—
Parkinson’s affects 120,000 people in the UK, both young and old.
A recent review from the NCBI in the US (1) on Parkinson’s disease begins with the following:
‘Parkinson’s disease (PD) is a common neurodegenerative disease for which there is no treatment modifying the course of the disorder and no reliable biomarkers for early diagnosis. (2) In just 26 years, the number of PD patients around the world has more than doubled. (3) A relatively conservative prediction model shows that it is expected that there will be 12 million PD patients in the world by 2050.’
Thus, early detection and timely intervention of PD appear to be particularly important.
Thanks to the pioneering work of Dr Geoffrey Leader and Lucille Leader, a doctor and nutritionist living in London, we now know that the right nutritional intervention can effectively support the symptoms of Parkinson’s disease.
—
Dopamine is a neurotransmitter (chemical messenger) found within the brain. It has a variety of influences on brain function including playing a role in regulation. (Fig 1) [4]
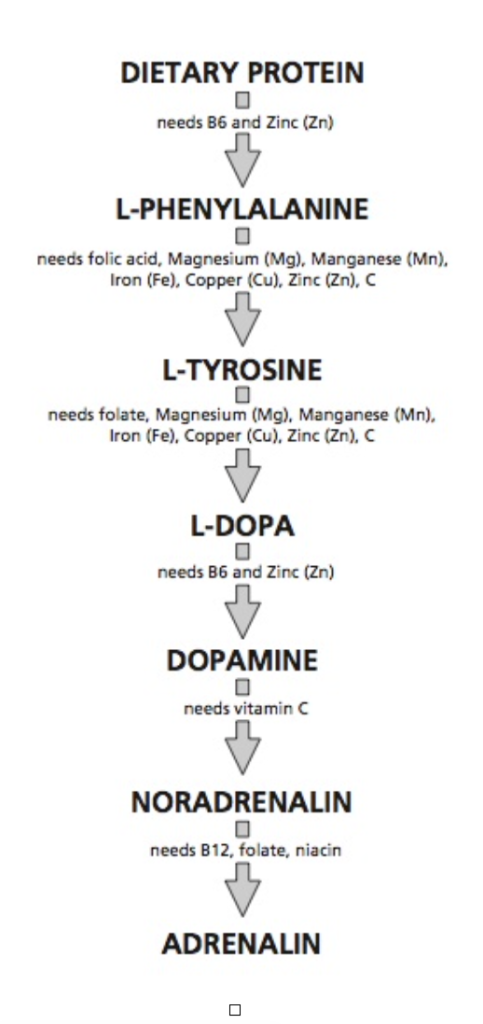
There is little doubt that dopamine deficiency is the major cause of the symptoms of Parkinson’s, and most drug therapy aims to improve the body’s ability to make dopamine from L-dopa. But, why do some people develop this impaired ability to make this key neurotransmitter?
There are many answers to this question.
In some cases the neurons that produce dopamine don’t work properly, sometimes because they lack the raw materials, or the enzymes that turn on the building blocks, amino acids. (Amino acids are commonly known as the building blocks of protein. There are 20 standard amino acids from which almost all proteins are made.) The neurons can die off or be damaged, for example by oxidants, or by environmental toxins such as pesticides and herbicides.
Interestingly, researchers at the University of Miami have found levels of these chemicals to be higher in the brains of Parkinson’s sufferers.[5] The incidence of Parkinson’s is notably higher in rural areas where a lot of crop spraying takes place, and some pesticide combinations have shown a clear geographical correlation with incidences of the disease.[6,7]
Deficiency of nutrients such as folate which is critical during pregnancy for the development of a baby’s brain and nerves and also essential for brain and nerve function, play a part, making these dopamine-producing brain cells more susceptible to damage.[8]
—
The balance of neurotransmitters, including dopamine, is controlled to a large extent by the process of methylation. (Methylation is what occurs when the body takes one substance and turns it into another, so that it can be detoxified and excreted from the liver.)
Most people with Parkinson’s have raised homocysteine levels. [9] Homocysteine is an amino acid found in the blood. Elevated levels of homocysteine have been associated with narrowing and hardening of the arteries and an increased level indicates disrupted methylation patterns. The latest review [10] states that “Homocysteine is linked with the occurrence and progression of Parkinson’s. This review briefly discussed the structure of Hcy, the metabolism of Hcy, and the mechanism of HHcy in PD. There are many disputes about the relationship between HHcy and PD which remain to be investigated. It also remains to be examined whether homocysteine is a causative agent or marker of damage.” Additionally,treatment with L-dopa medication tends to raise homocysteine levels.[11]
Either way, testing for homocysteine and supplementing homocysteine-lowering nutrients accordingly would be a recommendation. Buy your test kit here.
