The Alzheimer’s Prevention Diet
By Patrick Holford
Does what you eat affect your risk for dementia later in life and, if so, what is the best diet to protect your brain and prevent cognitive decline? Many studies have been published with different results ranging from no effect at all, as reported in a study in Sweden[i], to over a 90% reduced risk of Alzheimer’s, as reported in a study in Finland and Sweden which compared those with the a ‘healthy’ versus unhealthy diet in mid-life for future risk of developing Alzheimer’s disease and dementia 14 years later. Those who ate the healthiest diet had an 86-90% decreased risk of developing dementia and a 90-92% decreased risk of developing Alzheimer’s disease.[ii] We have put together a science backed Alzheimer’s Prevention Diet.

Many of these studies are similar in design, by looking at mid-life diet then tracking a group of people over time to see who does or doesn’t develop dementia or its most common type, Alzheimer’s disease. Many also look at some measure of coherence to a ‘Mediterranean’ diet, which usually means eating more fruit, vegetables, legumes, nuts and seeds, as well as more fish, less meat and sometimes some or more wine. Others compare to the standard recommendations for a ‘healthy’ diet made by the country’s authorities. Some foods or drinks could go either way. For example, some studies suggest coffee drinking might reduce risk, yet coffee increases homocysteine levels, which is a strong predictor of risk. Alcohol consumption, especially red wine, may reduce risk in moderation but possibly increase risk in excess.
Another way to answer the question regarding the best anti-dementia diet is to look at studies that have linked specific foods or drinks to risk of cognitive decline then build up the brain-friendly diet from there. These studies can also help define how much of the food or drink is optimal, or too much for those foods or drinks that increase risk.
Protective Foods
One of the first good studies was carried out in Norway more than a decade ago by Eha Nurk and Helga Refsum and colleagues in Norway.[iii] [iv] They found that:
Tea – the more you drink the better. The tea benefit has been confirmed more recently in a study in Singapore, with green tea being marginally better than black tea.[v] However, this benefit was not found in a UK Biobank study, which reported by tea and coffee drinking to be associated with worsening cognition compared to abstainers.[vi]
Chocolate – peaks at 10g, or about 3 pieces – and let’s say dark, 70%+ thus with less sugar is more likely to be better, as sugar is a strong indicator of cognitive decline. More recent studies giving cocoa, a rich source of flavanols, have shown improved cognition, possibly by improving circulation.[vii]
Wine – consumption reduced risk up to 125g a day, which is a small glass. A study in the British Medical Journal in 2018 showed that while abstinence increased risk by 48% having more than 14 units of alcohol a week, which is equivalent to a medium glass of wine every day, increases risk.[viii]
Grains and potatoes – reached a plateau at 100 to 150g a day, which is one or two servings max. High fibre bread was the most beneficial carb food. White bread increased risk. Fruit and veg – although the more you eat the better, benefits start to plateau at 500g a day, which is about five to six servings a day. Of individual vegetables, carrots, cruciferous vegetables and citrus fruit were the most positive as were mushrooms. A more recent study in the US found that those who ate 1.3 portions of green leafy vegetables a day, compared to less than one a week, had a dramatically slower decline in cognitive function, equivalent to being 11 years younger over a 10-year period. Berries are particularly protective, especially blueberries and strawberries.[ix]
Fish – is the most protective. Nurk’s study found a peak benefit at about 100g a day, which is one to two servings. A study of all studies by National Institutes of Health researcher, Beydoun, reported that eating fish once or more each week reduces risk of Alzheimer’s by a third compared with those who eat fish less than once a week.[x]
Olive oil and nuts – seem to be positive aspects associated with a Mediterranean diet.[xi] One study assigned people to a Mediterranean diet supplemented with either a litre a week of olive oil or 30g of nuts a day which is a small handful, versus a control diet with low fat and reported reduced cognitive decline with the extra olive oil or nuts. [xii]
Protective Diets
Early studies on the Mediterranean style diet reported that high adherence versus low adherence reduced risk of Alzheimer’s by a third.[xiii][xiv] A study which followed 2,000 people over 20 years found that adherence to what they defined as healthy diet which meant ‘modifying the quality of fats, increasing vegetable consumption, and decreasing salt and sugar consumption’ was associated with a halving of dementia risk. With the exception of sugar, no individual food predicted risk significantly.[xv]
But the problem with studies like this is the assumptions. In this case ‘modifying the quality of fats’ means using vegetable oils as opposed to margarine or butter and not eating the visible fat on meat. Vegetable oils is rather vague – it could be olive oil or something like sunflower oil. The assumption is that a low-fat diet might be beneficial, yet a high fat, low carb (HFLC) ketogenic diet appears to be protective.
