The Shrinking Brain. Are we dumbing down?
—
Both brain size and IQ are falling in modern humans, coinciding with a big increase in mental illness.
What we eat is to blame, says Professor Michael Crawford, author of a new book ‘The Shrinking Brain’ and Sir David Attenborough is convinced he is right.
The Falling IQ
IQ scores have also been steadily falling for the past few decades. Norwegian researchers, headed by Ole Rogeberg, a senior research fellow at the Ragnar Frisch Center for Economic Research in Norway, analysed the IQ scores of Norwegian men born between 1962 and 1991 and found that scores steadily decreased among those born after 1975 (1). “Similar studies in Denmark, Britain, France, the Netherlands, Finland and Estonia have demonstrated a similar downward trend in IQ scores” says Rogeberg. “The decline is due to environmental factors,”
This coincides with a change in Western diet away from fat, towards carbohydrates and sugar, based on the mistaken belief that it was fat, not sugar, that was causing heart disease and that we should all eat a low-fat diet. Since then, our IQ scores have been dropping by about 7 per cent per generation.
“We are heading for an idiocracy” says Professor Crawford who is Director of the Institute of Brain Chemistry and Human Nutrition. Currently one in five of the world’s children and adolescents have a mental health condition (2).’ If this trend continues, by 2080 he predicts that more than a third of the world’s population will have a mental disability.
The World Health Organisation report says ‘there has been a 13% rise in mental health conditions. One in eight now suffers from mental illness. The incidence of depression is through the roof. Last year in the UK there were over 100 million prescriptions for antidepressants.
Crawford is convinced it is the modern-day diet that is causing us to dumb down. “Our genome is adapted to eating the wild foods we ate during our species’ evolution. Today’s diet bears no resemblance to this.”
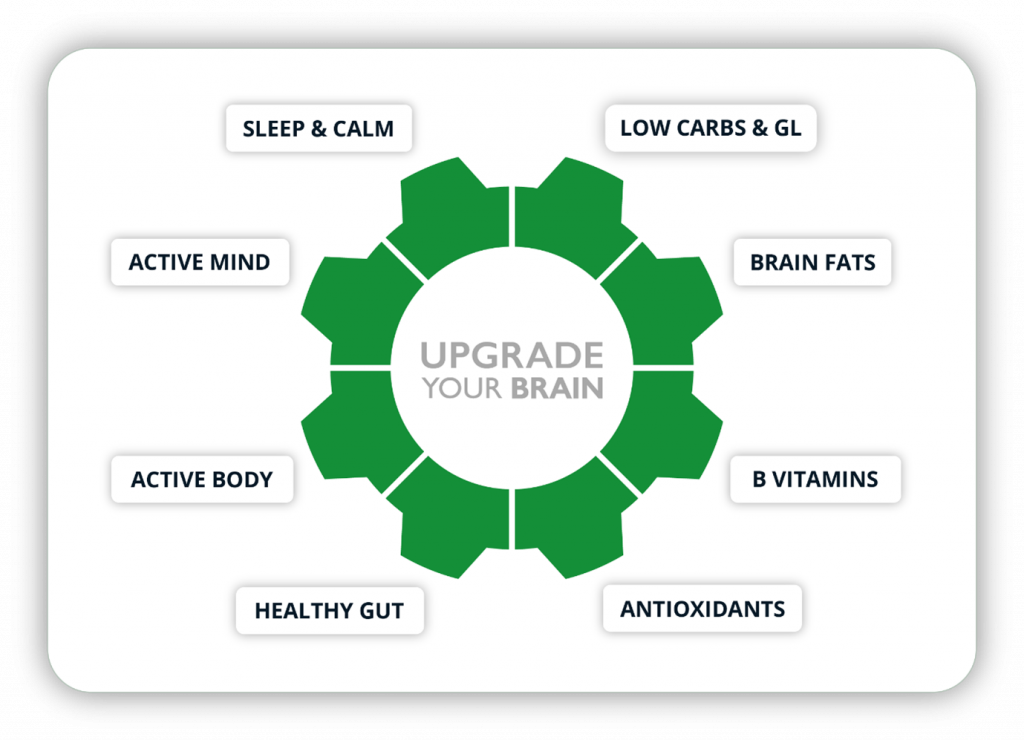
Key nutrients from land & sea
In his book, The Shrinking Brain, he says “Our ancestors evolved a unique 1,600cc brain evolving from our ancestral 350cc brain of the chimpanzee, despite our genome only differing by 1.5% (3). This could only have happened by providing brain-specific building nutrients from land and sea. There is incontrovertible evidence of early Homo sapiens exploiting the marine food web in coastal Africa.” In other words, we were the waterside ape who became smart, with bigger brains, by eating mussels, oysters, crabs and fish.