—
In addition to faulty methylation, sometimes there is a problem in how the body detoxifies, a job primarily done by the liver, leaving neurons unprotected.[12] Then there are other factors such as prolonged stress and the likelihood of genetic predispositions. Geoffrey and Lucille Leader figured that each of these pieces of the jigsaw puzzle could be made a lot better if sufferers followed a targeted optimum nutrition programme. They started to test patients with Parkinson’s disease and found that literally 100 percent of them had nutritional deficiencies based on tests that measure what is going on within cells. They also found that many were deficient in stomach acid and digestive enzymes. Digestive enzymes break down carbohydrates, fats and proteins into their smallest components, allowing them to be absorbed by the body. Examples of deficient digestive enzymes might look like poor digestion, and increased intestinal permeability, leading to faulty absorption of nutrients.
Intestinal permeability is easily tested by drinking a solution that shouldn’t pass through the gut wall, and then measuring urinary levels. Using such a test, people with Parkinson’s disease may often show an increase in gut permeability or evidence of malabsorption. While there is no conclusive evidence yet that Parkinson’s disease is caused by nutrient deficiencies, the Leaders have found that correcting these deficiencies often helps.
—
All this faulty digestion and absorption places extra stress on the liver, the detoxification capital of the body. Since the brain’s neurons can’t protect themselves from toxins, they depend on the liver. A simple example of this is alcohol – once you drink more than your liver can detoxify, you get drunk, which is what happens when brain cells are exposed to this toxin. In excess, you lose muscular control and movements, including speech, slow down.
Problems with liver detoxification are often a hallmark of Parkinson’s patients.
One of the liver’s best detox allies are the sulphur-containing amino acids, which have the ability to mop up undesirable toxins in a process called sulphation. Researchers have reported faulty sulphation in patients with Parkinson’s, which can be helped by supplementing cysteine, methionine and molybdenum. These can help rid the body of protein breakdown products, strengthen teeth and may help reduce the risk of tooth decay [13] .
Avoiding wine, coffee, certain cheeses and chocolate, all known inhibitors of sulphation [12] and eating foods rich in glucosinolates, such as broccoli, brussel sprouts, cabbage, cauliflower and kale, also help the liver to detoxify.
The greatest toxins of all are oxidants, or ‘free-radicals’. Giving antioxidants helps to prevent free radical damage to brain cells and slows the progression of the disease.
In a 7-year pilot study, 21 patients with early Parkinson’s were given 3,000mg of vitamin C and 3,200iu of vitamin E daily. The need for drug therapy was delayed up to two to three years compared to those who did not receive the antioxidants.[14]
Along with its negative effect on neurons, Parkinson’s also damages function in the mitochondria, which are the energy factories in our cells where energy conversion takes place. One of the most critical antioxidants for protecting mitochondria is coenzyme Q10 (CoQ10). The older you are, the more likely you are to be deficient.
These nutrients are some but by no means all of the allies that can support liver function, thereby preventing brain damage from toxins.. Dr Jeffrey Bland from Gig Harbor, Washington, an expert in liver detoxification, has also found tremendous improvement by supporting liver function with nutritional supplementation, increasing the effectiveness of drugs, reducing symptoms and boosting energy levels in those suffering from the early stages of Parkinson’s in studies.[15]
As detoxification may be compromised in Parkinson’s Disease, as is demonstrated by tests and clinical experience, personal clinical experience demonstrates that it is best to clean up the diet very gradually and recommend nutrients which support detoxification pathways.
—
The Leaders have found the best approach involves a tailor-made nutritional programme of diet and supplements and have found that this may often reduce symptoms and make drugs more effective, thus optimising dosage.
They recommend appropriate supplements based on patients’ biochemical individuality, including vitamins, minerals, essential fats, amino acids, antioxidants, phospholipids and brain-friendly herbs, providing that there are no contraindications for the administration of any herbs or nutrients for daily use, or in preparation or recovery from surgery.
As with so many mental health problems, controlling blood sugar and checking and correcting food allergies or intolerances can make a big difference. The most common allergy-provoking foods are the gluten grains (especially wheat, but also rye, oats, barley and spelt) and dairy products. Managing stress is also important because we respond to stress by producing the stress hormones noradrenalin and adrenalin, which are made from dopamine. This is why the symptoms of Parkinson’s often get worse when the sufferer is stressed.
—
The right diet is very important in tackling every piece of the jigsaw of Parkinson’s. Movement problems can get worse when dense proteins are eaten too close to the times of taking L-dopa medication.[16] This is because L-dopa competes with the amino acids for absorption at the receptor sites in the intestine and at the blood-brain barrier, so less gets through.
To make best use of the L-dopa, protein-rich foods containing the other amino acids should not be eaten at the same time as taking L-dopa medication, according to the following guidelines:
L-dopa medication and diet – what to eat when*
L-dopa is affected by protein-containing foods which contain significant amounts of the amino acids: tyrosine, phenylalanine, valine, leucine, isoleucine, tryptophan, methionine and histidine. Foods which contain these amino acids include eggs, fish, meat, poultry, dairy produce (not butter), pulses, green peas, spinach, sago, soy, couscous, bulgar, coconut, avocado, asparagus and gluten-containing grains (oats, rye, wheat, barley, spelt).