A study in Holland reported ‘that better diet quality related to larger brain volume, grey matter volume, white matter volume, and hippocampal volume. High intake of vegetables, fruit, whole grains, nuts, dairy, and fish and low intake of sugar-containing beverages were associated with larger brain volumes.’[xvi]
Harmful Foods and Diets
Sugar – be it sucrose (white sugar) or fructose comes out consistently negative. Studies report poorer cognition associated with intake of sugar-sweetened beverages in adults (Ye 2011).
Animal studies show sucrose and fructose both impair cognition and brain health (Lakhan 2013) (Orr 2014) which is all consistent with the with the fact that diabetes is a risk factor for cognitive decline (see ‘Is Sugar Killing Your Brain’) and supported by recent human studies on blood glucose as a major predictor of Alzheimer’s and dementia later in life.[xvii]
Even so-called ‘high’ levels within the normal reference range for blood glucose are linked to decreased grey matter in the brain.[xviii]
The most recent and substantial study relates to ultra-processed foods following around 70,000 people over a decade. The more ultra-processed foods eaten the higher was the risk for both dementia, Alzheimer’s and vascular dementia.[xix] Replacing just 10 per cent of ultra-processed food by weight in one’s diet with an equivalent proportion of unprocessed or minimally processed foods was estimated to lower risk of dementia by 19%. So, get off the junk. Choose whole foods only.
What is it about what you eat that could be protective?
The best candidates are foods high in:
- Antioxidant vitamins (C and E)
- Fruit and vegetables
- Flavanols
- Vitamin D
- Fish and omega-3 fats
- Folate and other B vitamins including b12, only found in animal foods
- Phospholipids, found in eggs and fish
Apart from the studies above it is certainly logical to include choline rich foods sources, as a source for phospholipids. In animal studies, giving choline slows down Alzheimer’s disease development.[xx]
Also, consuming two tablespoons C-8 oil, a form of medium chain triglyceride, has been shown to enhance cognition in those with mild cognitive impairment and elevate neuronal energy derived from ketones both in those with MCI and Alzheimer’s.[xxi] Given the preponderance of neurons to prefer ketones to glucose for fuel, and the evidence for benefit, such dietary practices such as 18:6 (eating all food within a 6 hour window) or starting the day with a Hybrid Latté, almost carb-free, high in cacao, C8 oil and almonds from carb-free almond milk and almond butter or following a low carb, high fat (LCHF) ketogenic diet, which has been shown to have beneficial for those with Alzheimer’s,[xxii] should be considered.
Although in some respects conjectural calling on all this evidence, especially given the other health-promoting benefits of these foods, the key components of a diet designed to protect brain health and reduce risk of cognitive decline are:
Eat essential fats and phospholipids

- Eat an egg a day, or six eggs a week – preferably free-range, organic, and high in omega-3s. Boil, scramble or poach them, but avoid frying.
- Eat a tablespoon of seeds and nuts every day – the best seeds are chia, flax, hemp, pumpkin, higher in omega-3. They’re delicious sprinkled on cereal, soups, and salads. The best nuts are walnuts, pecans, and macadamia nuts. Each are high in omega-3 but all nuts, including almonds, hazelnuts and unsalted peanuts are good sources of protein and minerals.
- Eat cold-water, oily carnivorous fish – have a serving of herring, mackerel, salmon or sardines two or three times a week (limit tuna, unless identified as low in mercury, to three times a month). Vegans need to supplement algal omega-3 DHA, as well as choline or lecithin capsules or granules, rich in phosphatidyl choline.
- Use cold-pressed olive oil for salad dressings and other cold uses, such as drizzling on vegetables instead of butter. Substitute frying with steam frying with olive oil, coconut oil or butter, e.g. for onions and garlic, then adding a watery sauce such as lemon juice, tamari and water, to ‘steam’, for example, vegetables perhaps with tofu, fish or chicken.
Eat slow-release carbohydrates

- Eat wholefoods – whole grains, lentils, beans, nuts, seeds, fresh fruit, and vegetables – and avoid all white, refined and over-processed foods, as well as any food with added sugar.
- Snack on fresh fruit, preferably apples, pears and/or berries, especially blueberries.