Professor Crawford discovered, in 1971, that the brains of all mammals are rich in omega-3 DHA. Their brain size varied according to their dietary supply of DHA found in seafood. A dolphin, for example, has a 1,700cc brain, slightly larger than ours, while a lion has a 320cc brain about that of a chimpanzee. “The mix of wildland and aquatic foods powered by the encephalization of the brain from the 340cc of the chimp to the 1,500-1,700 of cro-magnon. DHA is not only involved in signalling but it stimulates gene expression in the brain so the rich aquatic food sources constantly, every day, would have powered the increase in brain size and function.” says Crawford.

“Today’s diet contains less than a tenth of the omega-3 fats that our ancestors ate and this is having dire consequences on mental health. Increased rates of depression, autism, ADHD and dementia are all strongly linked to lack of seafood. Increased intake from eating fish or supplementing omega-3 fish oils reduces dementia risk by 20 per cent (4). While a plant-based diet has many benefits, those who eat no fish, are especially vulnerable and must supplement omega-3 DHA, derived from algae. The only way to be sure you have enough is to get a blood test to specifically test your levels.” Says our CEO and founder Patrick Holford.
This is why we have just launched a simple ‘do it at home’ pin-prick test that can give you a clear indication of your Omega-3 levels, which done alongside our Cognitive Function Test, can help identify what’s driving future risk and show you how to dementia-proof your diet and lifestyle.
Canadian neuroscientist and brain expert Professor Stephen Cunnane at the University of Sherbrook in Canada agrees “A shore-based diet, i.e., fish, molluscs, crustaceans, frogs, bird’s eggs and aquatic plants, provides the richest known dietary sources of brain selective nutrients.” says Cunnane. “Change in diet away from marine foods is the likely explanation for this decrease in brain size.”
Sir David Attenborough, a supporter of the waterside ape theory, agrees “Gathering molluscs is far easier than chasing elephants and wildebeests across the savannah.”
Children & omega-3
Today, under 5 per cent of children achieve the basic requirement for omega-3 from seafood (5).
Professor Michael Crawford, who is a visiting professor at Imperial College’s Chelsea & Westminster campus and on our Scientific Advisory Board, was part of the team that has recently established that, if a pregnant woman lacks omega-3 DHA she produces a substitute fat, oleic acid, to fill the baby’s brain. But it doesn’t work. Levels of oleic acid in a pregnant woman’s blood predicted preterm birth which carries the highest risk of developmental brain problems and mental deficits in their offspring, as well as a risk of learning and cognitive disabilities. Low omega-3 and B vitamins in mothers increase risk for lower IQ, learning and emotional problems in children (6).
