Whether your goal is to protect your memory from getting worse, or enhance and optimise your mental acuity, you need three things.
The first is having the best ‘structure’ – that is building brain cells and their connections; then it’s about the best ‘function’ as in fuel supply; and ‘utilisation’ and the importance of having an active physical, social and intellectual lifestyle.
The thing about memory is that it is very subjective.
One person’s perception of how good their memory is will be very different from someone else. Many people, later in life, think their memory is getting worse, while for others, they choose the path of denial that anything is wrong, even when it’s becoming obvious to those around them. Yet the specific aspects of cognition that decline on the road to dementia can, in fact, be objectively mapped and measured decades before any diagnosis might occur and, most importantly, can enable us to ‘course correct’ if we are ready to take the right actions soon enough.
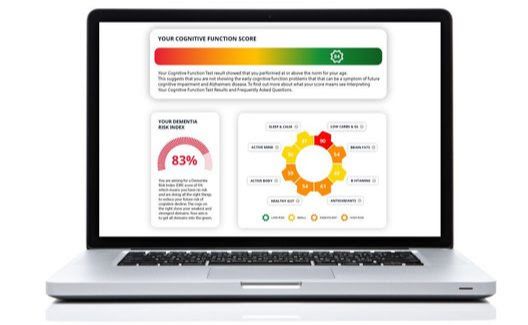
Many people who worry their memory is worse find that they score well into the healthy green zone. Only by having enough people of different ages completing the Cognitive Function Test, can we explore what is optimum and possible, to further improve, and what people with higher scores are doing differently to those with lower scores to stay in the green zone.
For example, if a person is aged 50 to 70, a score of 54 is the average expected score and we expect most respondents to score between 43 and 65. Scores below 43 and above 38 we classify as ‘amber’ or ‘at risk’ – that is not ideal. Below 38 is in the red zone and is consistent with mild cognitive impairment (MCI) sometimes called pre-dementia.
So, the first step to improving your memory is to take the Cognitive Function Test, and complete the questionnaire that follows, to find out which bits of your brain could benefit from an MOT and some proverbial ‘bodywork’. It will give you the very best road map to improve those areas that are not serving you well, while keeping up the bits that do work. This is what the COGNITION programme is all about.
We spend time and care looking after our cars – why not our minds and brains too?
The good news is, that there are some great shortcuts to improving your memory that you can start taking now.
Diana first took the Cognitive Function Test when she was 60.
“I‘ve been doing the Cognitive Function Test for about 10 years. I’m no longer worried that I’m losing my mental abilities.” Now, age 70, her cognitive function has improved. “In fact, my memory is better, my vocabulary has improved and I’m no longer searching for that “right” word – it’s springing to mind much more readily. People are even complimenting me on my great memory whereas in the past, I used to joke that I had the memory retention of a goldfish. Doing the test annually has given me confidence that ageing and Alzheimer’s are not to be feared and has played a significant role in reinforcing the lifestyle changes I’ve made.”
The B vitamin – Omega-3 Dynamic Duo
The first, relating to how we build neurons and their connections, is the dynamic duo of homocysteine-lowering B vitamins and omega-3 fats, especially DHA.
Homocysteine is an amino acid and B vitamins play a crucial role in breaking down homocysteine into other chemicals your body needs.
In trials, participants with memory problems were given homocysteine-lowering B vitamins and had a massive 73% reduction in the annual rate of brain shrinkage compared to those on a dummy placebo pill. Another trial, giving just 2.3 grams of omega-3 fish oils to participants (who already had adequate B vitamin status) produced a halving of the participant’s clinical dementia rating (CDRsob), and an improvement in their memory on the mini-mental state exam (MMSE). Omega 3 is vital to keep our brain membranes fluid and supports the action of neurotransmitters (our brain’s chemical couriers) so the combination is a clear freeway to better brain health.
So what levels are optimal? Getting your omega-3 index above 8%, whether by eating fish or supplementing with capsules, is a good starting point. Psychiatrist Joe Hibbeln gives 4 grams a day – that’s four large fish oil capsules. Also, higher homocysteine levels (above 7 to 7%) indicate that your body needs more B vitamins to break down the amino acids. A broad spectrum supplement that includes B12, folate, B6, TMG, zinc and NAC is a great option.
