What’s driving Alzheimer’s and vascular dementia?
By Patrick Holford
How does cognitive decline happen?
One theory was that it was to do with the accumulation of amyloid protein, producing amyloid plaque that interferes with brain cell communication. But, despite over 30 clinical trials, lowering amyloid protein has had close to zero clinical effect. But, even if this was part of the problem, one would have to ask why?
There are plenty of left-field theories. One, for example, is that it’s an auto-immune disease whereby the brain starts to destroy itself. There are plenty of diet and lifestyle diseases that tip over into auto-immune diseases. For example, type-2 diabetes can convert to type-1 diabetes and osteoarthritis can convert to rheumatoid arthritis. But even so, one would have to ask why? What would be driving this?
Risk Factors for Alzheimer’s – what do they have in common?
There are over 20 known risk factors that predict future risk for cognitive decline, dementia and/or Alzheimer’s. These include:
- Anon-adherence to Mediterranean diet principles
- Cardiovascular disease, and high blood pressure
- Depression/social isolation/loneliness
- Diabetes
- Genes (such as senilin) and predisposing genes (eg ApoE4)
- Head trauma
- High blood homocysteine (a measure of B vitamins)
- Insulin resistance
- Lack of antioxidants/polyphenols in plant foods
- Lack of cognitive stimulation
- Lack of exercise and muscle mass – frailty
- Lack of folate, B12 and B6
- Lack of sleep
- Low education level
- Low phospholipid and choline intake (in eggs and fish)
- Low seafood consumption and a lack of omega-3
- Low sunlight exposure
- Low vitamin C, D and E intake
- Low zinc levels
- Medication – antiacids, metformin, diuretics
- Metabolic syndrome
- Poor gut health and dental health
- Poor hearing
- Smoking
- Stress
- Strokes and TIAs (transient ischemic attacks )
- Too much sugar, refined, processed, carb-rich foods
So far researchers have looked at individual known risk factors for Alzheimer’s, then tried to change them with some success. The nutritionists have tried to change diet, or give supplements. The pharmacologists have tried to give drugs to lower, for example, high blood pressure or insulin levels. The psychologists have tried to increase cognitive stimulation and address depression and isolation, and insomnia. The sports physiologists have tried to increase exercise. But what do all these factors have in common? Is there a way of looking that ties all these risk factors together into an understanding as to what is actually driving dementia?
The old, but still dominant mindset in science is ‘reductionism’. The idea is to look at one thing, or one risk factor, then change it in a randomised placebo-controlled trial. The idea is that if everyone does this then you could pool all the interventions together to produce a cure. This reminds me of a comment made in the G8 summit on dementia in 2010, in London, when we succeeded in getting a discussion on dementia prevention added to the agenda. The pharma representative said words to the effect of ‘we will solve dementia with multiple drugs, just like we solved AIDS’. The reality is studies giving drugs[1] to lower blood sugar for diabetics, lower blood pressure with anti-hypertensive drugs, lower cholesterol with statins, even lower amyloid protein, have failed. The official cost of all this research is $42.5 billion to date.[2] This is five times more than the cost of the James Webb telescope. This approach clearly isn’t working. The only ‘drugs’ that have worked are homocysteine lowering B vitamins and omega-3 fish oils – and the recent discovery is that they work together, in cooperation.
There’s a new emerging way of doing science which is called ‘systems-based’ science. The physicist, Fritjof Capra, has explained this way of doing science in his book ‘The Web of Life’. He says “Systems thinking emerged from a series of interdisciplinary dialogues among biologists, psychologists, and ecologists, in the 1920s and ’30s. In all these fields, scientists realized that a living system—organism, ecosystem, or social system—is an integrated whole whose properties cannot be reduced to those of smaller parts. The “systemic” properties are properties of the whole, which none of its parts have. So, systems thinking involves a shift of perspective from the parts to the whole. The early systems thinkers coined the phrase, “The whole is more than the sum of its parts.”[3]
Us humans are a complex adaptive system. What’s also been learnt about complex adaptive systems is that they have a certain amount of ‘resilience’ which you can think of as the credit in your health deposit account. When that runs out, disease occurs. Many leaders in the field of nutritional and naturopathic medicine consider that many of the same underlying processes are going wrong in our bodies, which then cause the emergence of a ‘disease’ depending on the organ it strikes – so heart disease, diabetes, arthritis and dementia have similar contributing factors.