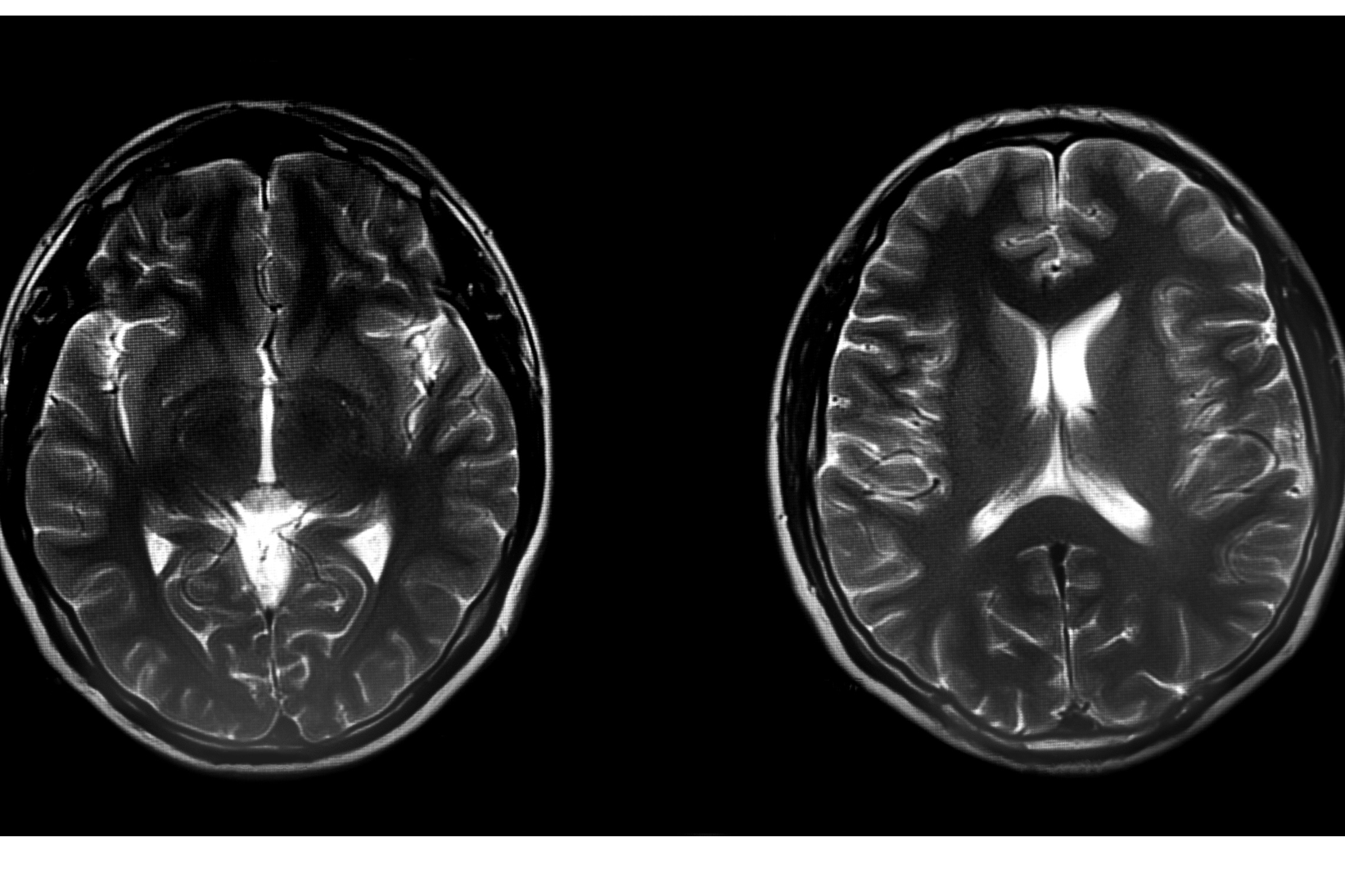
A new study shows that the higher the omega-3 index and DHA, the greater both the brain size and the cognition of older people (7). Brain size predicts cognitive abilities, which is why we have started offering these vital tests – which are both easy and affordable to do at home.
Brain size is worked out from skull capacity. Homo sapiens skulls dating back to 29,000 years ago had a brain capacity of 1,660cc. By 10,000 years ago it was around 1,500cc or 1.5 kilograms. The average brain size today is a fifth smaller, at 1,336cc. Brain size may have started to shrink from 10,000 years ago, coinciding with mankind developing more land-based agriculture and eating less marine food along rivers and coasts.