Up Antioxidants
The next stop on the brain upgrade road trip is to fill up on those antioxidants. Two of the key antioxidants in your body are glutathione and melatonin. They help detox the brain and play an important role in protecting the brain from ‘free radicals’, a byproduct of energy production. Think of antioxidants as the ‘fuel filter’ for your brain.
Glutathione is made from NAC (N-acetylcysteine), an amino acid that should be included in your homocysteine-lowering formula. It is also ‘recycled’ by anthocyanins – that’s all those blue/red foods, such as blueberries, green leafy vegetables like spinach, and dark chocolate, while onions, asparagus and eggs are rich in glutathione. You could aim to have a serving of berries every day, but also supplement glutathione or NAC.
Having sufficient melatonin is a product of both your serotonin status, made from tryptophan or 5-HTP, and getting good quality sleep. If you have a neurodegenerative disease, cognitive impairment, high stress or poor sleep, and especially if you have more than one of these, supplementing 1 to 5mg of melatonin every night, the higher level being for those with sleeping problems, may have anti-ageing benefits for the brain (1).
Don’t Forget Niacin
One B vitamin that has a benefit for your memory is Vitamin B3, in the form of niacin. In animal studies, the combination of melatonin and NMN (nicotinamide mononucleotide, also in the family of vitamin B3) has been shown to protect the central hippocampus area of the brain, slowing down ageing, improving mitochondrial energy production and cognition (2). They are the hot new nutrients in brain research, with the potential to protect against amyloid and p-tau formation, two key markers of brain degeneration.
In a long-term study looking at nutrient levels in people aged 18 to 30, then measuring their memory 25 years later, niacin intake most predicted better memory, followed by folate, B6 and B12 (3). Another study found niacin intake protects against Alzheimer’s. Those with higher niacin intakes had a third of the risk (4) than those with lower intakes.
A small study giving supplements of niacin at a dose of 141 mg (which is almost ten times the basic ‘nutrient reference value’ of 16mg), produced measurable improvement in memory in eight weeks in healthy people without cognitive decline (5).
I hedge my bets and supplement 50mg daily in my multivitamin.
Fill the Energy Gap with C8 oil
In previous articles, we have explained how the brain loves ketones as fuel, primarily derived from a specific type of medium-chain triglyceride (MCT) called C8 oil. The main sources of C8 oil are coconut, palm oil, butter and milk, though coconut is the most common, containing about 7% C8 oil.
People with blood sugar problems such as diabetes, as well as many older people, become less able to get sufficient glucose (the other critical brain fuel), into the brain’s mitochondrial energy factories within neurons and end up with a brain energy deficit. Filling this energy gap with one or two tablespoons (15-30 g) of C8 oil is a quick win for increased brain energy.
This has proven to work in those with cognitive decline, thanks to the excellent research of Professor Stephen Cunnane. Four out of six studies have shown improvements in memory from MCT oil supplementation in those without dementia (6). And the benefits are there if you’re younger and healthier too. One study at Liverpool Hope University giving healthy young adults between 12-18 g of C8/C10 in combination found cognitive improvements in just three weeks.
To support memory, start with a tablespoon of C8 oil a day for younger, healthier people, or twice this if you’re older, are already experiencing some cognitive decline, or have blood sugar problems, such as a raised HBA1c level above 6% or 53 nmol/mol.
The other way to boost your brain with ketones is to eat a low-carb high-fat diet or do intermittent fasting. I recommend two or three days a week doing ‘18:6’ (18 hours fasting, six hours eating). After your last evening meal, fast until lunch the next day, but start your day with a Hybrid Latté containing a tablespoon of C8 oil. Your brain is more likely to convert the C8 to ketones if you are ‘starved’ of carbohydrates in this way.
Vitamin D protects your brain and memory
Vitamin D is considered a true all rounder as far as your brain and mental health is concerned and it’s worth ensuring your level is optimal for both brain and body. It helps neurotransmission and exerts anti-inflammatory and neuroprotective activities within the brain by reducing inflammation and oxidative stress (8), both of which are drivers of cognitive decline.
Vitamin D deficiency increases the risk of Alzheimer’s (9). In a study in France involving 912 elderly patients followed for twelve years, a total of 177 dementia cases occurred. Those with low vitamin D levels had a nearly three-fold increased risk of Alzheimer’s (10).