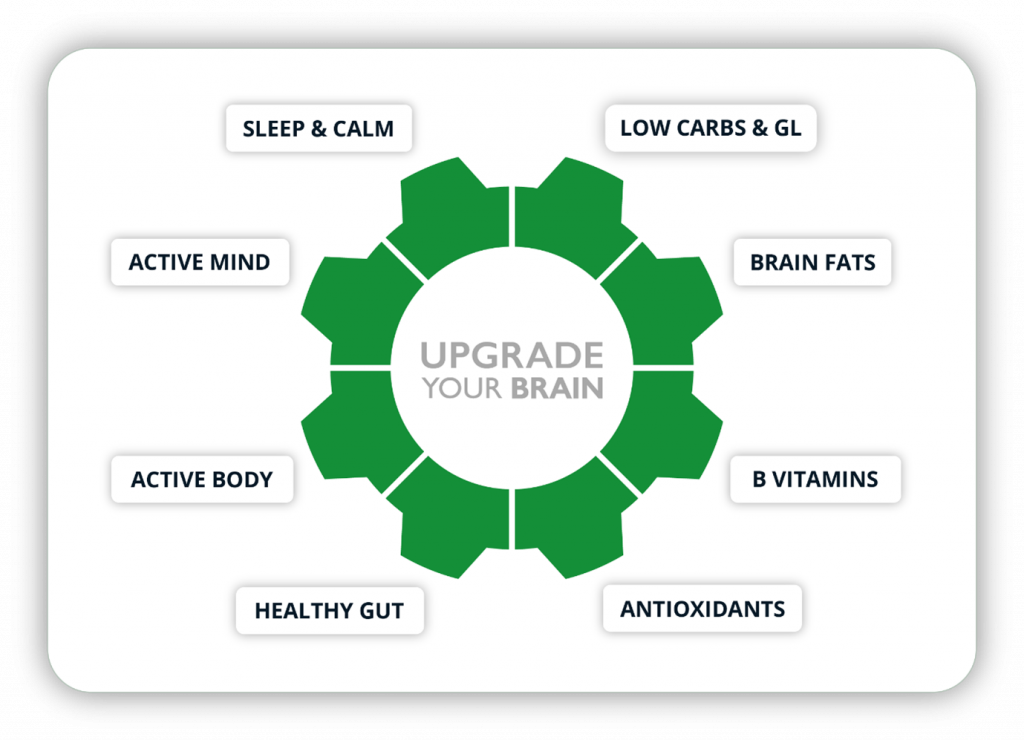
At Food for the Brain, we can organise all these risks above into eight domains shown below. It is certainly true that these eight domains of ‘risk’ cover much of what we know about the risks for heart disease, diabetes and arthritis, for example. This partly, but not fully. answers the question about what is actually driving dementia.
Another understanding within systems-based thinking is well illustrated by asking the question ‘what is the difference between an inanimate object, like a bicycle, and an animate organism, such as us?’ A bicycle has ‘parts’ and the parts related to each other, as in functioning together. So do we. But also, there is ‘life’ running through us. You can imagine your brain’s neural network lighting up, with ‘energy’ or signals shooting this way and that. If you have healthy parts, all functioning, but no signals, you’re kind of ‘switched off’.
We call the parts – structure; the relationship of the parts – function; and the life running through the neural network – utilisation. These are shown visually below in a way to illustrate that they are integral, with each dependent on the other.