- Eat less gluten. Try brown rice, rye, oats, quinoa, lentils, beans, or chickpeas.
- Avoid fruit juices. Eat fresh fruit instead. Occasionally have unsweetened Montmorency cherry juice or blueberry juice (made from unsweetened concentrate).
Eat antioxidant and vitamin-rich foods

- Eat half your diet raw or lightly steamed.
- Eat two or more servings a day of fresh fruit, including one of berries.
- Eat four servings a day of dark green, leafy and root vegetables such as tenderstem broccoli, broccoli, kale, spinach, watercress, carrots, sweet potatoes, Brussels sprouts, green beans, or peppers, as well as mushrooms. Choose organic where possible.
- Have a serving a day of beans, lentils, nuts, or seeds – all high in folate, as are peanuts.
Eat enough protein

- Have three servings of protein-rich foods a day, if you are a man, and two if you are a woman.
- Choose good vegetable protein sources, including beans, lentils, quinoa, tofu, or tempeh (soya) and ‘seed’ vegetables such as peas, broad beans and corn.
- If eating animal protein, choose lean meat or preferably fish, organic whenever possible.
Avoid harmful fats
- Minimise your intake of fried or processed food and burnt saturated fat on meat, and cheese.
- Minimise your consumption of deep-fried food. Poach, steam or steam-fry food instead.
Avoid sugar, reduce caffeine, and drink alcohol in moderation
- Avoid adding sugar to dishes and avoid foods and drinks with added sugar. Keep your sugar intake to a minimum, sweetening cereal or desserts with fruit.
- Avoid or considerably reduce your consumption of caffeinated drinks. Don’t have more than one caffeinated drink a day. Tea is preferable to coffee.
- Drink alcoholic drinks infrequently, and preferably red wine, to a maximum of one small glass (125g) a day.
- Have up to three slices of dark chocolate, minimum 70% cacao, or drink unsweetened cacao with milk or plant milk.

Help support Food for the Brain
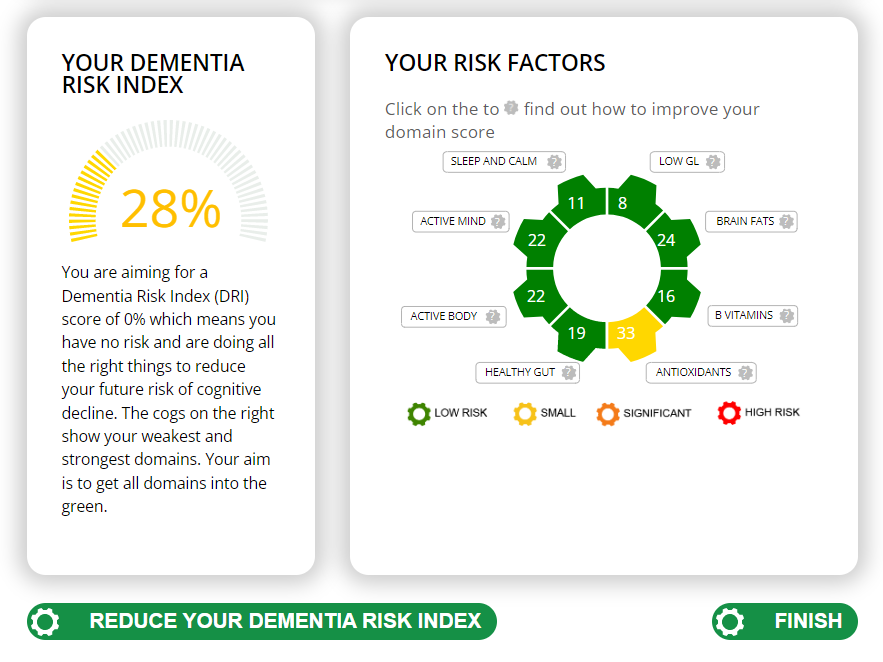
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
References
[i] Glans I, Sonestedt E, Nägga K, Gustavsson AM, González-Padilla E, Borne Y, Stomrud E, Melander O, Nilsson P, Palmqvist S, Hansson O. Association Between Dietary Habits in Midlife With Dementia Incidence Over a 20-Year Period. Neurology. 2022 Oct 12:10.1212/WNL.0000000000201336. doi: 10.1212/WNL.0000000000201336. Epub ahead of print. PMID: 36224029.