Supplements may also help ward off dementia, according to a recent, large-scale study involving over twelve thousand dementia-free 70+ year olds in the US (12). More than a third (37%) took supplements of vitamin D. Those who did had a 40% lower incidence of dementia. Professor Zahinoor Ismail, of the University of Calgary and University of Exeter, who led the research, said: “We know that vitamin D has some effects in the brain that could have implications for reducing dementia, however so far, research has yielded conflicting results. Overall, we found evidence to suggest that earlier supplementation might be particularly beneficial, before the onset of cognitive decline.”
So what is considered a ‘good’ level? Ideally, a blood level above 75 nmol/l (30 ng/ml) is recommended, which usually means supplementing 3,000 iu during the winter months (October to March for those in the Northern hemisphere) and up to 1,000iu in the summer months depending on your sun exposure. But even supplementing just 800 iu (20 mcg) a day for 12 months has been shown to improve cognitive function (11). And we also have an at-home Vitamin D research project you can join here by simply testing your vitamin D with us.
Mushrooms and Your Mind
Various plants and fungi have positive effects on memory that are worth knowing about.
Those that stand out are the oldest living tree Ginkgo biloba and the fungus Lion’s Mane. A trial in healthy adults given Gingko for 30 days showed memory improvements. Ginkgo is a potent antioxidant, anti-inflammatory and neuroprotective compound (13). The usual doses given are 120–300 mg of standardized Ginkgo biloba. It slightly thins the blood so should be used with caution for those on blood thinners. It’s an optional extra.
Lion’s Mane has been shown to improve aspects of memory and cognitive function in three trials, on healthy volunteers (14), those with mild cognitive impairment (15) and dementia (16).
The best-researched mushroom, used for thousands of years in Japan as an anti-ageing compound, is Reishi. It is a potent antioxidant, thus protecting the brain from damage (17). Many people in Japan take it on a daily basis.
There are other brain-friendly plant remedies that fall more into the ‘stimulant’ category.
Maca root from Peru (18), Ginseng, Siberian Ginseng (Eleutherococcus)and Rhodiola are other potentially brain-friendly plants, perhaps best used by those with low brain energy, mental fatigue or high stress as they have effects on stress hormones and may support stress resilience. Some stimulating supplements (see Resources) use combinations of these.
There are others, such as guarana, whose main active ingredient is caffeine. I’m not so keen on these as caffeine ultimately causes downregulation, making you less responsive to your own adrenal hormones. In this way, the more you have the more you need.
Keeping our brains healthy is a lifelong journey that changes with the different stages of life. And just like a road trip, we can sometimes get lost. The good news is, we can get back on track. Knowing where we are is key, and Food for the Brain is there to support you on your way. Here are some simple things you can do today to begin to rebuild your brain and protect your precious memories along the ride.
Thank you for reading!
Food for the Brain is a non-for-profit educational and research charity that offers a free Cognitive Function Test and assesses your Dementia Risk Index to be able to advise you on how to dementia-proof your diet and lifestyle.
By completing the Cognitive Function Test you are joining our grassroots research initiative to find out what really works for preventing cognitive decline. We share our ongoing research results with you to help you make brain-friendly choices.
Please support our research by becoming a Friend of Food for the Brain.
1 Martín Giménez VM, de Las Heras N, Lahera V, Tresguerres JAF, Reiter RJ, Manucha W. Melatonin as an Anti-Aging Therapy for Age-Related Cardiovascular and Neurodegenerative Diseases. Front Aging Neurosci. 2022 Jun 3;14:888292. doi: 10.3389/fnagi.2022.888292. PMID: 35721030; PMCID: PMC9204094.
2 Read https://www.lifespan.io/topic/melatonin-benefits-side-effects/; also seeHosseini L, Farokhi-Sisakht F, Badalzadeh R, Khabbaz A, Mahmoudi J, Sadigh-Eteghad S. Nicotinamide Mononucleotide and Melatonin Alleviate Aging-induced Cognitive Impairment via Modulation of Mitochondrial Function and Apoptosis in the Prefrontal Cortex and Hippocampus. Neuroscience. 2019 Dec 15;423:29-37. Doi: 10.1016/j.neuroscience.2019.09.037. Epub 2019 Oct 31. PMID: 31678348.
