indicator that the brain is shrinking. Professor David Smith, another member of our Scientific Advisory Board, recommends treatment with B vitamins for anyone with a homocysteine above 10µmol/L , giving 20 mg of B6, 400 mcg of methylfolate and 500µg of B12.
Increasingly, raised homocysteine is extremely common. In America, 40 per cent of those over 60 have a homocysteine of over 11 (15). In China ‘the mean (average) homocysteine levels in adult males less than 30 years of age and greater than 60 years were higher than the upper limit of normal (15 µmol/L).’ And in the UK, two in five adults over 61 have insufficient B12 to prevent accelerated brain shrinkage (16).
Homocysteine not only predicts Alzheimer’s dementias but also vascular dementia which, combined, make up almost 90 per cent of all dementias. Raised homocysteine is a major driver of cardiovascular and cerebrovascular disease. Raised homocysteine increases the risk of cerebrovascular disease by seventeen times (17)! Joe Rogan dedicated his recent show to exactly this (18) and stressed why testing homocysteine is vital for anyone with any form of cardiovascular, neurological or mental health disease.
The trouble with homocysteine is you just don’t know if your level is raised without testing it, which is why we have create our own at-home, highly accurate test kit. While up to 20 per cent of people have a methylation gene mutation (MTHFR677TT) making them more likely to have a raised level, it’s likely that most people with raised homocysteine are just not good at absorbing vitamin B12, a condition that becomes more common with age. This is why antacid proton pump inhibitor (PPI) drugs are such bad news. They drive down B12 and four years use cranks up Alzheimer’s risk by over 33 per cent (19).
Breakthrough in homocysteine testing
It is essential to test homocysteine level for anyone over 50 and anyone with any brain or mental health or cardiovascular disorder including hypertension. Treatment with B vitamins is also essential if the level is above 10µmol/L. While a homocysteine level above 11 means increased brain shrinkage, research shows that even a homocysteine level of above 9 during pregnancy predicts more problems, specifically withdrawn behaviour, anxiety/depression, social problems and aggressive behaviour in the child by the age of six (20). Raised homocysteine is a well known predictor of miscarriage and pregnancy problems, which is why I recommend that women can best prepare for a healthy pregnancy by ensuring their homocysteine level is below 7.5 mcmol/l. Above this, the evidence points to chromosomal damage (21).
All these studies refer to plasma homocysteine, that is the level found in the clear serum part of blood (rather than the red blood cells). The difficulty with many test kits is the need to separate or spin the blood shortly after taking the sample or pass the blood through a plasma separator. Many fall short of the correlation with serum/plasma homocysteine, the gold standard of testing. Excitingly, a breakthrough with both the fixing of blood (taken using a dry blood spot) and the testing process now means that we now have an accurate and inexpensive way to test homocysteine with our home test kit. This is going to be made available all over the world, starting with the UK and EU in January 2024. The validation of this test is extremely good, with no false positives or negatives. Accuracy can be further improved if the test is taken after fasting for 12 hours with water only. Both coffee and alcohol affect homocysteine levels, as does eating a protein-rich meal.
Please, join our Citizen Science research by both testing homocysteine and completing the Cognitive Function Test here

A consensus of world experts (22) has concluded that lowering homocysteine with B vitamins is the easiest and most cost-effective prevention action, which Oxford University’s health economists estimate would save the UK £66 million per year (23).
However, it’s vital to test both homocysteine and Omega-3 levels, as they are co-dependent. Homocysteine-lowering B vitamins only work in those with sufficient omega-3, and omega-3 only works if homocysteine is low. This short film shows how this works here.
It explains why studies giving omega-3 or giving B vitamins have not consistently been effective. However, in re-analyses of three studies, B vitamins are highly effective, both in reducing the rate of brain shrinkage and improving cognition, in those with sufficient omega-3, and conversely, omega-3 is highly effective, but only in those with homocysteine below 11 mcmol/L (24).