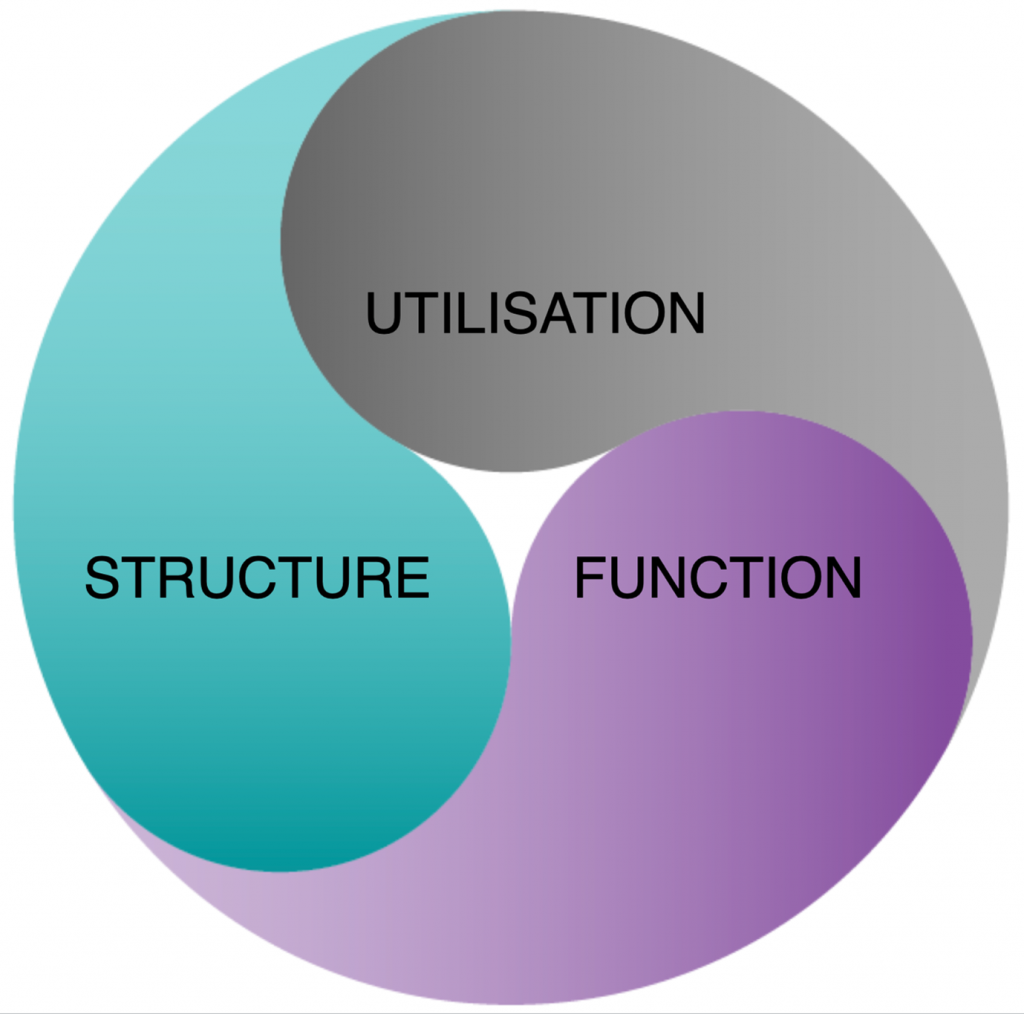
Now, let’s reorganise all those risk factors accordingly into whether they are primarily required for the structure or function of the neural network, or send messages across it.