[ii] Eskelinen MH, Ngandu T, Tuomilehto J, Soininen H, Kivipelto M. Midlife healthy-diet index and late-life dementia and Alzheimer’s disease. Dement Geriatr Cogn Dis Extra. 2011 Jan;1(1):103-12. doi: 10.1159/000327518. Epub 2011 Apr 27. PMID: 22163237; PMCID: PMC3199886.
[iii] Nurk E, Refsum H, Drevon CA, Tell GS, Nygaard HA, Engedal K, Smith AD. Intake of flavonoid-rich wine, tea, and chocolate by elderly men and women is associated with better cognitive test performance. J Nutr. 2009 Jan;139(1):120-7. doi: 10.3945/jn.108.095182. Epub 2008 Dec 3. PMID: 19056649.
[iv] Nurk E, Refsum H, Drevon CA, Tell GS, Nygaard HA, Engedal K, Smith AD. Cognitive performance among the elderly in relation to the intake of plant foods. The Hordaland Health Study. Br J Nutr. 2010 Oct;104(8):1190-201. doi: 10.1017/S0007114510001807. Epub 2010 Jun 16. PMID: 20550741.
[v] Feng L, Chong MS, Lim WS, Lee TS, Kua EH, Ng TP. Tea for Alzheimer Prevention. J Prev Alzheimers Dis. 2015;2(2):136-141. doi: 10.14283/jpad.2015.57. PMID: 29231231.
[vi] Cornelis MC, Weintraub S, Morris MC. Caffeinated Coffee and Tea Consumption, Genetic Variation and Cognitive Function in the UK Biobank. J Nutr. 2020 Aug 1;150(8):2164-2174. doi: 10.1093/jn/nxaa147. PMID: 32495843; PMCID: PMC7398783.
[vii] Lamport DJ, Pal D, Moutsiana C, Field DT, Williams CM, Spencer JP, Butler LT. The effect of flavanol-rich cocoa on cerebral perfusion in healthy older adults during conscious resting state: a placebo controlled, crossover, acute trial. Psychopharmacology (Berl). 2015 Sep;232(17):3227-34. doi: 10.1007/s00213-015-3972-4. Epub 2015 Jun 7. PMID: 26047963; PMCID: PMC4534492.
[viii] Sabia S, Fayosse A, Dumurgier J, Dugravot A, Akbaraly T, Britton A, Kivimäki M, Singh-Manoux A. Alcohol consumption and risk of dementia: 23 year follow-up of Whitehall II cohort study. BMJ. 2018 Aug 1;362:k2927. doi: 10.1136/bmj.k2927. PMID: 30068508; PMCID: PMC6066998.
[ix] Devore E et al, ‘Dietary intakes of berries and flavonoids in relation to cognitive decline’, Annals of neurology 2012; 72: 135-43; Agarwal P, Holland TM, Wang Y, Bennett DA, Morris MC. Association of Strawberries and Anthocyanidin Intake with Alzheimer’s Dementia Risk. Nutrients. 2019 Dec 14;11(12):3060. doi: 10.3390/nu11123060. PMID: 31847371; PMCID: PMC6950087
[x] Beydoun MA, Beydoun HA, Gamaldo AA, Teel A, Zonderman AB, Wang Y. Epidemiologic studies of modifiable factors associated with cognition and dementia: systematic review and meta-analysis. BMC Public Health. 2014 Jun 24;14:643. doi: 10.1186/1471-2458-14-643. PMID: 24962204; PMCID: PMC4099157.
[xi] Román GC, Jackson RE, Reis J, Román AN, Toledo JB, Toledo E. Extra-virgin olive oil for potential prevention of Alzheimer disease. Rev Neurol (Paris). 2019 Dec;175(10):705-723. doi: 10.1016/j.neurol.2019.07.017. Epub 2019 Sep 11. PMID: 31521394.; Salis C, Papageorgiou L, Papakonstantinou E, Hagidimitriou M, Vlachakis D. Olive Oil Polyphenols in Neurodegenerative Pathologies. Adv Exp Med Biol. 2020;1195:77-91. doi: 10.1007/978-3-030-32633-3_12. PMID: 32468462.
[xii] Valls-Pedret C, Sala-Vila A, Serra-Mir M, Corella D, de la Torre R, Martínez-González MÁ, Martínez-Lapiscina EH, Fitó M, Pérez-Heras A, Salas-Salvadó J, Estruch R, Ros E. Mediterranean Diet and Age-Related Cognitive Decline: A Randomized Clinical Trial. JAMA Intern Med. 2015 Jul;175(7):1094-1103. doi: 10.1001/jamainternmed.2015.1668. Erratum in: JAMA Intern Med. 2018 Dec 1;178(12):1731-1732. PMID: 25961184.