3 Qin B, Xun P, Jacobs DR Jr, Zhu N, Daviglus ML, Reis JP, Steffen LM, Van Horn L, Sidney S, He K. Intake of niacin, folate, vitamin B-6, and vitamin B-12 through young adulthood and cognitive function in midlife: the Coronary Artery Risk Development in Young Adults (CARDIA) study. Am J Clin Nutr. 2017 Oct;106(4):1032-1040. doi: 10.3945/ajcn.117.157834. Epub 2017 Aug 2. PMID: 28768650; PMCID: PMC5611785.
4 Morris MC, Evans DA, Bienias JL, Scherr PA, Tangney CC, Hebert LE, Bennett DA, Wilson RS, Aggarwal N. Dietary niacin and the risk of incident Alzheimer’s disease and of cognitive decline. J Neurol Neurosurg Psychiatry. 2004 Aug;75(8):1093-9. doi: 10.1136/jnnp.2003.025858. PMID: 15258207; PMCID: PMC1739176.
5 Loriaux SM, Deijen JB, Orlebeke JF, De Swart JH. The effects of nicotinic acid and xanthinol nicotinate on human memory in different categories of age. A double blind study. Psychopharmacology (Berl). 1985;87(4):390-5. doi: 10.1007/BF00432500. PMID: 3936095.
6 Giannos, P., Prokopidis, K., Lidoriki, I. et al. Medium-chain triglycerides may improve memory in non-demented older adults: a systematic review of randomized controlled trials. BMC Geriatr 22, 817 (2022). https://doi.org/10.1186/s12877-022-03521-6
7 Jake S. Ashton, James W. Roberts, Caroline J. Wakefield, Richard M. Page, Don P.M. MacLaren, Simon Marwood, James J. Malone, The effects of medium chain triglyceride (MCT) supplementation using a C8:C10 ratio of 30:70 on cognitive performance in healthy young adults, Physiology & Behavior, Volume 229, 2021, 113252, ISSN 0031-9384, https://doi.org/10.1016/j.physbeh.2020.113252.
8 Jayedi A, Rashidy-Pour A, Shab-Bidar S. Vitamin D status and risk of dementia and Alzheimer’s disease: A meta-analysis of dose-response †. Nutr Neurosci. 2019 Nov;22(11):750-759. doi: 10.1080/1028415X.2018.1436639. Epub 2018 Feb 15. PMID: 29447107
9 Chai B, Gao F, Wu R, Dong T, Gu C, Lin Q, Zhang Y. Vitamin D deficiency as a risk factor for dementia and Alzheimer’s disease: an updated meta-analysis. BMC Neurol. 2019 Nov 13;19(1):284. doi: 10.1186/s12883-019-1500-6. PMID: 31722673; PMCID: PMC6854782.
100 Jia J, Hu J, Huo X, Miao R, Zhang Y, Ma F. Effects of vitamin D supplementation on cognitive function and blood Aβ-related biomarkers in older adults with Alzheimer’s disease: a randomised, double-blind, placebo-controlled trial. J Neurol Neurosurg Psychiatry. 2019 Dec;90(12):1347-1352. doi: 10.1136/jnnp-2018-320199. Epub 2019 Jul 11. PMID: 31296588.
111 Feart C, Helmer C, Merle B, Herrmann FR, Annweiler C, Dartigues JF, Delcourt C, Samieri C. Associations of lower vitamin D concentrations with cognitive decline and long-term risk of dementia and Alzheimer’s disease in older adults. Alzheimers Dement. 2017 Nov;13(11):1207-1216. doi: 10.1016/j.jalz.2017.03.003. Epub 2017 May 16. PMID: 28522216.
12Ghahremani M, Smith EE, Chen HY, Creese B, Goodarzi Z, Ismail Z. Vitamin D supplementation and incident dementia: Effects of sex, APOE, and baseline cognitive status. Alzheimers Dement (Amst). 2023 Mar 1;15(1):e12404. doi: 10.1002/dad2.12404. PMID: 36874594; PMCID: PMC9976297.
13 Stough C, Clarke J, Lloyd J, Nathan PJ. Neuropsychological changes after 30-day Ginkgo biloba administration in healthy participants. Int J Neuropsychopharmacol. 2001 Jun;4(2):131-4. doi: 10.1017/S1461145701002292. PMID: 11466162. ; see also Mix JA, Crews WD Jr. A double-blind, placebo-controlled, randomized trial of Ginkgo biloba extract EGb 761 in a sample of cognitively intact older adults: neuropsychological findings. Hum Psychopharmacol. 2002 Aug;17(6):267-77. doi: 10.1002/hup.412. PMID: 12404671.