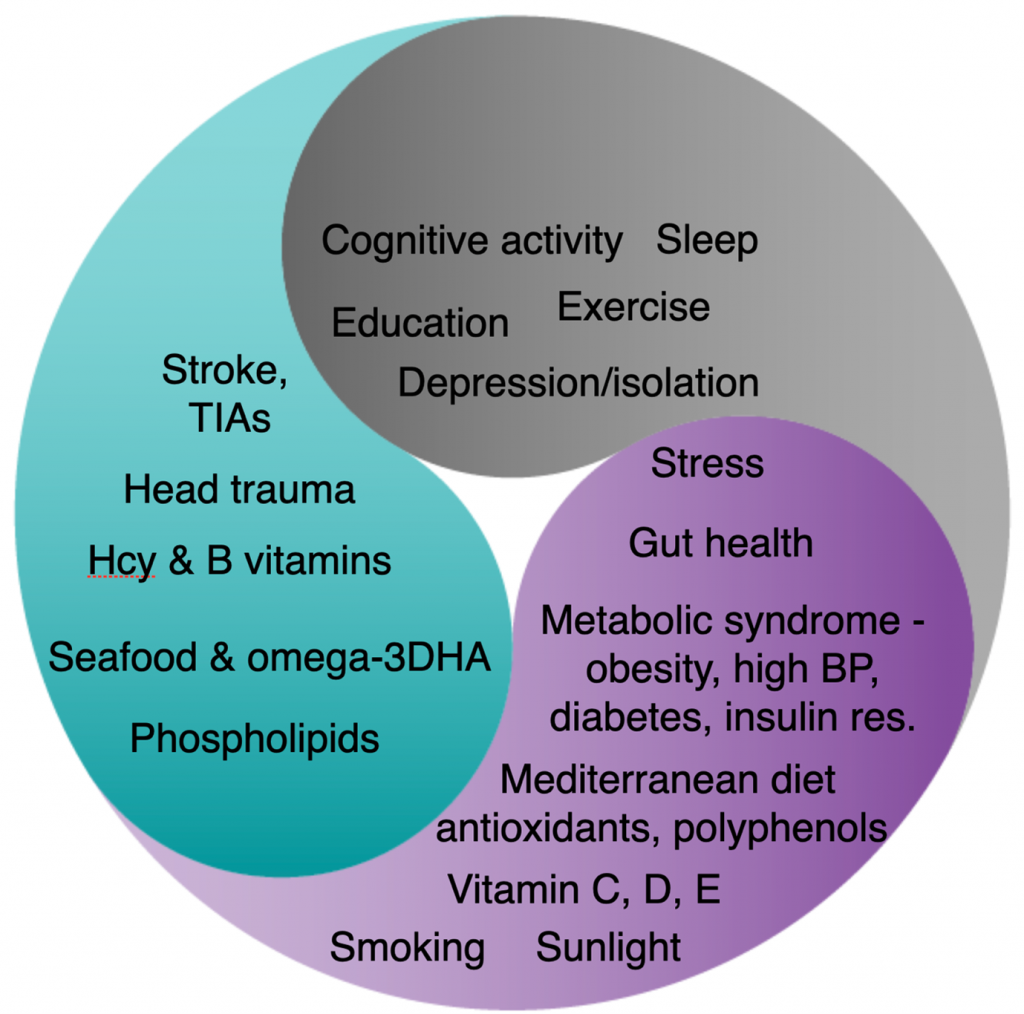
If you’ve watched the short animated film ‘how to keep building brain cells at any age‘ you’ll know that the membrane of every brain cell is made by binding omega-3 DHA, rich in seafood, to phospholipids and especially Phosphatidylcholine, rich in eggs and fish, to produce what called ‘phosphorylated DHA’. You need this to have a functioning brain. It actually makes up more than 90 per cent of the structure of your brain.