So we are inviting you to join our ‘citizen science’ study to track the impact of diet and Omega-3 on cognitive function over time.
Our brains and mental health are suffering as a result of our dietary changes.
So if you are concerned about your levels of Omega-3 and how it might be impacting your brain, body and life – you can now test your levels with our Omega-3 hometest kit here, which is offered alongside the free Cognitive Function Test, which assesses how well your diet is supporting your brain health.
Thank you for reading!
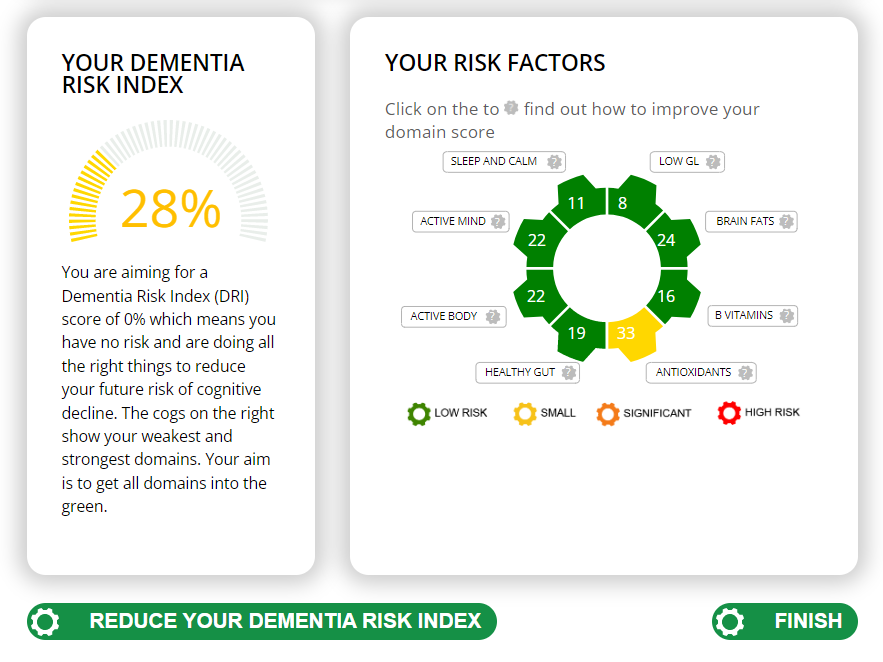
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
Supporting Research
IQ FALLING
Bratsberg B, Rogeberg O. Flynn effect and its reversal are both environmentally caused. Proc Natl Acad Sci U S A. 2018 Jun 26;115(26):6674-6678. doi: 10.1073/pnas.1718793115. Epub 2018 Jun 11. PMID: 29891660; PMCID: PMC6042097.
DECREASE IN BRAIN SIZE
Cunnane SC, Crawford MA. Energetic and nutritional constraints on infant brain development: implications for brain expansion during human evolution. J Hum Evol. 2014 Dec;77:88-98. doi: 10.1016/j.jhevol.2014.05.001. Epub 2014 Jun 11. PMID: 24928072.
MENTAL HEALTH RISING
OMEGA-3 PREDICTS COGNITIVE PROBLEMS IN CHILDREN
Montgomery P, Burton JR, Sewell RP, Spreckelsen TF, Richardson AJ. Low blood long chain omega-3 fatty acids in UK children are associated with poor cognitive performance and behavior: a cross-sectional analysis from the DOLAB study. PLoS One. 2013 Jun 24;8(6):e66697. doi: 10.1371/journal.pone.0066697.