[xiii] Singh B, Parsaik AK, Mielke MM, Erwin PJ, Knopman DS, Petersen RC, Roberts RO. Association of mediterranean diet with mild cognitive impairment and Alzheimer’s disease: a systematic review and meta-analysis. J Alzheimers Dis. 2014;39(2):271-82. doi: 10.3233/JAD-130830. PMID: 24164735; PMCID: PMC3946820.
[xiv] Scarmeas N, Stern Y, Tang MX, Mayeux R, Luchsinger JA. Mediterranean diet and risk for Alzheimer’s disease. Ann Neurol. 2006 Jun;59(6):912-21. doi: 10.1002/ana.20854. PMID: 16622828; PMCID: PMC3024594.
[xv] Sindi S, Kåreholt I, Eskelinen M, Hooshmand B, Lehtisalo J, Soininen H, Ngandu T, Kivipelto M. Healthy Dietary Changes in Midlife Are Associated with Reduced Dementia Risk Later in Life. Nutrients. 2018 Nov 3;10(11):1649. doi: 10.3390/nu10111649. PMID: 30400288; PMCID: PMC6265705.
[xvi] Croll PH, Voortman T, Ikram MA, Franco OH, Schoufour JD, Bos D, Vernooij MW. Better diet quality relates to larger brain tissue volumes: The Rotterdam Study. Neurology. 2018 Jun 12;90(24):e2166-e2173. doi: 10.1212/WNL.0000000000005691. Epub 2018 May 16. PMID: 29769374.
[xvii] Zhang X, Tong T, Chang A, Ang TFA, Tao Q, Auerbach S, Devine S, Qiu WQ, Mez J, Massaro J, Lunetta KL, Au R, Farrer LA. Midlife lipid and glucose levels are associated with Alzheimer’s disease. Alzheimers Dement. 2022 Mar 23. doi: 10.1002/alz.12641. Epub ahead of print. PMID: 35319157.
[xviii] Mortby ME, Janke AL, Anstey KJ, Sachdev PS, Cherbuin N. High “normal” blood glucose is associated with decreased brain volume and cognitive performance in the 60s: the PATH through life study. PLoS One. 2013 Sep 4;8(9):e73697. doi: 10.1371/journal.pone.0073697. PMID: 24023897; PMCID: PMC3762736.
[xix] Li H, Li S, Yang H, Zhang Y, Zhang S, Ma Y, Hou Y, Zhang X, Niu K, Borne Y, Wang Y. Association of Ultraprocessed Food Consumption With Risk of Dementia: A Prospective Cohort. Neurology. 2022 Jul 27:10.1212/WNL.0000000000200871. doi: 10.1212/WNL.0000000000200871. Epub ahead of print. PMID: 35896436.
[xx] Velazquez R, Ferreira E, Knowles S, Fux C, Rodin A, Winslow W, Oddo S. Lifelong choline supplementation ameliorates Alzheimer’s disease pathology and associated cognitive deficits by attenuating microglia activation. Aging Cell. 2019 Dec;18(6):e13037. doi: 10.1111/acel.13037. Epub 2019 Sep 27. PMID: 31560162; PMCID: PMC6826123.
[xxi] Fortier M, Castellano CA, St-Pierre V, Myette-Côté É, Langlois F, Roy M, Morin MC, Bocti C, Fulop T, Godin JP, Delannoy C, Cuenoud B, Cunnane SC. A ketogenic drink improves cognition in mild cognitive impairment: Results of a 6-month RCT. Alzheimers Dement. 2021 Mar;17(3):543-552. doi: 10.1002/alz.12206. Epub 2020 Oct 26. PMID: 33103819; PMCID: PMC8048678.
[xxii] Phillips MCL, Deprez LM, Mortimer GMN, Murtagh DKJ, McCoy S, Mylchreest R, Gilbertson LJ, Clark KM, Simpson PV, McManus EJ, Oh JE, Yadavaraj S, King VM, Pillai A, Romero-Ferrando B, Brinkhuis M, Copeland BM, Samad S, Liao S, Schepel JAC. Randomized crossover trial of a modified ketogenic diet in Alzheimer’s disease. Alzheimers Res Ther. 2021 Feb 23;13(1):51. doi: 10.1186/s13195-021-00783-x. PMID: 33622392; PMCID: PMC7901512.