Want to learn more about homocysteine and how to reclaim your brain? Join us for the Homocysteine Unplugged webinar.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
2 van Os J, Guloksuz S. Population Salutogenesis—The Future of Psychiatry? JAMA Psychiatry. Published online December 20, 2023. doi:10.1001/jamapsychiatry.2023.4582
3 Crawford M, Marsh, D ‘The Shrinking Brain’ 2023
4 Sala-Vila, A.; Tintle, N.; Westra, J.; Harris, W.S. Plasma Omega-3 Fatty Acids and Risk for Incident Dementia in the UK Biobank Study: A Closer Look. Nutrients 2023, 15,4896. https://doi.org/10.3390/ nu15234896
5 Sala-Vila, A.; Satizabal, C.L.; Tintle, N.; Melo van Lent, D.; Vasan, R.S.; Beiser, A.S.; Seshadri, S.; Harris, W.S. Red Blood Cell DHA Is Inversely Associated with Risk of Incident Alzheimer’s Disease and All-Cause Dementia: Framingham Offspring Study. Nutrients 2022, 14, 2408. https://doi.org/10.3390/ nu14122408
6 Wei BZ, Li L, Dong CW, Tan CC; Alzheimer’s Disease Neuroimaging Initiative; Xu W. The Relationship of Omega-3 Fatty Acids with Dementia and Cognitive Decline: Evidence from Prospective Cohort Studies of Supplementation, Dietary Intake, and Blood Markers. Am J Clin Nutr. 2023
7 Loong, S.; Barnes, S.; Gatto, N.M.; Chowdhury, S.; Lee, G.J. Omega-3 Fatty Acids, Cognition, and Brain Volume in Older Adults. Brain Sci.2023,13,1278. https://doi.org/ 10.3390/brainsci13091278
8 Ghahremani M et al. Vitamin D supplementation and incident dementia: Effects of sex, APOE, and baseline cognitive status. Alzheimers Dement (Amst). 2023 Mar 1;15(1):e12404. doi: 10.1002/dad2.12404. PMID: 36874594; PMCID: PMC9976297.
9 Płudowski P et al Guidelines for Preventing and Treating Vitamin D Deficiency: A 2023 Update in Poland. Nutrients. 2023 Jan 30;15(3):695. doi: 10.3390/nu15030695. PMID: 36771403; PMCID: PMC9920487.
10 Jia J et al. Effects of vitamin D supplementation on cognitive function and blood Aβ-related biomarkers in older adults with Alzheimer’s disease: a randomised, double-blind, placebo-controlled trial. J Neurol Neurosurg Psychiatry. 2019 Dec;90(12):1347-1352. doi: 10.1136/jnnp-2018-320199. Epub 2019 Jul 11. PMID: 31296588.
11 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7353432/pdf/nutrients-12-01868.pdf
12 https://www.nutrition.org.uk/news/2021/british-nutrition-foundation-survey-reveals-49-adults-unaware-of-uk-government-guidelines-for-vitamin-d/
13 Yu JT, Xu W, Tan CC, Andrieu S, Suckling J, Evangelou E, Pan A, Zhang C, Jia J, Feng L, Kua EH, Wang YJ, Wang HF, Tan MS, Li JQ, Hou XH, Wan Y, Tan L, Mok V, Tan L, Dong Q, Touchon J, Gauthier S, Aisen PS, Vellas B. Evidence-based prevention of Alzheimer’s disease: systematic review and meta-analysis of 243 observational prospective studies and 153 randomised controlled trials. J Neurol Neurosurg Psychiatry. 2020 Nov;91(11):1201-1209. doi: 10.1136/jnnp-2019-321913. Epub 2020 Jul 20. PMID: 32690803; PMCID: PMC7569385.
14 Beydoun MA, Beydoun HA, Gamaldo AA, Teel A, Zonderman AB, Wang Y. Epidemiologic studies of modifiable factors associated with cognition and dementia: systematic review and meta-analysis. BMC Public Health. 2014 Jun 24;14:643. doi: 10.1186/1471-2458-14-643. PMID: 24962204; PMCID: PMC4099157.