OMEGA-3 PREDICTS RISK FOR DEMENTIA AND COGNITIVE DECLINE
Wei BZ, Li L, Dong CW, Tan CC; Alzheimer’s Disease Neuroimaging Initiative; Xu W. The Relationship of Omega-3 Fatty Acids with Dementia and Cognitive Decline: Evidence from Prospective Cohort Studies of Supplementation, Dietary Intake, and Blood Markers. Am J Clin Nutr. 2023 Jun;117(6):1096-1109. doi: 10.1016/j.ajcnut.2023.04.001. Epub 2023 Apr 5. PMID: 37028557; PMCID: PMC10447496.
OMEGA-3 LEVELS PREDICT BRAIN SIZE IN OLDER PEOPLE
Loong, S.; Barnes, S.; Gatto, N.M.; Chowdhury, S.; Lee, G.J. Omega-3 Fatty Acids, Cognition, and Brain Volume in Older Adults. Brain Sci.2023,13,1278. https://doi.org/ 10.3390/brainsci13091278
References
1 Bratsberg B, Rogeberg O. Flynn effect and its reversal are both environmentally caused. Proc Natl Acad Sci U S A. 2018 Jun 26;115(26):6674-6678. doi: 10.1073/pnas.1718793115. Epub 2018 Jun 11. PMID: 29891660; PMCID: PMC6042097.
3 Cunnane SC, Crawford MA. Energetic and nutritional constraints on infant brain development: implications for brain expansion during human evolution. J Hum Evol. 2014 Dec;77:88-98. doi: 10.1016/j.jhevol.2014.05.001. Epub 2014 Jun 11. PMID: 24928072.
4 Wei BZ, Li L, Dong CW, Tan CC; Alzheimer’s Disease Neuroimaging Initiative; Xu W. The Relationship of Omega-3 Fatty Acids with Dementia and Cognitive Decline: Evidence from Prospective Cohort Studies of Supplementation, Dietary Intake, and Blood Markers. Am J Clin Nutr. 2023 Jun;117(6):1096-1109. doi: 10.1016/j.ajcnut.2023.04.001. Epub 2023 Apr 5. PMID: 37028557; PMCID: PMC10447496.
5 Kranz, S.; Jones, N.R.V.; Monsivais, P. Intake Levels of Fish in the UK Paediatric Population. Nutrients 2017, 9, 392. https://doi.org/10.3390/nu9040392
6 Montgomery P, Burton JR, Sewell RP, Spreckelsen TF, Richardson AJ. Low blood long chain omega-3 fatty acids in UK children are associated with poor cognitive performance and behavior: a cross-sectional analysis from the DOLAB study. PLoS One. 2013 Jun 24;8(6):e66697. doi: 10.1371/journal.pone.0066697. Erratum in: PLoS One. 2013;8(9); see also Veena SR, Krishnaveni GV, Srinivasan K, Wills AK, Muthayya S, Kurpad AV, Yajnik CS, Fall CH. Higher maternal plasma folate but not vitamin B-12 concentrations during pregnancy are associated with better cognitive function scores in 9- to 10- year-old children in South India. J Nutr. 2010 May;140(5):1014-22. doi: 10.3945/jn.109.118075. Epub 2010 Mar 24. PMID: 20335637; PMCID: PMC3672847; see also McNulty H, Rollins M, Cassidy T, Caffrey A, Marshall B, Dornan J, McLaughlin M, McNulty BA, Ward M, Strain JJ, Molloy AM, Lees-Murdock DJ, Walsh CP, Pentieva K. Effect of continued folic acid supplementation beyond the first trimester of pregnancy on cognitive performance in the child: a follow-up study from a randomized controlled trial (FASSTT Offspring Trial). BMC Med. 2019 Oct 31;17(1):196. doi: 10.1186/s12916-019-1432-4. PMID: 31672132; PMCID: PMC6823954.
7 Loong, S.; Barnes, S.; Gatto, N.M.; Chowdhury, S.; Lee, G.J. Omega-3 Fatty Acids, Cognition, and Brain Volume in Older Adults. Brain Sci.2023,13,1278. https://doi.org/ 10.3390/brainsci13091278