You’ll also know that the ‘binding’ of these two parts depends on B vitamins, which drive a process called methylation. So, without enough B vitamins your brain and nervous system fall apart. The best measure of methylation, and whether you are getting enough B vitamins, is your blood homocysteine level. If your homocysteine level is high, you’ve got a problem. Above 11mcmol/l and you’ve got a shrinking brain. More than half of all people over 70 have a homocysteine level above this. It should, therefore, be no surprise to find that, if you have a raised homocysteine level, and are given B vitamins, if you also have a low omega-3 DHA intake or blood level, the B vitamins won’t work. Conversely, if you supplement omega-3 fish oils, but have a raised homocysteine level or lack of B vitamins, the omega-3 won’t work. The full story of the dynamic duo of Omega-3 and B vitamins is explained here.
It is likely that choline deficiency, which is especially common in those who rarely eat fish or eggs, may also create a similar structural problem in the brain. In animals supplementing choline prevents Alzheimer’s related brain changes.[4]
Protecting the Function of Your Brain
There are many aspects of ‘function’ of the brain. Using a simple car analogy, one thinks of the need for fuel and the need for oil to lubricate the parts. The two main fuels of brain cells are either glucose, derived from carbs, or ketone derived from fat.
If you’ve watched the animated film ‘how to fuel your brain for better memory’, you’ll know about the need for slow-releasing carbs and ketones from a type of fat called a medium chain triglyceride (MCT) and specifically C8 oil.
Too much sugar, and especially fructose and high fructose corn syrup (now used by the food industry to sweeten foods), and too much refined carbohydrates interferes with fuel supply to brain cells by making you ‘insulin resistant’. Insulin receptors, embedded in neuronal membranes, transport glucose into brain cells. If these receptors, which are like doors, are largely shut down, the brain starves of clean fuel. Read professor Robert Lustig’s article “Is sugar killing your brain?’ for the full story.
The alternative brain fuel – ketones, which neurons actually prefer, can be made in the liver from a type of fat called C-8 (caprylic acid triglyceride) which makes up 7 per cent of coconut oil. In a study giving people with memory problems two tablespoons of C8 oil, their brains produced 230 per cent more energy from ketones and their memory improved. The article ‘Is fat the best brain fuel?’ gives you the full story.
The lubricating ‘oil’ in a car analogy would be both dealing with the ‘exhaust fumes’ of the brain’s energy production, namely oxidants. These are mopped up by antioxidants and polyphenols rich in plant foods. That where food such as blueberries and cacao, or vitamin C and E, come in. It’s also why smoking is such a big risk factor.
Another part of ‘function’ is circulation – anything that improves circulation helps the function. Many of the things we’ve mentioned – lowering homocysteine with B vitamins, omega-3, antioxidants, polyphenols – also help circulation.
Another part of ‘function’ is inflammation. Behind all those ‘metabolic’ diseases -diabetes, heart disease, arthritis to name a few – lies inflammation which doesn’t just affect the specific organ, be it heart of joint, but also the brain.
Use it or Loss it – Why Your Brain Needs Stimulation
One of our experts, Tommy Wood, assistant research professor at the University of Washington in Seattle, focussing on neuroscience, has developed an excellent model for understanding the ‘use it or lose it’ principle. He’s big into exercise.
‘Exercise is important because it makes the brain do things that keep it healthy, such as growth and repair and maintaining temperature and weight,’ he says. ‘When they aren’t stimulated, the health of brain tissues deteriorates with a knock-on effect on memory and thinking.’
And it’s not just physical exercise that does this, we also benefit from the mental exercise involved in likes of solving puzzles or learning a new language. ‘For many people the worst thing they can do for their brain is to retire’, says Wood. ‘They lose much of the stimulation that kept it healthy.’
Sleep as a brain protector also fits in here. It’s vital for recovering from both physical and intellectual exercise and to store and organise what you have learnt in the day.
‘But sleep and exercise aren’t enough on their own,’ Wood continues. ‘All that repair and maintenance needs a good supply of nutrients.’