*This dietary protocol has been developed and proven helpful by Dr Geoffrey and Lucille Leader and is reproduced with their kind permission. (Their book, Parkinson’s Disease Optimising ON-OFF Periods during L-dopa Therapy www.denorpress.com) provides all the monitoring forms for patients and medical professions in order to assess more precise timing and dosage of administration – diet and metabolic pathways also presented.
Some people are more susceptible to this dose-dependent side-effect than others, and few react at a dose of 10mg, which is commonly given for Parkinson’s.[15]
While being careful to avoid these foods around medication, it is important to get enough protein from foods at other times. Good whole proteins include fish and eggs. Many people choose to have their meal containing concentrated protein at night. This is because they do not need as much help with movement control at night as during the day when their L-dopa medication is necessary to see them through all their activities. Some people leave out L-dopa completely after the protein meal. Otherwise, it is best to follow the time protocol for taking L-dopa with a protein-rich meal, as above.
It is also important to have a well-balanced diet throughout the day including fruits and vegetables, gluten-free wholegrains and plenty of fluids. A common problem in Parkinson’s is constipation. Having a diet rich in fruits and vegetables and drinking plenty of water throughout the day makes a big difference, as can a few prunes, figs or dried apricots between meals with water. There are also special fibres, such as glucomannan, which help relieve constipation.

Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
1 [https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10848096/pdf/CNS-30-e14420.pdf]
2 Surguchov A. In: Peplow PV, Martinez B, Gennarelli TA, eds. Neurodegenerative Diseases Biomarkers: Towards Translating Research to ClinicalPractice. Springer US; 2022:155-180.
3 GBD 2016 Neurology Collaborators. Global, regional, and national burden of neurological disorders, 1990–2016: a systematic anal- ysis for the global burden of disease study 2016. Lancet Neurol. 2019;18:459-480. doi:10.1016/S1474-4422(18)30499-X
4 V.L. Davidson and D.B. Sittman, Biochemistry: The National Medical Series for Independent Study, Harawl Publishing (1994), pp.477-8
5. L. Fleming et al., ‘Parkinsons’ disease and brain levels of organochlorine pesticides’, Ann Neurol, Vol 36(1), 1994, pp.100-3
6. M. Thiruchevlvam et al., ‘The Nigrostriatal Dopaminergic System as a preferential target of repeated exposures to combined paraquat and maneb: implications for Parkinson’s Disease’, Journal of Neuroscience, Vol 20(24), 2000, pp.9207-14 and J. Corell et al., ‘The risk of Parkinson’s disease with exposure to pesticides, farming, well water and rural living’, Neurology, Vol 67, 1998, pp.1210-18
7. L. Leader, Parkinson’s Disease – The Way Forward, Denor Press (2000), p.77
8. W. Duan et al., ‘Dietary folate deficiency and elevated homocysteine levels endanger dopaminergic neurons in models of Parkinson’s Disease’, J Neurochemistry, vol 80, 2002, pp.101-10
9. Zhou L. Homocysteine and Parkinson’s disease. CNS Neurosci Ther. 2024 Feb;30(2):e14420. doi: 10.1111/cns.14420. Epub 2023 Aug 29. PMID: 37641911; PMCID: PMC10848096; see also
10. Zhou L. Homocysteine and Parkinson’s disease. CNS Neurosci Ther. 2024 Feb;30(2):e14420. doi: 10.1111/cns.14420. Epub 2023 Aug 29. PMID: 37641911; PMCID: PMC10848096; see also
S. Hassin-Baer et al., ‘Plasma homocysteine levels and Parkinson’s disease: Disease progression, carotid intima-media thickness and neuropsychiatric complications’, Clin Neuropharmacol, Vol 29(6), 2006, pp. 305-11
11.R.B. Postuma et al., ‘Vitamins and entacapone in levodopa-induced hyperhomocysteinemia: A randomized controlled study’, Neurology, Vol 66(12), 2006, pp. 1941-3
12. L. M. de Lau et al., ‘Dietary folate, vitamin B12, and vitamin B6 and the risk of Parkinson’s disease’, Neurology, Vol 67(2), 2006, pp. 315-8
13. G.B. Steventon et al., ‘Plasma cysteine and sulphate levels in patients with motor neurone, Parkinson’s and Alzheimer’s Disease’, Neurosci Letts, Vol 110, 1990, pp.216-20
14. S. Fahn, ‘A pilot trial of high dose alpha-tocopherol and ascorbate in early Parkinson’s Disease’, Ann Neurol, Vol 32(S), 1992, pp.128-32
15. J.S. Bland and J.A. Bralley, ‘Nutritional upregulation of hepatic detoxification enzymes’, J Applied Nutrition, Vol 4, 1992, pp.3-15
16. R.B. D’Agostino et al., ‘Plasma homocysteine as a risk factor for dementia and Alzheimer’s disease’, N Engl J Med, Vol 346(7), 2002, pp. 476-83