15 Pfeiffer C, Clin Chem. 2008; R. Xu, Nature Scientific Reports 2022; Vogiatzlou A, Neurology, 2008
16 Vogiatzoglou A, Refsum H, Johnston C, Smith SM, Bradley KM, de Jager C, Budge MM, Smith AD. Vitamin B12 status and rate of brain volume loss in community-dwelling elderly. Neurology. 2008 Sep 9;71(11):826-32. doi: 10.1212/01.wnl.0000325581.26991.f2. PMID: 18779510.
17 Teng Z, Feng J, Liu R, Ji Y, Xu J, Jiang X, Chen H, Dong Y, Meng N, Xiao Y, Xie X, Lv P. Cerebral small vessel disease mediates the association between homocysteine and cognitive function. Front Aging Neurosci. 2022 Jul 15;14:868777. doi: 10.3389/fnagi.2022.868777. PMID: 35912072; PMCID: PMC9335204.
18 See the Joe Rogan show https://www.youtube.com/watch?v=-oqYoNwnOs0.
19 Northuis CA, Bell EJ, Lutsey PL, George KM, Gottesman RF, Mosley TH, Whitsel EA, Lakshminarayan K. Cumulative Use of Proton Pump Inhibitors and Risk of Dementia: The Atherosclerosis Risk in Communities Study. Neurology. 2023 Oct 31;101(18):e1771-e1778. doi: 10.1212/WNL.0000000000207747. Epub 2023 Aug 9. PMID: 37558503; PMCID: PMC10634644.
20 Roigé-Castellví J, Murphy M, Fernández-Ballart J, Canals J. Moderately elevated preconception fasting plasma total homocysteine is a risk factor for psychological problems in childhood. Public Health Nutr. 2019 Jun;22(9):1615-1623. doi: 10.1017/S1368980018003610. Epub 2019 Jan 14. PMID: 30636652; PMCID: PMC10261079.
21 Fenech M, Aitken C, Rinaldi J. Folate, vitamin B12, homocysteine status and DNA damage in young Australian adults. Carcinogenesis. 1998 Jul;19(7):1163-71. doi: 10.1093/carcin/19.7.1163. PMID: 9683174.
22 Smith AD, Refsum H, Bottiglieri T, Fenech M, Hooshmand B, McCaddon A, Miller JW, Rosenberg IH, Obeid R. Homocysteine and Dementia: An International Consensus Statement. J Alzheimers Dis. 2018;62(2):561-570. doi: 10.3233/JAD-171042. PMID: 29480200; PMCID: PMC5836397.
23 Tsiachristas A, Smith AD. B-vitamins are potentially a cost-effective population health strategy to tackle dementia: Too good to be true? Alzheimers Dement (N Y). 2016 Aug 11;2(3):156-161. doi: 10.1016/j.trci.2016.07.002. PMID: 29067302; PMCID: PMC5651357.
24 Jernerén F, Elshorbagy AK, Oulhaj A, Smith SM, Refsum H, Smith AD (2015). Brain atrophy in cognitively impaired elderly: the importance of long-chain ω-3 fatty acids and B vitamin status in a randomized controlled trial. Am J Clin Nutr. 2015 Jul;102(1):215-21; see also van Soest, A.P.M., van de Rest, O., Witkamp, R.F. et al. DHA status influences effects of B-vitamin supplementation on cognitive ageing: a post-hoc analysis of the B-proof trial. Eur J Nutr 61, 3731–3739 (2022). https://doi.org/10.1007/s00394-022-02924-w; see also Jernerén F, Cederholm T, Refsum H, Smith AD, Turner C, Palmblad J, Eriksdotter M, Hjorth E, Faxen-Irving G, Wahlund LO, Schultzberg M, Basun H, Freund-Levi Y. Homocysteine Status Modifies the Treatment Effect of Omega-3 Fatty Acids on Cognition in a Randomized Clinical Trial in Mild to Moderate Alzheimer’s Disease: The OmegAD Study. J Alzheimers Dis. 2019;69(1):189-197. doi: 10.3233/JAD-181148. PMID: 30958356.
25 Lakhan, S.E., Kirchgessner, A. The emerging role of dietary fructose in obesity and cognitive decline. Nutr J 12, 114 (2013).