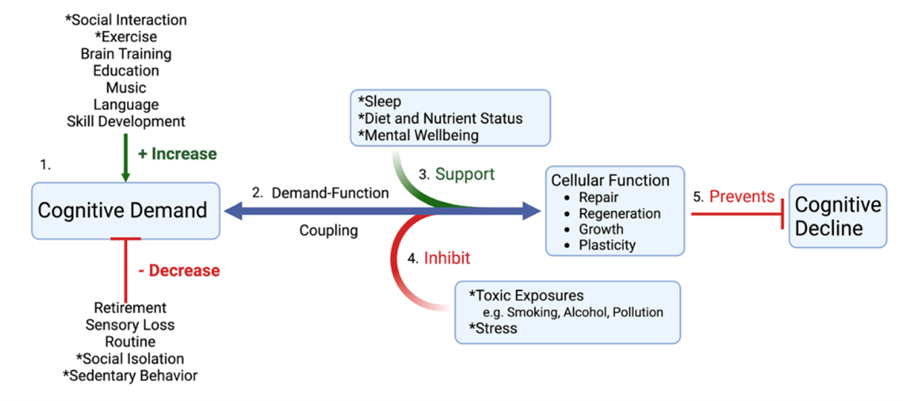
Stress also fits in here because stress, as well as environmental and dietary ‘pollution’ be it from drinking and smoking, dirty air, moulds, even allergens like gluten with can induce ‘brain fog’ often experienced by those with coeliac disease, promote inflammation and inhibit repair and regeneration.
A Unified Model for the Drivers of Cognitive Decline
This systems-based approach to what’s potentially driving cognitive decline makes it obvious that there will never be a single drug or single factor that stops a person developing dementia. Instead, if a person has enough ‘interference’ with the structure, function or utilisation of their brain then there will, inevitably be cognitive decline with age.
At Food for the Brain, when you complete your Cognitive Function Test, you know objectively how you are doing and how much room for improvement there is. Then you are invited to complete the Dementia Risk Index questionnaire, which not only gives you a score out of 100% (you are aiming for a score closer to 0%) but also shows you in which domain you have the most room for improvement.
You are then invited to join COGNITION, which is an interactive brain upgrade programme that targets your weakest areas and shows you the simplest changes that will make the biggest difference to reduce your risk.
The goal is to turn all your reds, oranges and yellows into green, then reassess your cognitive function. By joining you are becoming part of a group of hundreds of thousands of citizen health scientists helping to discover what really works to dementia-proof your diet and lifestyle.
Take the FREE Cognitive Function Test today.
References
[1] Peters R, Breitner J, James S, Jicha GA, Meyer PF, Richards M, Smith AD, Yassine HN, Abner E, Hainsworth AH, Kehoe PG, Beckett N, Weber C, Anderson C, Anstey KJ, Dodge HH. Dementia risk reduction: why haven’t the pharmacological risk reduction trials worked? An in-depth exploration of seven established risk factors. Alzheimers Dement (N Y). 2021 Dec 8;7(1):e12202. doi: 10.1002/trc2.12202. PMID: 34934803; PMCID: PMC8655351.
[2] Cummings JL, Goldman DP, Simmons-Stern NR, Ponton E. The costs of developing treatments for Alzheimer’s disease: A retrospective exploration. Alzheimers Dement. 2022 Mar;18(3):469-477. doi: 10.1002/alz.12450. Epub 2021 Sep 28. PMID: 34581499; PMCID: PMC8940715.
[3] Fritjof Capra (2009) The New Facts of Life: Connecting the Dots on Food, Health, and the Environment, Public Library Quarterly, 28:3, 242-248, DOI: 10.1080/01616840903110107
[4] Velazquez R, Ferreira E, Knowles S, Fux C, Rodin A, Winslow W, Oddo S. Lifelong choline supplementation ameliorates Alzheimer’s disease pathology and associated cognitive deficits by attenuating microglia activation. Aging Cell. 2019 Dec;18(6):e13037. doi: 10.1111/acel.13037. Epub 2019 Sep 27. PMID: 31560162; PMCID: PMC6826123.