15 Mori K, Inatomi S, Ouchi K, Azumi Y, Tuchida T (2009) Improving effects of the mushroom
Yamabushitake (Hericium erinaceus) on mild cognitive impairment: a double-blind placebo-
controlled clinical trial. Phytotherapy Research 23, 367-372.
16 Li IC, Chang HH, Lin CH, et al. Prevention of Early Alzheimer’s Disease by Erinacine A-Enriched Hericium erinaceus Mycelia Pilot Double-Blind Placebo-Controlled Study. Front Aging Neurosci. 2020;12:155. Published 2020 Jun 3. doi:10.3389/fnagi.2020.00155.
17 Huang, S., Mao, J., Ding, K., Zhou, Y., Zeng, X., Yang, W., Wang, P., Zhao, C., Yao, J., Xia, P., & Pei, G. (2017). Polysaccharides from Ganoderma lucidum Promote Cognitive Function and Neural Progenitor Proliferation in Mouse Model of Alzheimer’s Disease. Stem cell reports, 8(1), 84–94. https://doi.org/10.1016/j.stemcr.2016.12.007
19 Yahn GB, Leoncio J, Jadavji NM. The role of dietary supplements that modulate one-carbon metabolism on stroke outcome. Curr Opin Clin Nutr Metab Care. 2021 Jul 1;24(4):303-307. doi: 10.1097/MCO.0000000000000743. PMID: 33631772; see also
20 Marek K, Cichoń N, Saluk-Bijak J, Bijak M, Miller E. The Role of Vitamin D in Stroke Prevention and the Effects of Its Supplementation for Post-Stroke Rehabilitation: A Narrative Review. Nutrients. 2022 Jul 4;14(13):2761. doi: 10.3390/nu14132761. PMID: 35807941; PMCID: PMC9268813.
21 Jadavji NM, Emmerson JT, MacFarlane AJ, Willmore WG, Smith PD. B-vitamin and choline supplementation increases neuroplasticity and recovery after stroke. Neurobiol Dis. 2017 Jul;103:89-100. doi: 10.1016/j.nbd.2017.04.001. Epub 2017 Apr 7. PMID: 28396257.
22 Dimpfel W., Wedekind W., Keplinger I. Efficacy of dimethylaminoethanol (DMAE) containing vitamin-mineral drug combination on EEG patterns in the presence of different emotional states. Eur. J. Med. Res. 2003;8:183–191. [PubMed] [Google Scholar]
23 Sergio W. Use of DMAE (2-dimethylaminoethanol) in the induction of lucid dreams. Med. Hypotheses. 1988;26:255–257. doi: 10.1016/0306-9877(88)90129-6. [PubMed] [CrossRef] [Google Scholar]
24 Baumgaertel A. Alternative and Controversial Treatments for Attention-Deficit/Hyperactivity Disorder. Pediatr. Clin. N. Am. 1999;46:977–992. doi: 10.1016/S0031-3955(05)70167-X. [PubMed] [Google Scholar]
25 Lewis J.A., Young R. Deanol and methylphenidate in minimal brain dysfunction. Clin. Pharm. Therap. 1975;17:534–540. doi: 10.1002/cpt1975175534. [PubMed] [Google Scholar]
26 Moldavan M, Grygansky AP, Kolotushkina OV, Kirchhoff B, Skibo GG, Pedarzani P (2007) Neurotropic and trophic action of Lion’s Mane mushroom Hericium erinaceus (Bull.: Fr.) Pers. (Aphyllophoromycetideae) extracts on nerve cells in vitro. International Journal of Medicinal Mushrooms 9, 15-28; see also Yadav SK, Ir R, Jeewon R, Doble M, Hyde KD, Kaliappan I, Jeyaraman R, Reddi RN, Krishnan J, Li M, Durairajan SSK. A Mechanistic Review on Medicinal Mushrooms-Derived Bioactive Compounds: Potential Mycotherapy Candidates for Alleviating Neurological Disorders. Planta Med. 2020 Nov;86(16):1161-1175. doi: 10.1055/a-1177-4834. Epub 2020 Jul 14. PMID: 32663897.
Further info